
Expert Wound Care Medical Billing & RCM for Clinics, Hospitals & Specialty Practices
Wound Care Billing Services That Maximize Your Reimbursements
EliteMed Financials delivers end-to-end wound care billing services — from certified coding and clean claim submission to aggressive denial management and AR recovery. Our specialized team handles Medicare wound care billing, commercial payer claims, and compliance monitoring so you can focus on healing patients, not chasing payments.
✅ 98% First-Time Payment Resolution Rate
✅ 95%+ Clean Claim Accuracy
✅ 15–25% Revenue Growth Within 90 Days
✅ 100% HIPAA & CMS Compliance
Who We Are
EliteMed Financials is a specialized wound care billing company trusted by clinics, outpatient centers, hospital wound care departments, and Healogics-affiliated practices across the country.
Our team of certified wound care billers and coders manages the full revenue cycle — from patient eligibility verification through final payment posting. We specialize in the unique challenges of wound care billing: depth-based debridement coding, skin substitute reimbursement, Medicare LCD compliance, and payer-specific authorization requirements.
When you outsource wound care billing to EliteMed, you get a dedicated team that understands the difference between 11042 and 97597 — and why that distinction matters for your bottom line.
→ Read our Complete Guide to Wound Care Billing Codes
Our certified billers and coders handle every aspect of wound care billing — including Medicare wound care billing, supplies billing, and outpatient wound care coding — ensuring accuracy, compliance, and profitability.
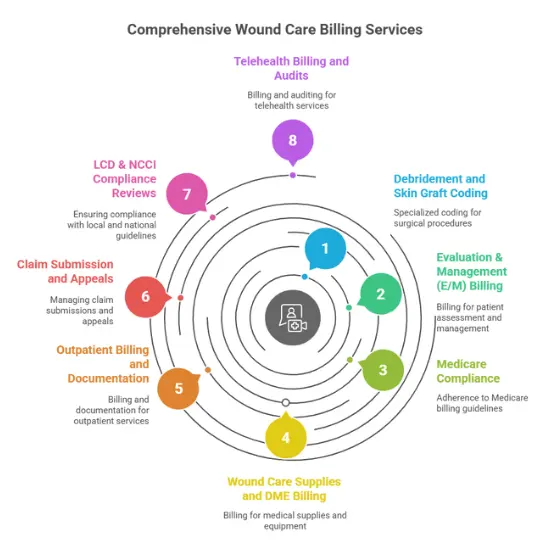
Comprehensive Wound Care Billing Services We Provide
We specialize in managing the unique complexities of wound care billing and coding, including:
Debridement and skin graft coding
Accurate CPT code selection for surgical debridement (11042-11047), active wound care (97597-97598), and skin substitute applications (15271-15278).
Prior Authorization Management
We handle prior auth for NPWT, advanced biologics, hyperbaric oxygen therapy, and other treatments requiring payer approval.
Medicare Wound Care Billing Compliance
Full LCD/NCD compliance, proper modifier usage, and documentation review to prevent Medicare denials and audit exposure.
AR Recovery & Collections
Systematic follow-up on aged receivables with average recovery of 20-30% on balances your in-house team has written off.
Claims Submission & Denial Management
24-48 hour claim turnaround, real-time rejection alerts, and aggressive appeals with 60%+ overturn rates on denied claims.
Compliance Auditing & Risk Prevention
Proactive chart audits, LCD compliance reviews, and OIG risk assessments to protect your practice from penalties.
Wound Care Supplies & DME Billing
Accurate HCPCS coding for dressings (A6021-A6233), NPWT equipment (E2402), and skin substitute products (Q4101-Q4255).
Analytics & Performance Reporting
Monthly KPI dashboards showing clean claim rates, denial patterns, AR aging, and revenue trends.
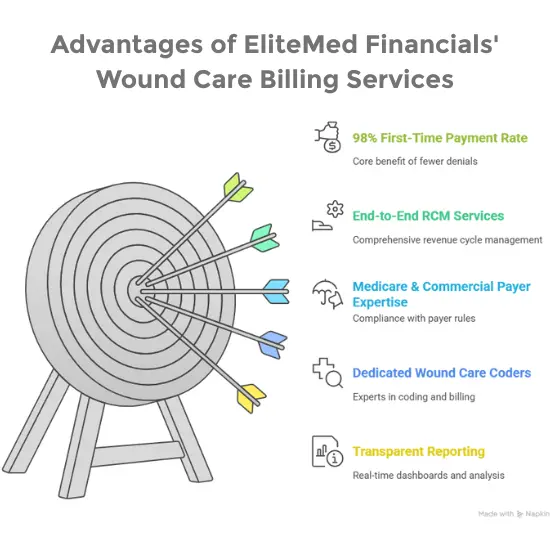
Why Choose Elitemed Financials for Wound Care Billing?
98% First-Time Payment Rate
Industry average is 70-80%. Our certified wound care coders achieve 98% clean claim rates — meaning faster payments and less rework.
Complete Revenue Cycle Management
From eligibility verification before treatment to final payment posting — we manage every step so nothing falls through the cracks.
