Is Non-Emergency Transportation a Good Business? [2026 Profit Analysis]
Table of Contents
Introduction
If you’re considering entering the non-emergency medical transportation (NEMT) industry in 2026, you’re asking the right question at precisely the right time. The short answer is yes—NEMT can be a profitable business—but success depends heavily on your location, operational efficiency, and understanding of the industry’s unique challenges and opportunities.
The NEMT industry sits at the intersection of two powerful forces: explosive demographic growth and critical healthcare access needs. The market is currently valued between $9.8 billion and $11.8 billion and is projected to reach $15 billion to $19.9 billion by 2030, representing a robust compound annual growth rate of 7% to 9.7%. According to the Centers for Medicare & Medicaid Services (CMS), NEMT is a federally mandated benefit under the Medicaid program, ensuring that eligible beneficiaries have reliable transportation to medical appointments. With approximately 11,400 Baby Boomers turning 65 every single day in 2026, demand for medical transportation services isn’t just growing—it’s accelerating.
Yet these impressive numbers tell only half the story. The reality is that roughly 4 million Americans miss or delay critical medical appointments annually due to transportation barriers, revealing both the scale of unmet need and the business opportunity for providers who can deliver reliable service. In this comprehensive guide, we’ll cut through the industry hype to deliver real profitability data—including actual monthly income calculations from single-van and fleet operations—detailed startup cost breakdowns, state-by-state rate variations, and the honest operational challenges that cause 70% of new NEMT providers to fail within their first few years. Whether you’re planning to start with a single vehicle or build a regional fleet, you’ll get the evidence-based analysis you need to make an informed decision about entering this essential, growing industry.
The Short Answer: Is NEMT a Good Business?
Yes, the non-emergency medical transportation business can be profitable, but it’s far from a passive income opportunity. NEMT business owners operating a single vehicle typically earn between $40,000 and $60,000 annually, while fleet operators managing 5-10 vehicles can generate $72,000 to $120,000 or more per year. However, these earnings require active daily management and strategic positioning.
The profitability of your medical transportation company hinges on five critical factors:
Location and state reimbursement rates create your financial ceiling. Medicaid rates vary dramatically—New York providers earn $45 to $120 per wheelchair trip, while Tennessee operators receive just $18 to $45 for identical services. This rate differential fundamentally determines your revenue potential.
Business model and payer mix directly impact profit margins. Healthcare transport services focused exclusively on Medicaid typically achieve 10-15% net margins. Operators who build a diversified payer mix—combining Medicaid with private-pay clients and facility contracts—can achieve 20-30% margins. Private dialysis transportation costs $75 to $150 per trip compared to Medicaid’s $40 to $60.
Operational efficiency separates profitable operators from those barely breaking even. The average NEMT vehicle operates at just 35% utilization, meaning drivers generate revenue only one-third of their shift. Operators implementing AI-powered dispatch software boost utilization to 60-80%, adding $5,000 to $10,000 annually per vehicle.
NEMT businesses generate revenue by providing transportation services to patients, but the real profit depends on mastering the billing process and for that prior authorization is the think provider should keep in mind always. Understanding how NEMT billing works is essential before starting your business—providers who achieve 95%+ clean claim rates earn significantly more than those struggling with denials.
✅ Best For:
- Small business owners with operations or logistics experience
- Entrepreneurs with strong customer service skills
- Areas with dense senior populations (15%+ aged 65+)
- Those comfortable navigating healthcare regulations
❌ Not Ideal For:
- Anyone seeking passive income (except 40-60 hour weeks)
- Oversaturated markets with broker dominance (70%+ control)
- Those expecting six-figure profits from one vehicle in year one
- Insufficient startup capital (need $30K-$50K minimum plus reserves)
The non-emergency transport industry offers a genuine opportunity backed by demographic trends—it’s growing, essential, and recession-proof. However, the 20-30% profit margins are earned through operational excellence. Thin margins mean efficiency isn’t optional—it’s the difference between sustainability and joining the 70% who fail within three years.
Understanding the NEMT Business Model
Non-emergency medical transportation provides scheduled rides to medical appointments for patients who don’t require emergency care but need assistance getting to healthcare facilities. Unlike ambulance services that respond to 911 calls with trained EMTs, NEMT focuses on planned transportation for routine appointments, dialysis treatments, physical therapy, mental health visits, and similar non-urgent medical needs.
Service Types You Can Offer
Wheelchair-Accessible Van Services represent the most common NEMT category. These trips use specially modified vans with ramps or lifts to transport wheelchair users. Medicaid reimbursement ranges from $45 to $150 per trip, depending on your state, with premium weekend rates reaching $75 to $90. Higher rates reflect specialized equipment costs ($3,600 to $15,900 for lifts) and longer loading times.
Ambulatory Transportation serves the largest patient volume using standard minivans or sedans for patients who can walk independently. Rates are lower—typically $25 to $60 per trip—but faster turnaround allows 6-10 trips daily compared to 3-5 wheelchair transports.
Stretcher Van Services occupy the highest-paying niche at $100 to $400+ per trip, transporting bedridden patients on gurneys. However, these require two-person crews and insurance costs often 2-3x standard premiums, limiting this service to established operators.
Key Distinction: NEMT vehicles are not ambulances. You won’t provide medical care, respond to emergencies, or need EMT certification. However, drivers must complete training in wheelchair securement, CPR/First Aid, HIPAA compliance, and patient interaction protocols.
Where Revenue Comes From
Medicaid Contracts (60-70%) serve as the financial backbone. State Medicaid programs are federally mandated to provide transportation benefits, creating stable demand. According to CMS data, 3-4 million Medicaid beneficiaries use NEMT annually. Trade-offs include 30-90 day payment delays and 10-20% claim denial rates.
According to the Centers for Medicare & Medicaid Services (CMS), approximately 3-4 million Medicaid beneficiaries utilize NEMT services annually, making it a federally-mandated benefit that ensures consistent demand for qualified transportation providers.
Private Pay Clients (15-25%) represent your most profitable stream. Direct payment eliminates broker fees and accelerates payment to same-day or within 7 days. Rates range from $50 to $250 per trip for specialized services like dialysis transportation.
Medicare Reimbursements (5-10%) play a limited role. Traditional Medicare doesn’t cover routine transport, but Medicare Advantage plans increasingly include NEMT benefits.
Healthcare Facility Contracts (5-15%) provide stable revenue through direct agreements with hospitals, dialysis centers, or senior living communities, paying $60 to $100+ per trip for guaranteed availability.
Market selection dramatically impacts revenue potential since Medicaid reimbursement varies by over 300% between states. Before expanding, review current rates in our state-by-state Medicaid NEMT reimbursement guide.
Understanding the NEMT Broker System
Most operators work through transportation brokers—intermediaries between state Medicaid agencies and providers. ModivCare leads with 25-35% market share, managing 5,000+ providers nationwide, while MTM/Logisticare operates in 33 states with a 15-25% share.
How It Works: State agencies award contracts to brokers who manage the entire NEMT benefit—eligibility, scheduling, provider networks, and payment. You contract with brokers (not states directly) and receive trip assignments via their platforms. After completing trips and submitting documentation, brokers process claims and issue payment within 30-90 days.
The Economics: Brokers don’t directly deduct fees. Instead, they set provider rates within state-approved ranges, embedding their 10-30% management fee into the rate structure. The $40 to $60 you receive for wheelchair transport already reflects the broker’s margin.
Successful operators view brokers as distribution channels providing volume while simultaneously building direct facility contracts and private-pay clients to diversify beyond broker dependence.
The Economics: How Much Do NEMT Companies Make?
Understanding the real income potential of a medical transportation business requires breaking down revenue per trip, realistic trip volumes, operating expenses, and how these numbers scale from single-vehicle operations to fleet management. The profitability equation varies dramatically based on your state’s reimbursement rates, service specialization, and operational efficiency.
Revenue Potential by Service Type and Location
Average Revenue Per Trip varies significantly by service category and geography. Ambulatory transportation—the most basic service level—generates $25 to $60 per trip in most markets, with lower rates in Southern states ($18 to $35) and premium rates in high-cost Northeastern and West Coast markets ($35 to $60). Wheelchair-accessible van transport commands substantially higher reimbursement at $45 to $150 per trip, reflecting the specialized equipment and training requirements. Weekend and off-hours wheelchair trips can reach $75 to $90, even in moderate-rate states. Stretcher transport sits at the top of the rate structure at $100 to $400+ per trip, though operational complexity limits this segment to established operators.
