End-to-End RCM Services for Healthcare Providers: Optimize Prior Authorization, Coding & Billing
At EliteMed Financials, we transform your revenue cycle with a proven 3-pillar approach:
Insurance Eligibility Verification → Medical Coding → Medical Billing.
Reduce denials by 65% and accelerate cash flow – focus on patients, not paperwork.
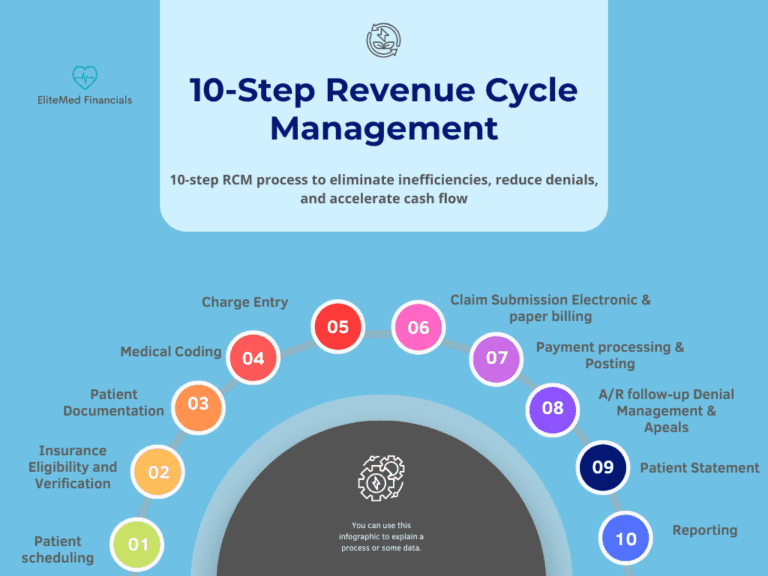
Our 3-Pillar RCM Methodology for Healthcare Providers
Eligibility Verification
Prevent denials at the source with error-free scheduling, documentation, and eligibility checks. This includes Patient Scheduling, Insurance Eligibility, and Patient Documentation.
Medical Coding
AAPC-certified coders ensure compliance with ICD-10/CPT coding to minimize claim rejections. The key focus is coding audits and denial prevention.
Medical Billing
From charge entry to denial management, we ensure faster reimbursements. Includes: Charge Entry, Claim Submission, Denial Management.
The 10 Steps of RCM We Perfect for Your Practice
Every dollar counts in healthcare. Here’s how our RCM services for healthcare providers optimize your revenue cycle from start to finish:
Patient Scheduling
- Automate appointments
- Reduce no-shows with SMS reminders
- Sync with EHR
- Optimize Workflow
Insurance Eligibility
- Instant Coverage Checks
- Pre-Authorization Alerts
- Benefit Details
- Patient Alerts
Patient Documentation
- Digital Intake Forms
- Error Scans
- EHR Integration
- Audit Trails
Medical Coding
- ICD-10/CPT codes based on clinical notes
- Compliance Audits
- CDI Support
- Ongoing Training
Charge Entry
- Real-Time Scrubbing
- Duplicate Checks
- Fee Schedule Sync
- Audit-Ready Logs
Claim Submission
- Electronic Claims
- Paper Claims
- Payer Rules Engine
- Real-Time Tracking
Payment Posting
- Auto-Posting
- Denial Alerts
- Patient Balances
- Daily Reports
A/R Follow-Up
- Aging Analysis
- Payer Follow-Up
- Adjustment Tracking
- Performance Metrics
Denial Management
- Root-Cause Analysis
- Auto-Appeals
- Payer Disputes
- Preventive Alerts
Patient Statements
- Simplified Billing
- Payment Plans
- Text/Email Alerts
- Dispute Resolution
Why EliteMed’s RCM Services Outperform In-House Teams
Advanced Technology: Real-time eligibility checks, denial trend analysis, and automated workflows without AI dependency.
Certified Experts: AAPC-certified coders, HIPAA-trained staff, and CMS compliance specialists.
Proven Results:
98% Clean Claim Rate | 30% Faster Reimbursements | 65% Fewer Denials
Trusted by 50+ Healthcare Providers
Certifications:
AAPC | Google Premier Partner | HIPAA Compliant
Certified Experts: AAPC-certified coders (Medical Coding specialists), HIPAA-trained staff, and CMS compliance specialists.
Proven Results:
98% Clean Claim Rate | 30% Faster Reimbursements | 65% Fewer Denials
Client Success Story

RCM Services FAQs
The first step is patient scheduling, where we streamline appointments, reduce no-shows, and ensure accurate data collection. Proper scheduling sets the foundation for clean claims and faster reimbursements.
Costs vary based on practice size and needs, but most clinics see a 300% ROI through reduced denials and faster payments. Request a free audit for a customized quote
Most clients see a 20-30% reduction in denials within 30 days. Full revenue cycle optimization typically takes 60-90 days.
Yes. Our 10-step process and certified coders help clinics achieve a 98% clean claim rate, with denial rates as low as 2-4% for long-term clients.
Yes. Our Denial Management team maintains a 98% clean claim rate across clients.
Absolutely. We adhere to strict HIPAA guidelines, use encrypted systems, and train all staff annually
Ready to Optimize Your Revenue Cycle?
- 📞 Schedule a Free RCM Audit – Recover Lost Revenue in 30 Days
- 📩 Download Free ROI Calculator
- Explore all healthcare financial services