Medicare & Commercial Payer Expertise
We stay current with CMS updates, MAC-specific LCDs, and commercial payer policies. When rules change, we adapt before it affects your revenue.
Dedicated Wound Care Billing Specialists
Not general medical billers. Your claims are handled by coders with CPC, CCS-P, and wound care certifications who understand debridement depth rules, LCD requirements, and skin substitute billing.
Aggressive Denial Management
We don't just resubmit denied claims — we analyze patterns, draft clinical appeals, and maintain 60%+ overturn rates. Average wound care practices see denials drop from 15%+ to under 5%.
Transparent, Real-Time Reporting
Access your dashboard 24/7. See clean claim rates, AR aging, denial reasons, and revenue trends. Monthly reviews with actionable insights.
Our Happy Clients!
Elitemed Financials transformed our wound care billing workflow. Our clean claim rate jumped to 98%, and collections improved within months.
Dr. Patricia Walker
Wound Care Specialist, Ohio
Their deep understanding of Medicare wound care billing and supply codes saved us hours every week. The support team is phenomenal!
James Foster
Director of Wound Management, Texas
Wound Care Billing Codes Our Team Masters
Our certified coders have deep expertise across all wound care billing codes — the CPT procedure codes, ICD-10 diagnosis codes, and HCPCS supply codes that determine whether your claims get paid or denied. Here's a quick overview of the code families we work with daily. **For complete code reference tables, decision trees, and coding scenarios, see our Complete Guide to Wound Care Billing Codes
CPT Codes for Wound Care Procedures
ICD-10 Diagnosis Codes for Wound Care
HCPCS Codes for Wound Care Supplies
Essential Modifiers for Wound Care Billing
Medicare Wound Care Billing Expertise You Can Trust

In-House vs. Outsourced Wound Care Billing
Many wound care practices debate whether to handle billing internally or partner with a specialized billing company. Here is an honest comparison to help you decide:
Factor | In-House Billing | Outsourced to EliteMed Financials |
Startup Cost | $50,000-$100,000+ (staff, software, training) | $0 setup fees |
Monthly Cost | $8,000-$15,000+ (salary, benefits, software) | Percentage of collections |
Wound Care Expertise | Varies – requires specialized training | Certified wound care coders |
Medicare Compliance | You manage LCD/NCD updates | We handle all compliance |
Denial Rate | Industry avg: 15-25% | Our rate: <5% |
Staff Turnover Risk | High – disrupts cash flow | Zero risk to you |
Scalability | Hire more staff = more cost | Scales automatically |
Technology | You purchase and maintain | Included in service |
Focus | Split between billing & patient care | 100% on patient care |
**Still Not Sure?**
→ Request a Free Side-by-Side Cost Analysis — We’ll compare your current billing costs to our service fees and show you the projected ROI.
Wound Care Billing Services for Every Practice Type
Wound Care Clinics & Centers
Dedicated wound care facilities handling chronic wounds, diabetic ulcers, and advanced treatments. We manage high-volume coding for debridement, NPWT, and skin substitutes
Hospital Outpatient Departments
Hospital-based wound care programs require specific billing rules for facility fees and professional services. We ensure proper HOPD billing compliance.
Physician Offices & Private Practices
Solo practitioners and group practices offering wound care as part of their services. We handle the complexity of mixed-specialty billing.
Home Health Agencies
Home-based wound care presents unique billing challenges. We manage Medicare home health claims including OASIS assessments and episode billing.
Skilled Nursing Facilities
SNF wound care billing requires understanding Part A consolidated billing and Part B carve-outs. We maximize reimbursement while ensuring compliance.
Long-Term Acute Care Hospitals (LTACHs)
Complex wound cases in LTACH settings need specialized coding expertise. We handle MS-DRG optimization and outlier billing.
Wound Care Subspecialties We Bill For:
Diabetic foot ulcer management
Pressure injury treatment
Venous and arterial ulcer care
Surgical wound complications
Burn wound management
Hyperbaric oxygen therapy
Common Wound Care Billing Questions
What are wound care billing services?
Wound care billing services handle the complete revenue cycle for wound treatment practices — including coding, claim submission, denial management, and AR recovery. Specialized services like ours focus exclusively on the unique challenges of wound care: depth-based debridement coding, Medicare LCD compliance, and skin substitute reimbursement.
Why should I outsource wound care billing instead of handling it in-house?
Wound care billing is uniquely complex — depth-based coding rules, MAC-specific LCDs, and high-cost supply billing require specialized expertise. In-house teams typically see 15-25% denial rates; our specialized team achieves under 5%. Plus, outsourcing eliminates staff turnover risk and lets your clinical team focus on patient care.
What size practices do you work with?
We serve solo wound care practitioners, multi-provider clinics, hospital outpatient departments, home health agencies, and SNFs. Our services scale to match your claim volume.
How much do your wound care billing services cost?
We offer flexible pricing: percentage of collections (typically 5-8%), per-claim fees, or flat monthly rates depending on your volume and needs. Most practices see 200%+ ROI within the first year through reduced denials and recovered revenue. [→ Request a custom quote](YOUR-CTA-LINK)
How long until I see results after switching to EliteMed?