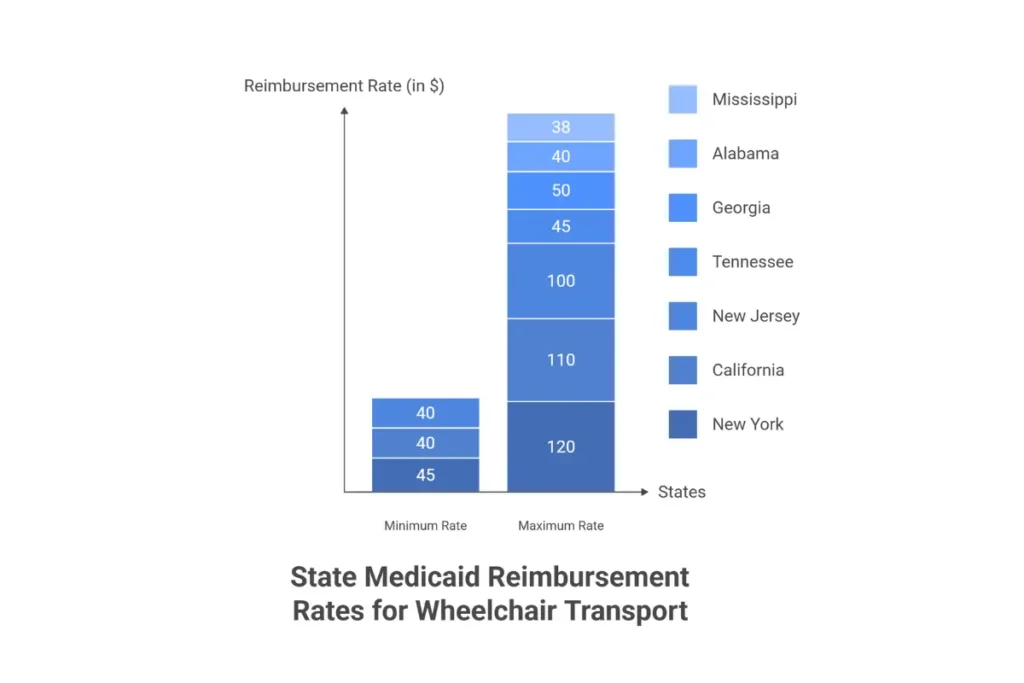
State-by-State Rate Analysis reveals stark disparities that fundamentally impact business viability. According to industry data, state Medicaid reimbursement rates range from 55% to 265% of the standard Medicare rate, with the highest-paying state offering rates 454% higher than the lowest. This translates to real-world differences: New York wheelchair transport pays $45 to $120 per trip, California ranges from $40 to $110, and New Jersey offers $40 to $100. Meanwhile, Tennessee operators receive just $18 to $45, Georgia pays $20 to $50, Alabama offers $18 to $40, and Mississippi bottoms out at $16 to $38 per trip for identical services.
Real Income Calculations: From Single Van to Fleet
Single Van – Ambulatory Focus: A well-optimized vehicle completing 10 ambulatory trips daily at an average rate of $35 generates $350 per day. Operating 22 working days monthly yields $7,700 in gross revenue. After deducting driver wages ($2,000 to $2,500), fuel costs ($400 to $600), insurance ($833 to $1,250 monthly), vehicle maintenance ($200 to $400), and administrative overhead ($150 to $300), net monthly profit ranges from $3,500 to $4,500. This translates to $42,000 to $54,000 in annual owner income for an owner-operator model where the owner serves as the primary driver.
Single Van – Wheelchair Service: A wheelchair-accessible van completing 3 high-value trips daily at $85 each generates $255 per day, or $5,610 monthly across 22 working days. The higher per-trip revenue partially offsets lower trip volume. After similar expense deductions—though insurance typically runs 15-20% higher for wheelchair vehicles—net monthly profit reaches $2,800 to $3,500, yielding $33,600 to $42,000 annually. The lower absolute income compared to high-volume ambulatory service is offset by reduced driver stress and wear on the vehicle.
5-Van Fleet Operation: A well-managed fleet with three ambulatory vans and two wheelchair vans generates a combined gross revenue of $30,000 to $40,000 monthly. However, fleet economics differ substantially from owner-operator models. Driver wages now represent 40-45% of revenue ($12,000 to $18,000 monthly for five drivers). Adding fleet insurance ($4,000 to $6,000), fuel ($2,000 to $3,000), maintenance ($1,000 to $2,000), dispatch software ($250 to $500), and administrative salaries ($3,000 to $5,000), total monthly expenses reach $22,000 to $34,000. This leaves owner’s net profit of $6,000 to $10,000 monthly, or $72,000 to $120,000 annually—but only with rigorous cost control and 70%+ vehicle utilization rates.
Profit Margins and the Efficiency Factor
Industry Benchmarks place sustainable NEMT profit margins at 20-30% for well-run operations using technology and efficient routing. Single vehicle owner-operators can achieve 50-70% margins by internalizing driver labor costs—essentially paying themselves the driver wage plus profit. However, this model caps total earnings due to limited trip capacity. Fleet operations see structurally lower percentage margins (15-25%) due to externalized labor and overhead, but higher absolute dollar profits through volume leverage.
The Technology Advantage dramatically impacts these numbers. Operators using dedicated NEMT dispatch and routing software increase monthly revenue per vehicle by 26% to 51% compared to manual scheduling, from approximately $3,300 monthly to $4,160 to $5,000. This $860 to $1,700 monthly improvement per vehicle stems from optimized routing that cuts travel time by 15-20%, increased utilization that boosts productive hours by 25%, and reduced no-shows through automated patient reminders.
State Reimbursement as the Financial Ceiling: Your profit potential is ultimately constrained by state Medicaid policy. The research data shows that 21 states increased NEMT rates in 2024, with 15 more planning increases in 2026. States classifying NEMT as a medical service (rather than an administrative cost) receive higher federal matching funds and tend to offer better reimbursement rates. Operators in high-rate states can achieve target profit margins with 5-6 trips daily, while low-rate state operators need 8-10 trips just to reach breakeven—a fundamental competitive disadvantage.
Understanding Your Expense Structure
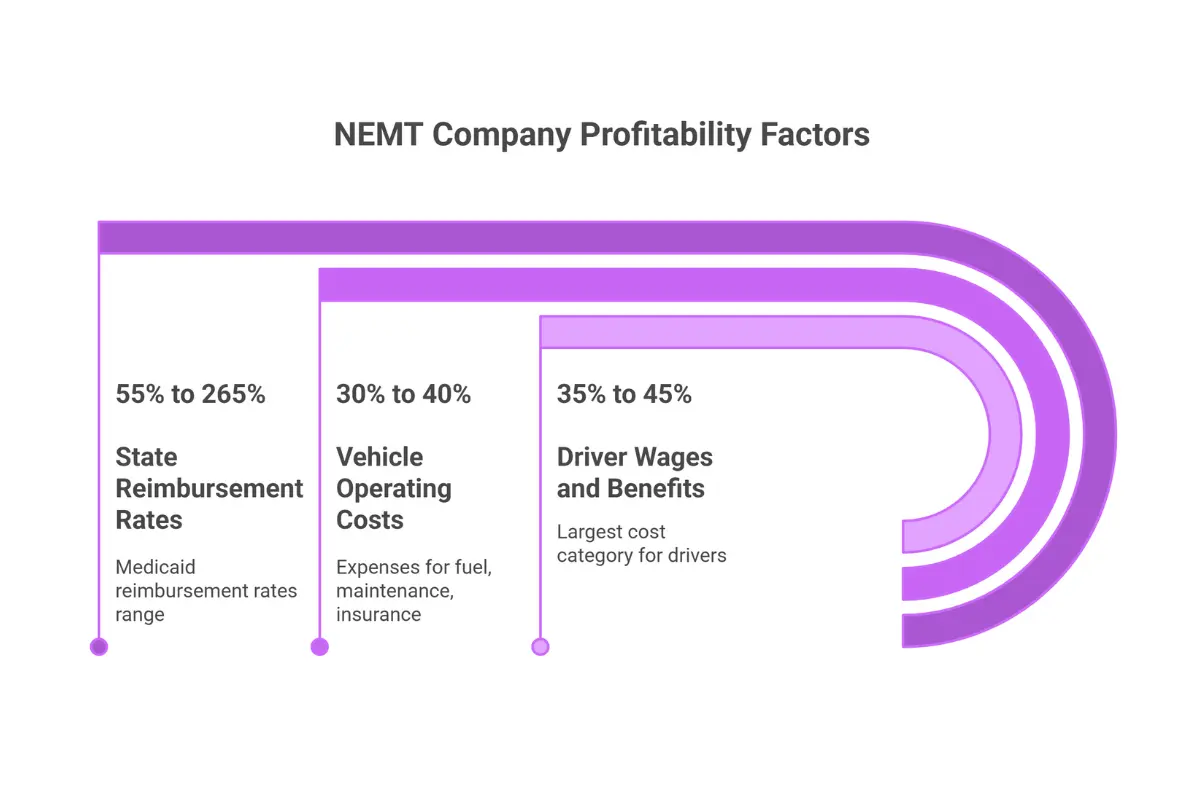
Driver Wages and Benefits consume 35-45% of operational expenses, making this your largest cost category. Competitive wages of $18 to $25 per hour are necessary to reduce the industry’s chronic 50-100% annual turnover rate. For a full-time driver working 160 hours monthly, this translates to $2,880 to $4,000 in base wages before payroll taxes and any benefits.
Vehicle Operating Costs (fuel, maintenance, insurance) represent 30-40% of expenses. Commercial auto insurance is particularly volatile, ranging from $4,200 to $18,000 annually per vehicle, depending on location—rural areas average $3,500, suburban markets $4,500, urban centers $5,500, and major cities like New York or Los Angeles can exceed $7,500 annually. Insurance costs can spike 30-50% at renewal following any claims, making this the most unpredictable fixed expense.