Most practices see measurable improvements within 60-90 days: higher first-pass rates, reduced denial volume, and faster AR turnover. Full ROI (including recovered aged AR) typically occurs within 6-12 months.
Is wound care treatment covered by insurance?
Most health insurance plans — including Medicare, Medicaid, and commercial payers — cover medically necessary wound care when properly documented. Our team verifies coverage and handles prior authorizations to minimize out-of-pocket surprises for your patients.
What documentation do you need from our practice?
We need access to your EHR or superbills containing wound measurements (L×W×D), wound bed description, tissue types, treatments performed, and supplies used. We'll provide documentation templates if needed to ensure all billable elements are captured.
What is the Rule of 30, and how do you ensure compliance?
The Rule of 30 requires 30 days of documented conservative care before Medicare covers advanced wound therapies. We review documentation to ensure this requirement is met before submitting claims — preventing automatic denials.
How do you handle Medicare wound care billing compliance?
We monitor LCD requirements for your MAC region, verify Rule of 30 documentation for advanced therapies, ensure proper code sequencing, and prepare audit-ready documentation. Our Medicare wound care clients see 40%+ fewer denials than industry average.
Can you help recover old accounts receivable?
Yes. During onboarding, we analyze your aged AR and systematically work accounts over 60, 90, and 120 days. Practices typically recover 20-30% of balances they had essentially written off.
Explore Our Specialty Billing Services
We provide specialized medical billing and coding services for diverse healthcare specialties across the USA — helping practices improve collections, reduce denials, and stay compliant with payer requirements.
Comprehensive billing for psychiatrists, psychologists, and therapists. We handle session-based billing, telehealth claims, and prior authorizations with a 98% clean claim rate — ensuring your mental health practice gets paid faster.
Cardiology Billing Services
Accurate and streamlined claim submission for diagnostic and interventional cardiology procedures — ensuring error-free modifier and E/M coding.
Family Medicine Billing Services
Efficient billing workflows for preventive, chronic, and primary care visits — helping family practitioners maintain consistent cash flow and reduce aging A/R.
Internal Medicine Billing Services
End-to-end revenue cycle management tailored for multi-payer setups and chronic care coordination programs.
Urgent Care Billing Services
Rapid, high-volume billing solutions with real-time eligibility checks and transparent reporting dashboards for urgent care centers.
Pediatric Billing Services
Comprehensive billing for child wellness visits, vaccinations, and preventive care — ensuring accurate coding and timely payments.
Neurology Billing Services
Accurate billing for time-based visits, EEGs, and diagnostic services with detailed documentation review to minimize denials.
OB/GYN Billing Services
From global maternity billing to ultrasound coding and preauthorization management — supporting busy OB/GYN practices with precision.
Therapy Billing Services
Specialized in unit-based billing, modifier management, and multi-session tracking for therapy providers.
Ophthalmology Billing Services
Expert handling of both medical and vision claims, ensuring accurate surgical and diagnostic coding for ophthalmologists.
Podiatry Billing Services
Accurate billing for foot and ankle specialists — from wound care to orthotics — ensuring compliant coding and faster reimbursements.
DME Billing Services
Expert HCPCS coding and recurring claim tracking for DME billing.
We Also Supply Medicare-Covered Wound Care Grafts
Elite Med Financials is an authorized representative for DermaBind amniotic wound care grafts — Medicare Part B covered products for diabetic foot ulcers, venous leg ulcers, and pressure injuries. Every practice we enroll goes through our 3-Step IVR verification process — provider credentials, manufacturer FDA documentation, and patient insurance confirmed before every application.
When your graft supplier and billing partner are the same company, there is no gap between product compliance and claim accuracy. Every enrolled account receives our 6-Year Claims Protection — the only program of its kind in the wound care market — at no additional cost.
Schedule a Free Consultation with Elitemed Financials Today.
👉 Ready to Optimize Your Wound Care Billing?
Partner with Elitemed Financials for accurate, compliant, and revenue-driven wound care billing services. Let our team help you eliminate denials, increase reimbursements, and achieve a more predictable revenue cycle.

Wound Care Billing Services: Complete Guide to Streamlined Medical Billing & Coding in 2025
Introduction
Wound care billing services play a vital role in helping healthcare providers maintain financial stability while delivering quality patient care. As wound care becomes increasingly specialized—with advanced treatments like negative pressure wound therapy (NPWT), skin grafts, and chronic ulcer management—accurate billing and coding are no longer optional; they’re essential for compliance and revenue optimization.
In 2025, the landscape of medical billing for wound care is evolving rapidly. Between Medicare’s updated coverage policies, payer-specific documentation requirements, and ICD-10/CPT code complexities, wound care providers face a continuous challenge: how to achieve timely reimbursements while remaining compliant with regulatory standards.
That’s where specialized wound care billing services come in. These services are designed to streamline every step of the revenue cycle, from eligibility verification and coding accuracy to denial management and revenue recovery. By partnering with experienced medical billing companies that understand the nuances of wound care documentation, clinics can focus entirely on what matters most—patient healing and practice growth.
In this guide, we’ll explore everything you need to know about wound care billing, including its challenges, processes, technologies, and best practices for success in 2025.
Who Needs Wound Care Billing Services?
Wound care billing isn’t just for hospitals—it’s critical for a wide range of healthcare entities that provide wound treatment. These include:
- Wound care clinics and outpatient wound care centers
- Physician offices offering wound management as part of chronic disease care
- Home health agencies providing post-surgical or chronic wound treatment
- Skilled nursing facilities (SNFs) and rehabilitation centers
- Hospitals with specialized wound care departments
Each of these care settings handles diverse cases—from acute wounds to pressure ulcers and diabetic foot ulcers—requiring unique CPT, HCPCS, and ICD-10 codes for proper reimbursement.
The growing incidence of chronic wounds (affecting nearly 8 million Americans annually) has significantly increased the demand for accurate wound care medical billing services. With payers tightening documentation and coverage requirements, relying on generic billing staff or under-trained coders can result in claim denials, payment delays, and compliance risks.
In short, any provider delivering wound care procedures can benefit from outsourcing to a specialized wound care billing company that understands both payer rules and clinical documentation standards.
Understanding Wound Care Billing
Overview of Wound Care Treatments and Procedures
Wound care services cover a range of treatments, from basic dressing changes to advanced reconstructive procedures. Common procedures include:
- Debridement (CPT 97597–97598) for removing necrotic tissue
- Skin grafts and flaps (CPT 15100–15275)
- Negative pressure wound therapy (NPWT) (CPT 97605–97606)
- Hyperbaric oxygen therapy for chronic, non-healing wounds
- Compression therapy and offloading techniques for venous or diabetic ulcers
Each of these procedures requires precise documentation of wound size, depth, location, and healing stage, which directly influences billing codes and payment accuracy.
Improper or incomplete documentation remains one of the top causes of denials and underpayments in wound care billing.
Why Wound Care Billing Is Complex
Unlike general medical billing, wound care billing involves handling multiple coding layers per patient encounter. For instance, a single visit might include:
- Debridement (procedure code)
- Dressing supplies (HCPCS codes like A6203–A6224)
- Evaluation & management (E/M) codes
- Modifiers to indicate repeat procedures or wound location
In addition, payer-specific rules (like Medicare LCDs for wound care) require thorough documentation of medical necessity—including before-and-after photos, physician notes, and detailed wound progression reports.
Even small coding errors—such as missing modifiers, using outdated ICD-10 codes, or failing to link procedures with correct diagnoses—can lead to claim rejections or audit flags.
That’s why expert medical billers and certified wound care coders play such a crucial role. They ensure every claim is compliant, accurate, and timely, leading to optimized cash flow and higher collection rates.
Medicare, Medicaid, and Private Insurance in Wound Care Billing
Medicare wound care billing guidelines are particularly stringent. Providers must adhere to Local Coverage Determinations (LCDs) and National Coverage Determinations (NCDs) that specify which wound types and procedures qualify for reimbursement.
For example:
- Medicare requires documentation of prior treatments before approving advanced therapies like NPWT.
- Certain dressings and supplies are only covered if the wound meets chronic care definitions.
- Claims lacking proper modifiers (e.g., 59, 25, 76) are often automatically denied.
Meanwhile, private insurers and Medicaid programs have their own rules, which can vary across states like California, Virginia, Texas, and North Carolina. This variation makes payer compliance a critical aspect of successful wound care billing.
Importance of Documentation and Medical Necessity
Documentation forms the foundation of accurate wound care billing. Each wound treatment must clearly establish medical necessity, including:
- Wound type, size, and depth
- Underlying condition (e.g., diabetes, venous insufficiency)
- Physician evaluation notes
- Treatment plan and frequency
- Evidence of progress (healing measurements, photos)
Failure to establish medical necessity is among the top five causes of claim denials in wound care billing. According to recent audits, over 35% of wound care claims are initially denied due to documentation issues alone.
The Growing Need for Specialized Wound Care Billing Solutions
With the increasing complexity of payer rules, more practices are turning to specialized wound care billing solutions that combine human expertise with automation. These services manage everything from eligibility checks to A/R follow-ups using AI-powered tools, enabling faster payments and better compliance.
Partnering with expert wound care billing companies ensures:
- Higher first-pass resolution rates
- Reduced A/R days
- Enhanced compliance with Medicare and private payer rules
- Detailed reporting and analytics for practice insight
By leveraging wound care billing and coding services, providers not only minimize denials but also unlock growth opportunities through better revenue cycle management.
Step-by-Step Wound Care Billing Process
Wound care billing involves much more than submitting claims—it’s a complete Revenue Cycle Management (RCM) process designed to capture, code, and collect every dollar your wound care practice earns. A well-structured billing process minimizes denials, ensures Medicare wound care billing compliance, and enhances financial outcomes for both hospital-based and outpatient wound care centers.
Here’s a breakdown of each stage in the wound care billing workflow:
1. Patient Registration & Eligibility Verification
The foundation of accurate wound care billing begins with patient intake and insurance verification. Before rendering services, your billing team must confirm:
- Patient demographics and insurance details
- Eligibility for Medicare, Medicaid, or commercial plans
- Coverage for wound care supplies, debridement, and biologics
Failure to verify can result in 15–20% claim rejections. For instance, Medicare wound care billing guidelines require prior authorization for certain advanced wound treatments—missing this can delay payment.