The Deadhead Mile Problem silently erodes 20-30% of potential profits. These unpaid miles—driving empty to the next pickup or returning to base—consume fuel and driver time without generating revenue. Operators achieving 80% vehicle utilization through AI routing effectively reclaim $5,000+ annually per vehicle compared to the industry average 35% utilization rate. This efficiency gap often determines whether operators achieve 25% margins or struggle at 10%.
How Much Does It Cost to Start an NEMT Business?
Starting a non-emergency medical transportation company requires substantial upfront capital and careful financial planning to survive the initial months before consistent revenue arrives. Understanding both one-time startup investments and ongoing monthly expenses is critical for adequate capitalization.
Vehicle Investment: Your Largest Capital Requirement
New Wheelchair-Accessible Vans represent the gold standard for reliability but command premium prices. A new Ford Transit or RAM ProMaster chassis costs $45,000 to $65,000, with wheelchair conversion adding another $20,000 to $50,000 for ramp or lift installation, securement systems, and ADA compliance modifications. Total investment for a new, fully converted wheelchair van ranges from $65,000 to $98,000. Mercedes-Benz Sprinter conversions can exceed $110,000 for premium operations targeting high-end private-pay markets.
Pre-Owned Options dramatically reduce upfront costs but introduce reliability risks. Used wheelchair-accessible vans range from $18,000 to $75,000, depending on age, mileage, and conversion quality. A strategic middle ground involves purchasing a used chassis ($30,000 to $50,000) and installing a new, warrantied conversion ($20,000 to $40,000), securing reliability on the high-liability mobility components while reducing total investment to $50,000 to $83,000.
Ambulatory-Only Startups can launch with standard minivans, dramatically lowering barriers. A used Dodge Grand Caravan or Chrysler Pacifica with minimal modifications costs $20,000 to $35,000 fully equipped. This lean approach allows bootstrap startups to prove the business model and generate revenue before investing in specialized wheelchair equipment.
Insurance: “The Most Painful Part”
Commercial auto insurance consistently ranks as operators’ biggest financial shock and most volatile fixed cost. Annual premiums range from $8,000 to $15,000 per vehicle for the required $1 million liability coverage, with significant geographic variation. Rural operators pay approximately $3,680 annually, suburban markets average $4,500, urban areas reach $5,500, and major metropolitan markets like New York City or Los Angeles can exceed $18,000 per vehicle annually.
The true pain comes at renewal. Industry data shows premiums can spike 30-50% following any claims, even minor ones, and insurers frequently impose surprise audit-based increases when your risk profile changes—adding vehicles, expanding service areas, or hiring additional drivers all trigger reassessments. Operators should budget for premium increases and maintain a cash reserve specifically for insurance cost escalation, as this single expense can swing from $833 monthly to $1,500+ overnight, instantly eroding months of profit.
Hidden Costs and Regulatory Requirements
DOT Compliance and Licensing adds $1,000 to $3,000 in initial setup costs. This includes business entity formation ($500 to $1,000), state-specific NEMT operating permits ($500 to $2,000 depending on jurisdiction), DOT physical exams ($85 to $225 per driver), and mandatory pre-employment drug screening ($30 to $80 per driver). Annual renewal fees of $300 to $800 create ongoing regulatory overhead.
ADA Compliance extends beyond one-time vehicle conversion. Federal law mandates “prompt” repair of wheelchair lifts and ramps, requiring backup vehicles or premium service contracts ($2,000 to $4,000 annually) to avoid service interruptions. Operators must also maintain certified personnel training on proper securement techniques, with recurring certification costs of $200 to $500 per driver annually.
Technology Infrastructure is mandatory for competitive operations. NEMT-specific dispatch and routing software costs $50 to $200 per vehicle monthly ($600 to $2,400 annually). GPS tracking and dashcam systems—often required by insurers and Medicaid contracts—add $300 to $800 in upfront equipment costs per vehicle. HIPAA-compliant billing systems, secure communication platforms, and electronic health record integration can add another $1,500 to $3,000 in first-year setup costs.
Many NEMT startups partner with healthcare IT service providers for initial system setup, network security, HIPAA-compliant data storage, and ongoing technical support—ensuring compliance from day one while avoiding costly setup mistakes.
Vehicle Branding and Marketing creates essential credibility. Professional vehicle wraps cost $2,500 to $4,000 per van but significantly impact customer perception and facility trust. Initial digital marketing setup—professional website, Google Business Profile optimization, and facility outreach materials—requires $2,000 to $5,000 for operators serious about private-pay client acquisition.
Total Investment Requirements
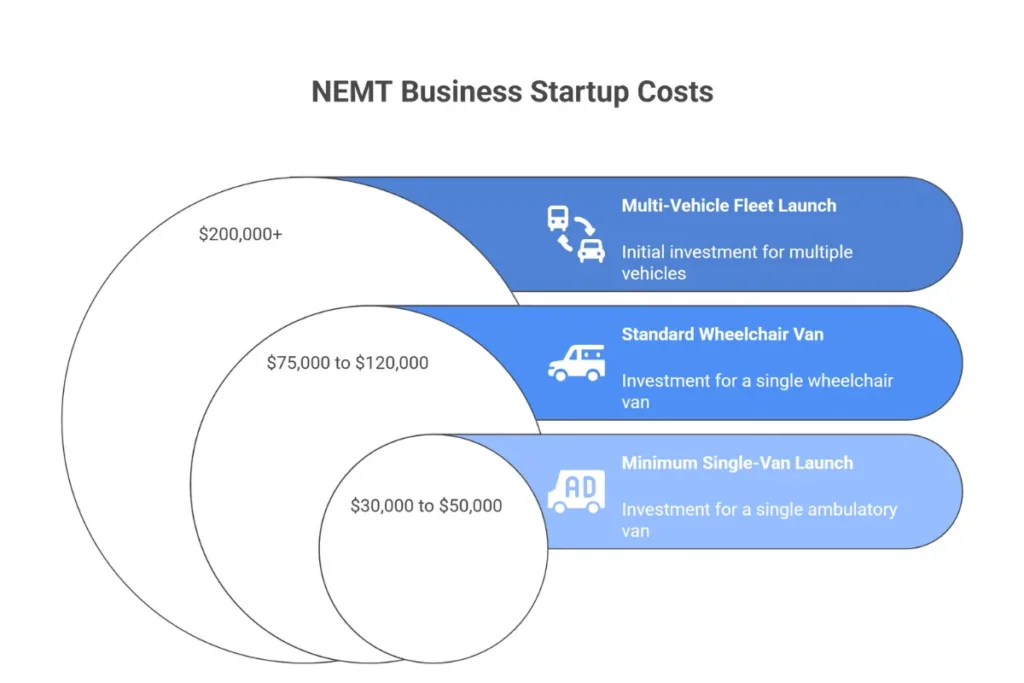
Minimum Single-Van Launch ($30,000 to $50,000): Used ambulatory vehicle ($20K to $35K) + insurance deposit ($1,500 to $2,500) + licensing ($1,000 to $2,000) + technology ($1,000 to $2,000) + initial marketing ($1,000 to $2,000) + 3-month operating reserve ($5,000 to $7,500). This lean approach targets private-pay and facility contracts while the Medicaid application process.
Standard Single Wheelchair Van ($75,000 to $120,000): New or quality used wheelchair van ($60K to $90K) + insurance ($2,500 to $4,000 deposit) + licensing and compliance ($2,000 to $3,000) + technology ($2,000 to $3,000) + marketing ($3,000 to $5,000) + 6-month operating reserve ($10,000 to $15,000). This model targets full-service Medicaid contracts with immediate operational capability.
Multi-Vehicle Fleet Launch ($200,000+): Three vehicles ($150K to $250K) + fleet insurance deposits ($7,500 to $12,000) + comprehensive licensing ($5,000 to $8,000) + enterprise software ($5,000 to $10,000) + facility-focused marketing ($5,000 to $10,000) + 6-month working capital reserve ($30,000 to $50,000). This approach targets immediate market presence and facility contract competitiveness.
Monthly “Burn Rate” and Cash Flow Reality
Every NEMT vehicle carries fixed monthly costs before completing a single trip. For a single van operation, expect a minimum monthly overhead of $2,000 to $3,500: commercial insurance ($833 to $1,250 monthly), technology subscriptions ($100 to $250), regulatory renewals amortized ($50 to $150), and vehicle financing ($800 to $1,500 if financed). This doesn’t include fuel, driver wages, or maintenance—these are your fixed survival costs.
The critical cash flow challenge is Medicaid’s 30-90 day payment cycle. You’ll complete trips in January, submit claims by mid-February, and receive payment in March or April. This creates a 60-90 day gap where you’re funding operations—driver payroll, fuel, insurance—without incoming revenue. Operators without adequate working capital reserves fail during this window, unable to sustain operations while awaiting their first Medicaid checks. This is why the 6-month operating reserve isn’t optional for Medicaid-focused businesses—it’s survival capital that bridges the gap between service delivery and payment receipt.
Working with experienced accounting professionals who understand healthcare businesses ensures proper financial structure, accurate cost tracking, tax-advantaged entity formation (S-corp vs LLC), and strategic financial planning that helps you survive and thrive through the startup phase.