2. Accurate Documentation & Clinical Notes
Proper documentation supports the billing codes used. Providers should clearly document:
- Wound location, size, depth, and type (pressure ulcer, diabetic ulcer, etc.)
- Frequency of treatment (as Medicare frequency guidelines strictly apply)
- Supplies used (e.g., dressings, grafts, negative pressure devices)
Incomplete notes or missing signatures are common reasons for medical necessity denials.
3. Medical Coding for Wound Care
This is the backbone of wound care medical billing. Coding specialists must correctly assign:
- ICD-10 codes for diagnosis (e.g., L97.411 – non-pressure chronic ulcer of right heel)
- CPT codes for procedures (e.g., 97597, 97598, 11042–11047 for debridement)
- HCPCS codes for wound care supplies
Outpatient wound care coding requires attention to modifiers (like -59 or -25) to prevent bundling issues. Many practices lose 30–40% of potential revenue due to coding errors or improper modifier usage.
4. Charge Entry and Review
Once the codes are assigned, charges are entered into the billing system. The accuracy of each claim depends on:
- Correct linking of diagnosis and procedure codes
- Validation of provider NPI and place of service (POS 11 for office, 22 for hospital outpatient)
- Checking Medicare Local Coverage Determinations (LCDs) for wound care
A good charge review process ensures claims pass payer-specific edits before submission.
5. Claim Submission
Clean claims are submitted electronically via clearinghouses or directly to payers. Any small mismatch—like a wrong payer ID or missing NPI—can lead to denials.
Automated claim scrubbing tools can reduce rejection rates by over 90% when configured for wound care-specific payer rules.
6. Payment Posting & EOB Reconciliation
After processing, the Explanation of Benefits (EOB) or Electronic Remittance Advice (ERA) is reviewed. Payments, adjustments, and denials are posted to patient accounts accurately.
This step provides insights into payer patterns and helps identify underpayments.
7. Denial Management & AR Follow-up
Even the best systems face claim denials—often due to coding inaccuracies, medical necessity issues, or missing modifiers.
Best practice includes:
- Denial categorization (technical vs. clinical)
- Root cause analysis
- Appeal with supporting clinical notes
A strong Accounts Receivable (AR) team should rework denied claims within 24–48 hours to maintain healthy cash flow.
8. Reporting, Analytics & Compliance
Finally, monthly RCM performance reports help providers track:
- Collection rates
- Days in AR
- First-time payment resolution rate (FTPR)
- Denial percentage per CPT
Regular audits ensure compliance with CMS wound care billing guidelines and prevent penalties.
Key Challenges in Wound Care Billing (and How to Solve Them)
The complexity of wound care billing often stems from the diversity of services, evolving Medicare coverage policies, and the need for precise documentation. Let’s look at the top challenges—and practical solutions that help overcome them.
Challenge 1: Frequent Policy Updates & Coding Changes
Medicare and private payers frequently update wound care billing codes and reimbursement policies. Keeping up with new guidelines like Medicare 2021 and 2024 updates can be overwhelming.
Solution:
Partner with an experienced wound care billing company that continuously tracks payer policy changes and updates coding workflows automatically. Regular training and compliance audits ensure your staff stays current.
Challenge 2: Documentation Errors and Lack of Medical Necessity
Many claims are denied because the documentation fails to support billed procedures, especially for debridement frequency or biologic applications.
Solution:
Implement EMR-integrated documentation templates that align with CMS wound care billing guidelines. Educate clinicians on documenting wound progress, dimensions, and justification for each service.
Challenge 3: Bundling and Modifier Confusion
Wound care often involves multiple services in one visit. Without the correct modifier (-59, -25, or -RT/LT), claims get bundled and underpaid.
Solution:
Use automated coding validation tools and maintain payer-specific modifier rules. Auditing your charge entry regularly can reduce bundling denials by 25%.
Challenge 4: Denials from Supply Billing
Billing for wound care supplies can be tricky—many payers have strict limits and documentation requirements. For example, Medicare DME guidelines define specific allowable dressing quantities per wound site.
Solution:
Establish a supply tracking system that links clinical notes, photos, and inventory logs. Always bill supplies separately using HCPCS codes and justify usage in the provider’s notes.
Challenge 5: Delayed AR and Cash Flow Gaps
Without proactive follow-up, unpaid claims can age beyond 90 days, causing serious cash flow problems.
Solution:
Adopt a dedicated AR team for wound care practices with automated workflows for reprocessing denials, sending appeals, and escalating payer issues. Metrics like Days in AR < 30 should be your benchmark.
Benefits of Outsourcing Wound Care Billing Services
Outsourcing to a professional wound care billing company is a strategic move that allows providers to focus on patient outcomes instead of administrative burdens. Here are the top reasons wound care centers outsource billing and coding:
1. Improved Accuracy and Compliance
Specialized billing partners have certified medical coders with expertise in outpatient wound care coding and Medicare wound care billing guidelines. This ensures:
- 98% First-Time Payment Resolution Rate (FTPR)
- Reduced risk of audit penalties
- Complete compliance with CMS and HIPAA regulations
2. Increased Revenue & Faster Collections
With proper denial management, payer communication, and real-time analytics, outsourcing can improve collection rates by 20–30%.