NEMT Licensing Requirements by State
Regulatory complexity varies dramatically across states, creating significantly different barriers to market entry. Understanding your state’s classification system is essential for accurate startup planning and compliance budgeting.
Understanding State Regulatory Categories
Strict States (High Barrier to Entry) include New York, Virginia, California, New Jersey, and Florida. These jurisdictions often require Certificate of Need (CON) approvals—particularly for stretcher or gurney transport services—strict vehicle age limits (often 7-10 years maximum), extensive background checks including FBI fingerprinting, and centralized oversight by state health departments. New York, for example, mandates direct Department of Health provider certification with rigorous ongoing compliance audits. California requires CPUC (California Public Utilities Commission) permits with detailed operational plans. Startup timelines in these states extend 6-12 months from application to approval, and the CON process alone can cost $5,000 to $15,000 in legal and filing fees.
Moderate States (Standard Process) like Texas, Pennsylvania, Illinois, and Ohio offer clearer pathways without CON requirements for standard NEMT services. A single state agency—typically the Medicaid program or health department—administers standardized licensing with predictable requirements: business entity formation, proof of commercial insurance ($1M minimum), driver background checks, vehicle safety inspections, and Medicaid provider enrollment. Processing typically completes within 2-4 months. These states create scalable environments where operators who master the state-level blueprint can expand regionally without navigating dozens of local ordinances.
Easy Entry States (Local Control) such as Texas (paradoxically both moderate and fragmented), Florida, Arizona, Nevada, Indiana, and South Carolina delegate NEMT regulation to municipalities. This creates a patchwork where each city or county imposes separate taxi or livery commission requirements. While individual locality barriers are low—often just a local business license and vehicle inspection—statewide scaling requires managing potentially dozens of different compliance regimes. An operator serving the Dallas-Fort Worth metro area might need licenses from 15 separate municipalities, each with unique renewal dates and fee structures.
Key Federal and National Entities
US Department of Transportation (USDOT) regulations generally don’t apply to most NEMT operations. Federal Motor Carrier Safety Administration (FMCSA) requirements—DOT numbers, Hours of Service logs, interstate operating authority—only trigger for vehicles exceeding 10,001 pounds Gross Vehicle Weight Rating or crossing state lines for commercial purposes. Most wheelchair vans and ambulances fall below this threshold and operate intrastate, exempting them from federal DOT oversight. However, many states adopt FMCSA standards (like drug testing protocols) at the state level even when federal jurisdiction doesn’t apply.
The National Aging and Disability Transportation Center (NADTC) serves as the industry’s premier non-regulatory resource. This federally funded (FTA) technical assistance center provides state-specific compliance guides, training webinars on best practices, and comprehensive directories of state Medicaid NEMT requirements. While NADTC sets no legal requirements, its guidance materials influence state Medicaid agencies and Managed Care Organizations when developing quality standards and contract specifications.
State Medicaid Agencies and MCOs function as your primary functional regulators regardless of official licensing authority. These entities control reimbursement rates, establish service quality metrics, dictate specific driver training requirements (HIPAA, cultural competency, patient assistance), and conduct performance audits. Their contractual standards often exceed state transportation department minimums, making Medicaid compliance the true operational standard rather than basic licensing requirements.
Certificate of Need (CON) States
Certificate of Need requirements apply specifically to high-acuity stretcher and gurney transport in select states, most notably New York and Virginia. The CON process requires proving “public need” for your service, demonstrating financial viability, and often defending your application against existing providers who may protest additional competition. This regulatory barrier—costing $10,000 to $25,000+ in legal fees and taking 6-18 months—effectively restricts market entry for stretcher services.
Most operators in CON states strategically avoid offering stretcher transport, focusing exclusively on wheelchair and ambulatory services to bypass CON requirements entirely. This business decision sacrifices the highest per-trip revenue category ($100 to $400+) but enables market entry within 2-4 months rather than 12-18 months, preserving capital and generating revenue faster.
Universal Compliance Requirements
Regardless of state category, nearly all jurisdictions mandate:
Driver Screening and Credentialing: Comprehensive criminal background checks (state and often FBI fingerprinting in strict states), Motor Vehicle Record reviews showing clean driving history, mandatory drug and alcohol testing programs meeting FMCSA protocols even when federal jurisdiction doesn’t apply, and increasingly, sex offender registry clearances.
Driver Training and Certification: Standardized instruction in HIPAA privacy compliance, CPR and First Aid certification (renewed every 2 years), defensive driving coursework, and ADA-compliant passenger assistance techniques, including proper wheelchair securement, fall prevention, and patient dignity protocols. Total training costs $500 to $1,000 per driver initially, with $200 to $400 in recurring biennial recertification.
Vehicle Standards and Inspections: Annual or biannual safety inspections specifically examining wheelchair lift/ramp functionality, securement system integrity, fire extinguisher and first aid kit presence, and overall mechanical condition. Many states enforce maximum vehicle age limits (7-10 years) to ensure reliability and safety equipment compatibility.
Insurance Mandates: Commercial auto liability coverage with minimum limits typically set at $1 million Combined Single Limit, though some jurisdictions require $1.5M or $2M for larger vehicles. General liability insurance of $500,000 to $1 million protects against non-vehicle claims, and workers’ compensation is mandatory when employing drivers.
Where to Find State-Specific Information
The National Aging and Disability Transportation Center (NADTC) provides comprehensive state-by-state NEMT regulatory guides, compliance toolkits, training webinars, and direct contacts for state Medicaid transportation offices—making it the most valuable free resource for navigating the complex licensing landscape across different jurisdictions.
State Medicaid Agency Websites provide the most current provider enrollment requirements, reimbursement rate schedules, approved broker lists, and MCO contact information. Search “[Your State] Medicaid NEMT provider enrollment” to locate your state’s specific portal.
The National Aging and Disability Transportation Center (NADTC) offers comprehensive state-by-state resource guides on its website, including regulatory summaries, key contact information, and links to state-specific applications.
State Departments of Health or Transportation administer physical licensing requirements. In strict states, the Department of Health controls NEMT licensing. In moderate states, check both the Health and Transportation departments. In fragmented local-control states, contact your city or county clerk’s office for local ordinances.
For Certificate of Need states, search “[State] Certificate of Need NEMT” or “[State] CON program” to locate the specific application process and current CON holders in your market.
Choosing the Right Vehicle for Your NEMT Business
Vehicle selection fundamentally impacts your operating costs, service capabilities, and profit margins. The medical transportation industry has converged on several proven platforms, each offering distinct advantages for specific operational models.
Top Vehicle Options for 2026
Ford Transit leads the NEMT market with superior acceleration, optional all-wheel drive for adverse weather markets, and flexible configurations. The high-roof extended length model accommodates multiple wheelchair positions. Fuel economy averages 16-17 MPG, translating to approximately $6,200 to $6,600 annually in fuel costs at 30,000 miles per year. Base chassis costs $47,000, with wheelchair conversions adding $19,000 to $50,000 (total: $66,000 to $97,000). The Transit’s strong market presence ensures parts availability and widespread mechanic familiarity.
RAM ProMaster offers a lower floor height than competitors, simplifying wheelchair boarding and maximizing interior space through its boxy, front-wheel-drive design. This platform excels for urban operations where easy patient access and tight turning radius matter more than highway performance. Fuel economy of 15 MPG creates approximately $7,000 annual fuel costs. Base price of $44,000 plus $22,000 average conversion totals $66,000 to $94,000.
Mercedes-Benz Sprinter represents the premium choice for operators targeting high-end private-pay markets or emphasizing safety ratings and driver comfort. Superior build quality and comprehensive safety features justify the premium, while strong resale value (retaining 60% after 5 years) offsets higher acquisition costs. Fuel economy and maintenance costs mirror the Transit. Total investment exceeds $80,000 to $110,000+ fully converted.
Toyota Sienna Hybrid has emerged as the game-changing choice for ambulatory-focused and mixed-service operations. Delivering 36 MPG—more than double traditional vans—the Sienna cuts annual fuel costs to approximately $2,900 at 30,000 miles, saving $3,300 to $4,100 yearly compared to full-size vans. Available all-wheel drive and factory-quality hybrid reliability make this the financially optimal choice for routes handling 1-2 wheelchair passengers plus ambulatory clients. Fully converted units range from $40,000 to $60,000, offering lower acquisition costs and dramatically reduced operating expenses. The Sienna’s fuel efficiency alone can boost annual profit per vehicle by $3,000+, directly improving bottom-line margins.
Budget Entry Options using used Dodge Grand Caravan or Chrysler Pacifica models ($20,000 to $35,000 fully converted) serve bootstrap startups targeting ambulatory-only markets. However, both platforms were discontinued, creating parts scarcity concerns that may increase long-term maintenance costs and downtime.
Wheelchair Access: Ramp vs. Lift Decision
Wheelchair Ramps ($5,000 to $15,000 installed) have become the industry standard for high-volume operations. Ramps deploy faster than lifts (20-30 seconds vs. 60-90 seconds), require less maintenance due to fewer mechanical components, and prove more reliable with lower failure rates. The incline requires adequate interior space and proper deployment technique, but most operators report better long-term cost of ownership and faster boarding times that directly increase daily trip capacity.
Hydraulic Lifts ($10,000 to $25,000 installed) serve specific use cases: vehicles with insufficient interior length for ramp incline, operations with many perpendicular curb-parking scenarios where ramps can’t deploy properly, or markets with extreme weather where enclosed lift platforms protect patients better than exposed ramps. However, lifts’ higher mechanical complexity creates 2-3x the maintenance costs and more frequent out-of-service periods for repairs.
Key Decision Factors
For Ambulatory-Focused Operations: The Toyota Sienna Hybrid offers unmatched economics, cutting fuel costs by 50%+ while maintaining sufficient capacity for mixed wheelchair/ambulatory service. The $3,000+ annual fuel savings significantly impact single-van profitability.
For Wheelchair-Intensive Service: Ford Transit or RAM ProMaster provides the interior volume and durability for high-frequency wheelchair transport. Choose Transit for all-weather markets; ProMaster for dense urban environments, prioritizing maneuverability.
For Premium Private-Pay Markets: Mercedes-Benz Sprinter signals quality and professionalism to high-end clientele while offering superior driver comfort for long-distance facility contracts.
For Bootstrap Startups: Used wheelchair-accessible minivans ($18,000 to $35,000) or ambulatory-only Siennas minimize capital requirements while proving market viability before expanding into specialized services.
The Hard Truth About NEMT Profitability
While market projections and revenue calculations paint an optimistic picture, real NEMT business owners face operational challenges that consistently erode margins and test perseverance. Understanding these obstacles—and proven strategies to overcome them—separates sustainable operators from the 70% who exit within three years.
Common Operational Challenges
Cash Flow Strangulation from Payment Delays represents the most immediate threat to new operators. Medicaid brokers and Managed Care Organizations typically process payments 30-90 days after service delivery, with 10-20% of claims initially denied requiring resubmission and extending timelines to 60-120 days. You’re funding driver payroll, fuel, insurance, and maintenance from operating reserves while waiting for revenue from trips completed months earlier. Operators without adequate working capital—typically 3-6 months of operating expenses—face impossible choices: delay driver payments (triggering turnover), skip vehicle maintenance (risking breakdowns), or use expensive invoice factoring at 2-5% fees that further erode already thin margins.
Professional NEMT billing and claims management services can reduce claim denial rates to under 5% through expert documentation and proactive error correction, significantly improving cash flow for new operators.
Insurance Cost Volatility and Surprise Renewals consistently shock operators. Annual premiums of $8,000 to $15,000 per vehicle already strain budgets, but the real crisis comes at renewal when insurers impose 30-50% increases following any claims or risk profile changes. Business owners describe budgeting for $10,000 annual premiums only to receive $15,000 renewal quotes with 30 days’ notice—a $5,000 unexpected expense that can eliminate an entire quarter’s profit. Geographic expansion, adding drivers, or a single at-fault accident can trigger these “surprise audits” that fundamentally alter your cost structure overnight.
The Driver Retention Crisis operates as a constant drain on resources and reliability. Annual turnover rates of 50-100% force perpetual recruitment cycles. Background checks ($50 to $100), drug screening ($30 to $80), training ($500 to $1,000), and onboarding administrative time represent $1,000+ investment per driver—expenditures you repeat multiple times annually for the same position. High turnover also damages service quality as inexperienced drivers commit scheduling errors, provide poor customer service, and increase claim denial rates through improper documentation.
The “Dead Miles” Profit Killer silently consumes 20-30% of potential earnings. These unpaid miles—driving empty to the next pickup location or returning to base after drop-offs—burn fuel, accumulate vehicle wear, and waste driver hours without generating revenue. At the industry average 0.35 unit-hour utilization rate, drivers generate income just 3.5 hours of a 10-hour shift. The remaining 6.5 hours represent pure operational cost that must be absorbed into your per-trip pricing. Operators who fail to optimize routing quickly discover that completing 6 trips requires funding 10 hours of driver time and vehicle operation, making profitable operations impossible at prevailing Medicaid rates.
One of the biggest challenges new NEMT owners face is navigating complex billing requirements across multiple payers. Medicaid, Medicare Advantage, brokers, and private insurance each have different rules, codes, and timelines. Learn the complete NEMT billing process step-by-step before launching your operation.
What Reddit and Forum Users Warn About Most
Real business owners in online communities consistently highlight pain points that don’t appear in business plan templates:
Overdependence on Brokers creates vulnerability where a single entity controls your trip volume and can unilaterally reduce rates. Operators report brokers cutting per-trip reimbursement by $5 to $10 with a 30-day notice, immediately converting profitable routes to break-even operations. The broker’s volume guarantee becomes a trap—you can’t walk away from 70% of your trips even when rates no longer cover costs.
Not Calculating Dead Miles Accurately leads to accepting contracts at rates that appear profitable on paper but lose money in execution. An operator might calculate that a $45 trip with 8 miles driving pays well at $5.62 per mile. However, if the pickup requires 6 miles of empty travel and the drop-off location is 7 miles from the next trip, the true calculation is $45 for 21 total miles—just $2.14 per mile, potentially below your cost to operate.
Drivers canceling Last Minute creates cascading crises. A 6 AM driver no-show means scrambling to cover scheduled trips, potentially driving them yourself, disappointing patients and facilities, and risking contract violations if trips are missed. This operational chaos drives owner burnout and damages relationships with facilities that might otherwise provide steady private-pay referrals.
“Everything Being Up in Price” reflects the 2026 operational reality. Driver wages increased 30% in many markets, commercial insurance premiums rose 40-70%, vehicle costs jumped 30%+, and fuel remains volatile. Medicaid reimbursement rates, however, often stay flat for years. This margin compression means strategies that worked in 2020 no longer pencil out in 2026 without significant efficiency improvements or revenue diversification.
Proven Strategies to Overcome These Challenges
Combat Cash Flow Gaps through strategic financing. Establish a business line of credit before you need it, covering 2-3 months of operating expenses. Use invoice factoring selectively during crunch periods—the 2-5% fee is expensive but cheaper than missing payroll or losing drivers. Most importantly, negotiate payment terms with facilities for direct contracts, securing 7-14 day payment cycles that fund operations while the Medicaid claims process.
Reduce Driver Turnover by implementing technology-enabled scheduling that creates predictable hours. Use performance bonuses tied to trip completion rates and patient satisfaction scores. Invest in competitive base wages ($18 to $25/hour) because the $2/hour premium costs far less than replacing 2-3 drivers annually at $1,000+ each.
Eliminate Dead Miles through AI dispatch software that chains trips geographically and temporally. RouteGenie, Bambi, and TripMaster platforms increase utilization from 35% to 60-80%, often adding 2-3 revenue trips daily per vehicle. The $50 to $200 monthly software cost generates $500 to $1,500 in additional monthly revenue per vehicle through efficiency gains.
Diversify Revenue Sources to reduce broker dependence. Target private-pay dialysis transport ($75 to $150 per trip), build direct contracts with 3-5 senior living facilities, and pursue discharge transportation agreements with hospitals. Even shifting 30% of volume to private pay can increase overall margins from 15% to 25% while reducing vulnerability to broker rate cuts.
NEMT Business Myths Debunked
The non-emergency medical transportation industry attracts entrepreneurs with misleading promises of easy income and simple operations. Separating fiction from reality prevents costly mistakes and sets appropriate expectations for what building a successful medical transport company actually requires.
Common Misconceptions vs. Operating Reality
Myth #1: NEMT is Passive Income Reality: NEMT demands intense, active management requiring 40-60 hours weekly, particularly during startup. You’ll handle real-time dispatch decisions, driver emergencies, facility relationship management, compliance documentation, billing disputes, and operational troubleshooting. Even with excellent systems and staff, owner involvement remains essential for maintaining service quality and financial oversight. Passive income seekers should look elsewhere.
Myth #2: You’ll Get Rich Quickly Reality: Realistic first-year owner earnings from a single vehicle range from $26,000 to $42,000 net—solid income but not wealth-generating. Gross revenue of $50,000 to $60,000 faces substantial operating costs before reaching owner profit. Building to $100,000+ annual income typically requires 2-3 years, scaling to a 5+ vehicle fleet with optimized operations. The path to meaningful wealth involves patient, strategic growth over years, not months.
Myth #3: Anyone Can Succeed in This Business Reality: Success strongly correlates with specific skills and circumstances. Operators with logistics experience, customer service backgrounds, and comfort navigating healthcare regulations significantly outperform those viewing NEMT as simply “driving people around.” Market selection matters profoundly—launching in a saturated urban market with broker-dominated contracts and $25 trip rates virtually guarantees failure, while underserved suburban markets with facility partnership opportunities and $50+ rates offer genuine viability.
Myth #4: Medicaid Rates Ensure Profitability Reality: Medicaid reimbursement creates a financial ceiling, not a profit guarantee. States paying $18 to $35 per trip make profitable operations nearly impossible without extreme efficiency. You need 8-10 trips daily just to cover fixed costs at these rates. Meanwhile, high-rate states offering $45 to $90 per trip allow profitability with 5-6 daily trips, fundamentally changing business economics. The revenue difference isn’t about working harder—it’s about geographic luck and policy decisions beyond your control.