Your billing partner ensures:
- Daily claim submission
- AR follow-up within 24 hours
- Accurate posting and reconciliation
3. Access to Advanced RCM Technology
Outsourced RCM teams leverage AI-driven billing platforms, clearinghouse integrations, and real-time dashboards to optimize financial performance. These tools flag missing documentation, automate coding checks, and monitor KPIs like denial rate and average reimbursement per claim.
4. Cost Efficiency
Hiring and training in-house billers is expensive. Outsourcing eliminates overhead costs, software subscriptions, and compliance training expenses.
You only pay for collections-based pricing, making it a scalable solution for both small wound care clinics and multi-location centers.
5. Focus on Patient Care
When billing complexities are off your plate, your clinicians can focus entirely on healing patients, not chasing payments. This not only boosts productivity but also enhances patient satisfaction and practice reputation.
Key Features of a Reliable Wound Care Billing Company
Choosing the right wound care billing company can make or break the financial health of your practice. The best billing partner should not only ensure error-free claims but also align their RCM strategy with your clinical workflow, compliance requirements, and revenue goals. Here are the most essential features you should look for:
1. Certified and Experienced Billing Specialists
A reliable billing company employs certified coders (CPCs) and RCM experts with in-depth knowledge of wound care billing codes, CPT/ICD-10 updates, and Medicare wound care billing guidelines.
They understand complex coding scenarios such as:
- Multiple wound debridement codes per visit
- Proper use of modifiers (-59, -25, -RT/LT)
- Bundled services and global periods
This expertise ensures every claim is fully optimized for maximum reimbursement.
2. Comprehensive End-to-End RCM Solutions
Instead of focusing only on claim submission, a professional wound care billing service manages the entire revenue cycle, including:
- Patient eligibility verification
- Charge capture and coding
- Claim submission and denial management
- Payment posting and financial reporting
This integrated approach minimizes errors at each stage and maintains a steady cash flow for your wound care clinic.
3. Specialty-Specific Knowledge
Wound care billing requires a specialized understanding of:
- Outpatient wound care coding and documentation
- Healogics’ specialty physicians’ billing protocols
- Billing for wound care supplies (HCPCS Level II codes)
- Frequency limitations for Medicare wound care billing
Billing companies familiar with these nuances can prevent denials caused by misinterpreted payer rules or medical necessity criteria.
4. Transparent Reporting and Real-Time Analytics
Financial transparency is crucial. A dependable billing partner provides:
- Monthly RCM performance reports
- Claim-level analytics
- Aging AR summaries
- Denial trends and payer comparison charts
These insights help your administrative team make informed decisions and identify areas for improvement.
5. Strong Compliance and Security Standards
Your wound care billing partner must follow HIPAA-compliant data handling practices and maintain up-to-date CMS compliance. Regular internal audits, staff training, and secure data transfer protocols ensure full protection of patient and financial data.
Technology & Automation in Wound Care Billing
Modern RCM technology is revolutionizing wound care billing. Automation and analytics now replace manual tasks, reducing human error and improving turnaround times. Here’s how technology enhances efficiency and profitability in wound care practices:
1. AI-Powered Coding and Claim Scrubbing
Advanced billing platforms use AI and machine learning to analyze clinical notes and automatically assign appropriate ICD-10 and CPT codes.
This reduces coding errors and ensures claims are scrubbed for payer-specific rules before submission—boosting First-Time Payment Resolution Rates (FTPR) up to 98%.
2. Intelligent Eligibility Verification Systems
Automated eligibility tools instantly verify patient insurance coverage and wound care benefits in real time.
They check Medicare wound care coverage limits, detect inactive plans, and confirm authorizations—reducing claim rejections due to eligibility issues by up to 30%.
3. Real-Time Analytics Dashboards
Modern billing software provides interactive dashboards that show live KPIs, including:
- Claim status tracking
- Denial rate trends
- Days in AR metrics
- Top reimbursing CPT codes
These insights empower providers to make data-driven decisions and maintain a consistent revenue growth trajectory.
4. EHR/EMR Integration
Integration between your Electronic Health Record (EHR) and billing system ensures seamless data flow.
This eliminates double entry, automates documentation imports, and prevents claim errors linked to mismatched clinical details. Many wound care billing companies integrate with systems like Epic, Cerner, Athenahealth, and Healogics platforms for accuracy and compliance.
5. Robotic Process Automation (RPA) for AR Management
RPA bots automate repetitive AR follow-up tasks—tracking unpaid claims, sending payer reminders, and initiating appeals.
This drastically reduces aging AR days and improves collection rates, allowing your staff to focus on patient engagement instead of paperwork.
6. Compliance Automation
Automation also assists in Medicare wound care billing compliance by automatically cross-checking documentation against LCD (Local Coverage Determinations) and NCD (National Coverage Determinations) before claim submission.