Myth #5: It’s Easy to Start with Just a Van Reality: A van is merely one component of a complex operational system. You also need commercial insurance ($8,000 to $15,000 annually), licensing and permits ($1,000 to $3,000), HIPAA-compliant technology ($1,200+ annually), working capital to survive payment delays ($10,000 to $20,000), trained drivers, facility relationships, and deep knowledge of billing procedures where 10-20% of claims face initial denial. The van might be 60% of your capital investment, but only 20% of actual operational requirements.
Myth #6: The Market Isn’t Saturated Reality: Market saturation varies dramatically by geography. In states like Arizona and Nevada, broker control exceeds 70% of trip volume, provider density reaches 1 per 5,000 residents, and race-to-the-bottom pricing makes new entry extremely challenging. Conversely, underserved suburban corridors in high-reimbursement states show persistent provider shortages with facilities actively seeking reliable partners. Market research—not assumptions—determines opportunity validity.
Setting Realistic Expectations
Timeline to Profitability: Breakeven typically occurs within 6-12 months for well-capitalized single-vehicle operations in favorable markets. Building to sustainable profitability where annual income matches the industry average of $40,000 to $60,000 requires 18-24 months of operation, consistent service quality, and successful facility relationship development. Fleet operations scaling to $100,000+ owner income demand 3-5 years of strategic growth, exceptional operational discipline, and often geographic expansion into multiple service territories. These timelines assume adequate capitalization—underfunded operators extend timelines significantly or fail during the cash flow gap period.
However, these profit margins assume efficient billing operations. A 15% denial rate on $1M revenue means $150,000 left on the table annually. Our comprehensive NEMT billing guide covers the exact KPIs, processes, and strategies that separate top-performing NEMT businesses from struggling operations.
How to Build a Profitable NEMT Business
Success in non-emergency medical transportation isn’t accidental—it results from deliberate strategic choices in market selection, operational systems, revenue diversification, and relationship development. Understanding what separates thriving operators from struggling ones provides a roadmap for sustainable profitability.
Strategic Market Selection
Location Determines Your Financial Ceiling. State Medicaid reimbursement rates create fundamental constraints that no amount of operational excellence can overcome. New York operators earning $45 to $120 per wheelchair trip work in a completely different economic environment than Tennessee providers receiving $18 to $45. Target states where Medicaid rates exceed $30 per trip for ambulatory transport and $60+ for wheelchair service. Within favorable states, focus on suburban corridors with aging populations (15%+ of residents aged 65+) that lack saturated provider networks.
Assess Market Saturation Carefully. Warning signs include broker dominance exceeding 70% of market trips, provider density above 1 per 5,000 residents, and established operators with 95%+ trip completion rates leaving little available volume. Favorable markets show facility complaints about provider reliability, open broker contract slots actively recruiting new providers, and senior living communities without exclusive transportation arrangements. Use NADTC resources and state Medicaid provider directories to quantify existing competition before committing capital.
Operational Excellence Through Technology
AI Dispatch Software Is Non-Negotiable. This single investment transforms economics by increasing vehicle utilization from the industry average 35% to 60-80%. RouteGenie, Bambi, and TripMaster platforms optimize routing to reduce travel time by 15-20%, chain trips geographically to minimize dead miles, automate patient reminders, reducing no-shows by 25-30%, and generate documentation that cuts claim denial rates by similar percentages. The $50 to $200 monthly cost per vehicle generates $500 to $1,500 in additional monthly revenue through efficiency gains alone.
Precision Cost Control Prevents Margin Erosion. Model your unit economics around the industry’s proven cost structure: driver wages consume 35-45% of revenue, vehicle costs (fuel, maintenance, insurance) take 30-40%, and compliance/administrative overhead requires 10-15%. Any deviation—particularly underestimating insurance or fuel costs—quickly erodes profitability. Track cost per mile religiously, targeting $2.50 to $3.50 all-in operating costs for sustainable 20-30% margins at typical reimbursement rates.
Revenue Diversification Strategies
Build a Hybrid Payer Model. Medicaid contracts provide volume stability and predictable demand, but private-pay clients generate superior margins. Target a revenue mix of 50-60% Medicaid/broker trips for baseline volume, 25-35% private-pay dialysis and senior facility contracts at premium rates, and 10-15% healthcare facility discharge transportation and direct insurance contracts. This diversification protects against broker rate cuts while maximizing overall profitability.
Pursue High-Margin Niches Aggressively. Private-pay dialysis transportation represents the single most profitable NEMT segment—recurring trips three times weekly at $75 to $150 per trip with minimal no-shows. A single dialysis patient generates $900 to $1,800 monthly in predictable revenue. Mental health and behavioral health transportation is the fastest-growing segment (10.11% CAGR) as insurance coverage expands, offering premium rates for specialized patient interaction training. Weekend and off-hours wheelchair transport commands 50-100% premiums over weekday rates, directly boosting margins without additional vehicle investment.
Master the Dead Mile Problem. Geographic trip clustering is essential. Rather than accepting trips across your entire metro area, focus on density within 2-3 specific zones where you can chain pickups efficiently. A provider completing 6 trips with an average 3 miles between stops (18 miles revenue, 3 miles dead) operates far more profitably than one covering 6 trips with 8 miles between stops (18 miles revenue, 24 miles dead). The trip count is identical, but operational costs differ by 40%.
Building consistent private-pay volume requires strategic digital marketing for NEMT businesses—including local SEO to capture ‘medical transportation near me’ searches, targeted Google Ads for facility decision-makers, and content marketing that establishes your expertise with healthcare administrators.
Critical Partnership Development
Senior Living Facility Contracts Provide Stability. Approach assisted living communities, independent living facilities, and continuing care retirement communities with dedicated transportation proposals. Offer fixed monthly rates ($2,000 to $4,000) for guaranteed availability covering 10-20 daily trips to medical appointments. These contracts ensure consistent vehicle utilization, eliminate broker fees, enable faster payment (often 15-30 days), and create a predictable cash flow that funds expansion.
Hospital Discharge Partnerships Unlock Premium Rates. Hospital discharge planners coordinate transportation for patients leaving inpatient care—time-sensitive trips, families willingly pay premium rates to secure immediate. Build relationships with discharge departments at 3-5 hospitals in your service area, emphasizing your HIPAA compliance, insurance verification, and same-day availability. Discharge transportation often pays $75 to $150+ per trip, with payment within 30 days directly from hospital billing systems.
Dialysis Center Relationships Generate Recurring Revenue. Each dialysis center serves 60-100+ patients requiring transportation 3x weekly—massive recurring demand. Approach center administrators (not individual patients) with proposals for preferred provider status, offering priority response times and volume pricing in exchange for patient referrals. Even capturing 5-10 patients from a single center generates $3,000 to $9,000 monthly in stable, predictable revenue with extremely low no-show rates due to the life-sustaining nature of treatments.
Ready to Launch Your NEMT Business with Expert Support?
We specialize in helping medical transportation companies:
✅ Website Development – HIPAA-compliant, conversion-ready
✅ Billing Services – Maximize reimbursements, reduce denials
✅ IT Solutions – Secure, compliant technology infrastructure
✅ Digital Marketing – Generate private-pay leads consistently
✅ Financial Planning – Navigate cash flow & tax optimization
How to Market Your NEMT Business Effectively
Marketing a medical transportation service requires a dual approach: digital presence for direct consumer bookings and B2B relationship development for facility contracts. Both channels are essential for sustainable growth and revenue diversification.
Local SEO and Digital Presence
Google Business Profile Optimization drives 40-60% of consumer leads for well-optimized operators. Claim your GBP listing immediately, complete every field, including service areas, hours, services offered, and insurance accepted. Upload high-quality photos of vehicles, drivers assisting patients, and facility partnerships. Most critically, actively solicit and respond to reviews—Google prioritizes listings with 10+ recent reviews in the Local 3-Pack results that dominate “NEMT near me” searches.
Comprehensive digital marketing services for healthcare companies can handle Google Business Profile optimization, local SEO, paid advertising campaigns, and content marketing—generating consistent private-pay leads while you focus on operations.
A Professional Website with HIPAA Compliance isn’t optional for serious operators. DIY website builders create amateur impressions that repel both private-pay clients and facility partnerships. Healthcare facilities conduct due diligence before establishing transportation relationships—an unprofessional website signals operational shortcuts that extend to compliance and service quality. Essential website features include HIPAA-compliant contact forms with SSL encryption, online booking calendars integrated with your dispatch system, clear service area maps, patient testimonials building trust, and a mobile-responsive design since 60%+ of users will access via smartphones. Investment of $3,000 to $10,000 for professional development typically generates 3-5x more qualified leads than template solutions.
Investing in professional NEMT website development services ensures HIPAA-compliant contact forms, real-time booking integration, and the credibility needed to secure facility contracts and private-pay clients.
B2B Facility Partnership Marketing
Healthcare Facility Outreach requires a consultative sales approach emphasizing compliance and reliability rather than price competition. Target discharge planners at hospitals, administrators at senior living communities, center managers at dialysis clinics, and program directors at mental health facilities. Lead conversations with your Business Associate Agreement readiness, HIPAA-compliant communication systems, insurance coverage verification, driver training certifications, and 95%+ on-time performance metrics. Offer trial periods with service level guarantees to overcome initial skepticism.