Case Studies: Proven Success in Wound Care Billing Optimization
Case Study 1: Increasing Revenue for a Hospital-Based Wound Care Center
A multi-provider wound care center in Florida faced frequent denials due to improper modifier use and supply billing errors.
After outsourcing their billing to a specialized wound care billing company, the results were transformative:
- Denial rate reduced by 45% within 90 days
- Collection rate improved from 80% to 96%
- Monthly cash flow increased by 27%
By aligning clinical documentation with Medicare wound care billing guidelines, every claim was backed by strong medical necessity evidence.
Case Study 2: Streamlining Outpatient Wound Care Billing for a Private Practice
A solo wound care practitioner in Texas struggled with delayed payments and inconsistent billing for biologic grafts and debridement codes.
The outsourcing partner implemented AI-driven coding verification and real-time RCM reporting tools, achieving:
- 98% FTPR (First-Time Payment Resolution Rate)
- Reduction in AR days from 65 to 28
- Increased average reimbursement per patient by 18%
This case highlights how specialized wound care billing and coding services eliminate guesswork, maximize reimbursement, and maintain compliance.
Case Study 3: Medicare Compliance Improvement for a Multi-Clinic Network
A large outpatient network faced audit risks due to inconsistent documentation practices. With expert coding audits, EHR integration, and staff education, compliance scores improved by 35%, and audit exposure dropped to near zero.
How to Choose the Right Wound Care Billing Partner
Selecting the ideal wound care billing and coding partner can transform your revenue operations. Here’s a practical checklist to help you make the right decision:
1. Verify Their Wound Care Expertise
Ask whether the billing company specializes in wound care, Healogics billing, or outpatient wound care coding.
Request references or case studies that demonstrate success in managing wound care claims and navigating Medicare guidelines.
2. Evaluate Their Compliance Track Record
Ensure the company follows:
- HIPAA data security protocols
- CMS wound care billing guidelines
- Periodic internal and external audits
Compliance protects your practice from penalties and recoupments.
3. Review Their Technology Stack
Choose a partner that uses advanced RCM platforms, AI-powered claim scrubbing, and automated AR workflows.
Ask for live dashboard access to monitor KPIs like:
- Denial percentage
- Days in AR
- Collection ratio
- Average reimbursement per claim
Transparency builds trust.
4. Assess Their Reporting & Communication
The best billing companies maintain clear, frequent communication. They provide weekly or monthly reports, respond promptly to queries, and offer actionable insights—not just raw data.
5. Understand Pricing Models
Avoid “one-size-fits-all” pricing. A reliable partner offers collections-based or hybrid pricing models, ensuring you pay only for results. This structure aligns their performance with your profitability goals.
6. Check for Scalability & Support
As your wound care business grows, your billing company should be able to scale with you—adding more providers, locations, and service lines without compromising efficiency.
Ask about their support hours, turnaround time for claims, and client retention rate.
Final Takeaway
In the ever-evolving world of wound care billing services, success depends on combining human expertise, automation, and strategic partnerships.
By aligning your clinic with a specialized billing company that understands Medicare wound care billing, leverages AI-powered RCM tools, and maintains compliance-first workflows, you can achieve:
- Faster reimbursements
- Reduced denials
- Enhanced patient satisfaction
- Sustainable revenue growth
Outsourcing your wound care billing and coding services isn’t just a cost-saving choice—it’s a growth strategy that positions your practice for long-term financial stability and operational excellence.
Latest Trends & Future of Wound Care Billing in 2025 and Beyond
The landscape of wound care billing services is evolving faster than ever, driven by advances in automation, data analytics, and evolving Medicare billing guidelines. To stay financially strong, wound care providers must adapt to these technological and regulatory shifts. Let’s explore the latest trends shaping the future of wound care billing and reimbursement.
1. Artificial Intelligence and Predictive Analytics
AI is no longer a futuristic concept—it’s transforming how wound care billing operates today.
Modern medical billing solutions powered by machine learning analyze historical claims data, predict denial patterns, and suggest the most compliant coding combinations.
Predictive analytics helps billing teams:
- Detect underpayments and lost revenue opportunities
- Identify the most profitable CPT and HCPCS codes
- Automatically flag compliance risks before claim submission
AI-driven claim scrubbing now improves first-pass acceptance rates by up to 99%, reducing manual rework and accelerating reimbursements.
2. Integration of Telehealth and Remote Wound Monitoring
With the rise of telemedicine, more wound care providers are conducting virtual follow-ups for post-surgical wounds and chronic ulcer management.
Telehealth wound care billing introduces unique coding rules, including place of service modifiers and telehealth-specific CPT codes (e.g., 99441–99443).
Medicare and commercial insurers are expanding reimbursement eligibility for remote wound monitoring and store-and-forward documentation, giving practices new revenue opportunities while improving patient outcomes.
3. Data-Driven Denial Management
In 2025, proactive denial management is essential. Billing companies now use big data analytics to identify the most common causes of claim denials—like insufficient documentation or mismatched wound size descriptions—and implement targeted fixes.
This shift from reactive to predictive denial prevention has led to up to 40% faster payment cycles across outpatient wound care clinics.