Relationship Development Tactics that consistently convert include monthly facility visits bringing branded materials and business cards for front-desk staff who influence referrals, hosting educational lunches on transportation resources for facility social workers and discharge planners, offering priority response times or volume discounts for exclusive referral agreements, and implementing white-labeled transportation coordination where your service operates under the facility’s brand for seamless patient experience.
Why Cheap Websites Damage Your Business
Generic template websites actively harm credibility in healthcare markets. They lack HIPAA-compliant form builders requiring signed Business Associate Agreements with vendors, can’t integrate with NEMT-specific dispatch software for real-time booking, suffer from poor mobile optimization, creating 50%+ bounce rates, and signal operational corners-cutting that raises red flags for compliance-focused facility partners. The website’s role isn’t simply informational—it’s a compliance audit that facilities use to assess your operational sophistication before risking patient relationships on your service quality.
How NEMT Compares to Other Transportation Services
Entrepreneurs considering the medical transportation industry often evaluate multiple transportation business models. Understanding the comparative economics, barriers to entry, and market dynamics helps clarify whether NEMT represents the optimal opportunity for your specific circumstances and capital availability.
Business Model Comparison
| Business Type | Profit Margin | Startup Cost | Regulations | Market Demand | Stability |
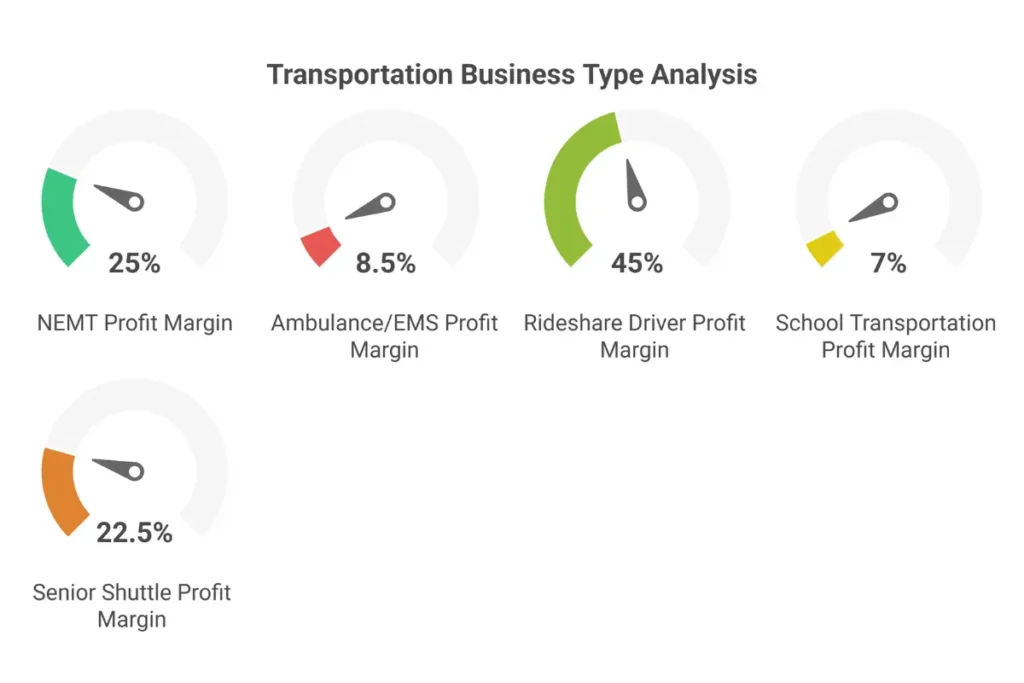
| NEMT | 20-30% | $30K-$50K | Moderate-High | High | Very Stable |
| Ambulance/EMS | 5-12% | $175K-$400K | Extreme | Stable | Very Stable |
| Rideshare Driver | 40-50% of fares | $15K-$25K | Low | Very High | Variable |
| School Transportation | ~7% | $100K-$180K | High | Stable | Seasonal |
| Senior Shuttle | 20-25% | $25K-$45K | Moderate | Growing | Stable |
NEMT’s Competitive Position: Medical transportation occupies the “sweet spot” of moderate barriers protecting against oversaturation, strong profit margins compared to regulated services like ambulance or school transportation, and stable, recession-resistant demand tied to non-discretionary healthcare needs. The 20-30% achievable margins significantly exceed ambulance services (5-12%) and school transportation (~7%) while requiring far less capital than ambulance operations ($30K-$50K vs. $175K-$400K).
Compared to Rideshare: While rideshare driving offers higher percentage margins (40-50% of fares kept by drivers), absolute income proves lower and less stable. NEMT trips pay $40-$60 for scheduled medical appointments compared to rideshare’s $15-$30 for point-to-point trips. More importantly, NEMT generates contracted, recurring revenue from facility relationships and Medicaid brokers rather than competing for variable street hail volume. However, rideshare requires minimal startup investment ($15K-$25K) and virtually no licensing complexity.
Compared to Ambulance Services: Emergency medical services command premium per-trip revenue ($500-$2,500) but face prohibitive entry barriers—EMT/Paramedic certification requiring 100-1,000+ training hours, vehicle costs of $175K-$400K per ambulance, and extreme insurance premiums. NEMT operators serve the same healthcare ecosystem without medical care provision requirements, accessing similar demand with 80% lower capital requirements.
Market Demand and Growth Trajectory
NEMT benefits from the most favorable long-term demand drivers: aging Baby Boomer demographics guaranteeing 10-20 year growth, increasing prevalence of chronic conditions requiring recurring appointments, and federal Medicaid mandates ensuring reimbursement stability regardless of economic cycles. The industry’s projected 7-9% annual growth through 2030 outpaces most transportation segments and operates entirely independent of consumer discretionary spending patterns that impact rideshare volume during recessions.
Ease of Entry Analysis
Easiest: Rideshare driving (minimal requirements, personal vehicle acceptable) Moderate: NEMT and Senior Shuttle (business licensing, commercial insurance, vehicle modifications) Difficult: School Transportation (CDL requirements, seasonal contract competition) Most Difficult: Ambulance/EMS (extensive medical training, extreme capital requirements, complex regulations)
NEMT strikes a balance—higher barriers than pure rideshare create competitive moats and sustainable margins, while lower barriers than ambulance or school transportation enable reasonable startup timelines of 2-4 months from planning to first revenue.
Why Technology Matters for NEMT Success
Technology infrastructure separates marginally profitable NEMT operations from those achieving 25-30% margins. The right software stack doesn’t simply improve efficiency—it fundamentally transforms unit economics and competitive positioning in ways that manual operations cannot replicate.
Implementing and maintaining this technology stack often requires specialized IT services for healthcare businesses to ensure HIPAA compliance, secure data handling, system integration between dispatch and billing platforms, and 24/7 uptime for mission-critical operations.
Essential NEMT Software Platforms
Dispatch and Routing Software represents your most critical technology investment. Industry-leading platforms include RouteGenie ($50 per vehicle monthly), offering strong route optimization for small fleets, Bambi ($69 per vehicle monthly) featuring AI routing that cuts dead miles 25-30%, and TripSpark with custom enterprise pricing for large operations. These platforms increase monthly revenue per vehicle from approximately $3,300 with manual scheduling to $4,160-$5,000—a 26-51% improvement—by optimizing trip sequences, reducing travel time 15-20%, and dynamically rerouting vehicles when cancellations occur.
Integrated Billing and Compliance Tools like TripMaster handle Medicaid claims submission, track denied claims requiring resubmission, manage HIPAA-compliant patient data, and generate trip documentation meeting state audit requirements. Clean claims submission reduces the industry-standard 10-20% denial rate by half, accelerating payment timelines and improving cash flow substantially.
Many operators outsource this complexity to specialized NEMT billing services that handle claim submissions, denial management, and Medicaid reconciliation—reducing the 10-20% denial rate and accelerating payment timelines by 30-50%.
Patient Communication Systems automate appointment reminders via SMS, voice calls, and email, reducing no-show rates from the 15-30% industry average to below 10%. Each prevented no-show saves $35-$75 in wasted operational costs while protecting your trip completion rate metrics that brokers use for preferred provider status decisions.
Website Requirements for NEMT Businesses
A professional medical transportation website must include three non-negotiable elements: HIPAA-compliant contact and booking forms using healthcare-grade encryption and signed Business Associate Agreements with all technology vendors, real-time scheduling integration with dispatch software preventing double-bookings and showing accurate availability, and a mobile-responsive design passing Google’s Mobile-Friendly Test since 60%+ of users access via smartphones.
Our NEMT website development specialists build sites specifically designed for medical transportation companies, with integrated dispatch systems, HIPAA compliance, and conversion-optimized booking flows that attract private-pay clients.
Additional trust-building elements include clear service area maps instantly showing coverage, facility partnership logos demonstrating credibility, patient testimonials addressing reliability concerns, insurance acceptance information, and driver certification details showcasing training investments.