4. Value-Based Reimbursement Models
The traditional fee-for-service model is transitioning toward value-based care. Payers are now rewarding providers who demonstrate measurable improvements in wound healing outcomes.
This means accurate, outcomes-based documentation and coding are more critical than ever.
Wound care billing companies are incorporating clinical outcome reporting into the billing workflow, aligning revenue cycle management (RCM) with patient care quality.
5. Automation of Compliance Checks
Constant changes in Medicare wound care billing guidelines can overwhelm providers.
Automation tools now cross-check every claim against Local Coverage Determinations (LCDs) and National Coverage Determinations (NCDs) to ensure documentation supports medical necessity.
This not only prevents audit risks but also ensures compliance with CMS and payer policies—critical for practices in states like California, Virginia, and North Carolina, where audits are frequent.
6. Enhanced Patient Billing Experience
Patients today expect transparency in their medical costs.
RCM platforms are integrating patient payment portals that provide real-time cost estimates, easy online payments, and digital receipts.
Improving patient billing communication strengthens trust and boosts collection rates while reducing administrative calls and disputes.
7. Cloud-Based and Interoperable Systems
The future of wound care billing lies in interoperability—systems that can communicate seamlessly between EHR, clearinghouses, and payer portals.
Cloud-based billing systems ensure scalability, secure remote access, and disaster recovery. For multi-location wound care networks, this offers unified billing management across all facilities.
Frequently Asked Questions (FAQs) about Wound Care Billing Services
1. What are wound care billing services?
Wound care billing services involve managing the end-to-end billing and coding process for wound treatment procedures—such as debridement, grafts, and dressings—to ensure accurate reimbursement and compliance with payer policies.
2. How does Medicare handle wound care billing?
Medicare wound care billing follows strict LCD and NCD coverage policies. Claims must include accurate ICD-10 codes for wound type, location, and severity, along with CPT codes for procedures performed (e.g., 97597–97598 for debridement).
3. What makes wound care billing complex?
Wound care involves multiple visits, overlapping procedures, and extensive documentation. Accurate modifier use, medical necessity proof, and payer-specific rules make it more complex than standard medical billing.
4. Why should I outsource wound care billing?
Outsourcing to expert wound care billing companies minimizes claim denials, improves cash flow, and ensures compliance with HIPAA and Medicare standards. It also frees your in-house team to focus on patient care.
5. How do wound care billing companies reduce denials?
Professional billing firms use AI-powered claim scrubbing, real-time eligibility verification, and denial tracking systems to detect and fix errors before claim submission—significantly improving first-pass claim approval rates.
6. What documentation is required for wound care billing?
Providers must record wound size, depth, type, debridement level, and healing progress in each visit note. This documentation justifies medical necessity and ensures correct coding for reimbursement.
7. How often should wound care be done and billed?
Billing frequency depends on wound type and treatment plan. Chronic wounds may require weekly debridement sessions, while acute wounds might only need one or two follow-ups. Always check payer-specific limits.
8. What are the latest wound care billing guidelines for 2025?
The 2025 updates emphasize electronic claim submission, AI-driven compliance, and remote wound monitoring billing. CMS has also expanded telehealth coverage and automated prior authorization tools.
9. Are wound care billing services HIPAA compliant?
Yes, reputable wound care billing companies follow HIPAA and CMS data protection standards, ensuring confidentiality, secure data transmission, and privacy across all digital workflows.
10. How long does it take to see results after outsourcing wound care billing?
Most providers see measurable improvement in revenue within 60–90 days, including higher reimbursement rates, fewer denials, and faster claim turnaround times.
Conclusion: Transform Your Practice with Expert Wound Care Billing Services
In the ever-changing healthcare landscape, wound care billing services are no longer just about claim submission—they are about driving financial efficiency, regulatory compliance, and patient satisfaction.
Partnering with an experienced billing company ensures:
- Accurate coding and timely reimbursements
- Full compliance with Medicare and payer guidelines
- Reduced denials and improved cash flow
- Optimized revenue cycle management through AI and automation
Whether you manage a wound care center, outpatient facility, or home health agency, outsourcing your billing to specialists with deep expertise in wound care documentation, coding, and payer rules guarantees sustainable growth and peace of mind.
At Elitemed Financials, our certified RCM professionals, coders, and analysts work exclusively with wound care providers across the United States—including California, Virginia, and North Carolina—to simplify complex billing challenges and maximize reimbursements.
We use AI-driven billing automation, HIPAA-compliant systems, and customized reporting dashboards to deliver transparent, error-free results every time.
 Ready to Optimize Your Wound Care Billing?
Ready to Optimize Your Wound Care Billing?
Schedule a Free Consultation with Elitemed Financials Today.
Let our team help you eliminate denials, increase reimbursements, and achieve a more predictable revenue cycle.



For further details and regulatory insights, professionals can always refer to official CMS guidelines on Medicare wound care billing, review the CPT code references provided by the American Medical Association, or explore the latest research and standards shared by the American College of Wound Healing and Tissue Repair. These trusted sources ensure your wound care billing practices stay compliant, accurate, and aligned with national standards.
 Ready to Optimize Your Wound Care Billing?
Ready to Optimize Your Wound Care Billing?