The True Cost of Cheap DIY Websites
Generic website builders create three critical failures: compliance violations through lack of HIPAA-safeguards exposing you to massive fines and facility contract disqualification, operational inefficiency from inability to integrate with NEMT dispatch platforms forcing manual data entry and booking errors, and credibility destruction where amateur design signals unprofessionalism that healthcare facilities interpret as broader operational shortcuts.
Facilities conducting due diligence before establishing transportation partnerships evaluate your website as a proxy for operational sophistication. Template sites with poor mobile experience, missing HIPAA compliance statements, and generic contact forms fail this initial screening, eliminating you from consideration before conversations begin.
ROI of Professional Technology Investment
Operators using integrated NEMT software platforms achieve 40% more leads than those with basic websites, convert at 3-5x higher rates due to real-time booking capability reducing friction, and capture facility contracts that generic providers cannot access due to compliance demonstration requirements. The monthly software investment of $150-$400 per vehicle generates $500-$1,500 in additional revenue through efficiency gains, reduced no-shows, and qualification for premium contracts—a 200-400% monthly ROI that compounds as operations scale.
Future of the NEMT Industry: 2026-2035 Outlook
The non-emergency medical transportation industry stands positioned for sustained growth through 2035, driven by demographic forces that are guaranteed rather than speculative. Understanding these trends and emerging opportunities helps entrepreneurs assess the long-term viability of NEMT business investments.
Powerful Growth Drivers
The Silver Tsunami represents the single most reliable demand driver. With 11,400 Baby Boomers turning 65 daily throughout 2026, the population aged 65+ will reach 73 million Americans by year-end—nearly 20% of the total population. By 2030, all Baby Boomers will exceed 65, guaranteeing an aging population with high chronic disease rates and transportation needs for the next 10-20 years. This demographic shift is irreversible and creates inelastic demand—seniors require medical transportation regardless of economic conditions.
Medicaid Expansion and Enrollment Growth ensure reimbursement stability. Medicaid enrollment is projected to reach 90 million beneficiaries by 2028, with approximately 4-5% utilizing NEMT services annually—translating to 3.6-4.5 million regular users. Federal mandates require states to provide NEMT benefits, making this government-backed demand among the most reliable in healthcare services. Additionally, 21 states increased NEMT reimbursement rates in 2024, with 15 more planning increases in 2026, improving provider economics.
Home Healthcare Growth (10.17% CAGR projected) reflects the broader “aging in place” trend where seniors remain in residential settings rather than institutional care. This shift multiplies transportation needs as patients require regular trips to multiple specialists, therapists, and treatment centers rather than receiving coordinated care in single facilities.
Emerging High-Growth Opportunities
Telehealth Integration creates new transportation patterns. While virtual consultations reduce some appointment volumes, they increase demand for diagnostic testing, lab work, imaging appointments, and pharmacy visits—services that cannot be delivered remotely. Post-telehealth transportation to complete necessary in-person components represents a growing segment.
Mental Health and Behavioral Health Transportation is the fastest-growing application segment at 10.11% CAGR as insurance coverage expands and stigma reduces. These trips often require specialized patient interaction training and command premium rates due to complexity.
Bariatric Patient Transportation addresses the specialized needs of patients requiring oversized vehicles and additional staffing, commanding $200-$300+ premium over standard rates while serving an expanding patient population.
Long-Term Threats and Considerations
Autonomous Vehicles represent a potential disruption on a 10-15 year horizon. Self-driving vehicles from Waymo, Uber, and others could impact 30-40% of ambulatory NEMT trips by 2030+ through lower-cost, on-demand availability. However, regulatory barriers, patient trust issues with vulnerable populations (elderly, disabled), and the need for human assistance during boarding and exiting suggest that wheelchair and specialized transport will remain human-operated indefinitely.
Rideshare Healthcare Partnerships like Uber Health already compete for ambulatory trips in some markets, but their inability to handle wheelchair transport or meet specialized compliance requirements limits market penetration. NEMT operators who focus on wheelchair accessibility and facility relationships maintain strong competitive moats against this threat.
The industry outlook remains strongly positive through 2035 for operators who emphasize specialized services, maintain compliance excellence, and build facility relationships that rideshare platforms and autonomous vehicles cannot easily replicate.
Should You Start an NEMT Business? Decision Framework
Determining whether non-emergency medical transportation represents the right business opportunity for your specific circumstances requires honest self-assessment across operational capabilities, financial resources, and market conditions. This framework helps you make an informed entry decision.
Success Profile: Required Traits and Skills
Operations and Logistics Discipline proves more predictive of success than industry experience. NEMT profitability hinges on mastering scheduling efficiency, route optimization, cost per mile tracking, and utilization rate management. Entrepreneurs with backgrounds in logistics, delivery services, fleet management, or similar operational businesses demonstrate significantly higher success rates than those viewing NEMT as simply “helping people get to appointments.”
Customer Service Orientation and Empathy are foundational requirements. You’re serving vulnerable populations—elderly patients with mobility limitations, individuals with chronic conditions, and people experiencing healthcare anxiety. Patience, clear communication, cultural awareness, and a genuine caregiver mentality separate operators who build sustainable facility relationships from those burning through partnerships due to patient complaints. This isn’t a pure logistics business—it’s a healthcare-adjacent service where bedside manner matters.
Regulatory Compliance Comfort determines whether licensing processes feel manageable or overwhelming. NEMT operators navigate Department of Transportation rules, HIPAA privacy requirements, ADA accessibility mandates, state-specific healthcare licensing, and Medicaid billing procedures. Entrepreneurs who embrace systems, documentation, and structured compliance thrive, while those seeking minimal regulation struggle with the healthcare industry’s oversight intensity.
Warning Signs You Should Reconsider
Market Saturation Indicators include broker contracts with 95%+ trip assignment rates, leaving no available volume, provider density exceeding 1 per 5,000 residents, creating destructive price competition, established operators dominating facility relationships through exclusive contracts, and declining state Medicaid reimbursement rates that no longer cover operational costs, even with maximum efficiency.
Insufficient Capitalization represents the most common failure cause. Starting with less than $30,000 total investment—vehicle, insurance, licensing, working capital—virtually guarantees a cash flow crisis during the Medicaid payment delay period. The 6-month operating reserve isn’t pessimistic cushioning—it’s survival capital that funds operations through the 60-90 day gap between service delivery and payment receipt.
Unrealistic Income Expectations doom operators who require a six-figure income immediately. First-year single-vehicle earnings of $26,000-$42,000 net represent reality. Building to $80,000-$100,000+ annual income requires 3-5 years scaling to fleet operations with exceptional cost control. Entrepreneurs needing a larger immediate income should explore other opportunities.
Starting with Limited Capital: The $10K-$20K Path
Phase 1 – Foundation ($4,500-$9,000): Form LLC ($500-$1,000), secure state licensing and permits ($500-$2,000), and prepay 3-6 months commercial insurance ($3,500-$6,000). This frontloads fixed costs before vehicle acquisition.
Phase 2 – Vehicle ($1,000-$4,000 down): Negotiate a lease or equipment financing agreement for a used wheelchair-accessible van with deferred first payment (90 days out), preserving capital for operations. Target $400-$800 monthly payments on a $30,000-$50,000 financed amount.
Phase 3 – Technology and Go-to-Market ($500-$1,500): Subscribe to essential dispatch software ($50-$200 monthly), apply to Medicaid broker networks immediately (processing takes 60-90 days), and begin facility networking while awaiting approval.
Phase 4 – Working Capital Reserve ($4,000-$6,500): Reserve all remaining funds strictly for fuel, maintenance, and personal living expenses during the 90 days before Medicaid payments arrive and vehicle financing begins. This capital preservation strategy separates successful bootstrap launches from those that fail due to cash depletion.
Market Research Essentials
Before committing capital, investigate four critical factors: State reimbursement rates above $30 per ambulatory trip and $60+ for wheelchair transport indicate viable markets; competitive density below 1 provider per 7,500 residents suggests opportunity; broker market share below 70% of total trips allows competitive entry; and demographic concentration with 15%+ population aged 65+ ensures sustained demand. Use state Medicaid provider directories, NADTC resources, and facility outreach calls to quantify these metrics before launch decisions.
Frequently Asked Questions About NEMT Profitability
Is non-emergency transportation a good business?
Yes, NEMT can be a profitable business for operators who approach it strategically. Average owners earn $40,000 to $60,000 annually with a single vehicle, while fleet operators managing 5-10 vehicles can generate $72,000 to $120,000+ per year. Success depends on your state’s reimbursement rates (high-paying states like New York offer $45-$120 per trip vs. low-paying states like Tennessee at $18-$45), operational efficiency using dispatch software to maximize vehicle utilization, and revenue diversification combining Medicaid volume with higher-margin private-pay clients. The industry benefits from guaranteed demographic growth (11,400 Baby Boomers turning 65 daily) and federally-mandated Medicaid coverage, creating stable long-term demand.
How much can you make in NEMT per month?
A single NEMT vehicle realistically generates $2,500 to $4,700 in monthly net profit after all expenses. Gross revenue typically ranges from $5,000 to $8,000 monthly (completing 5-8 trips daily at $35-$60 average rates across 22 working days), but you must deduct driver wages ($2,000-$2,500), fuel ($400-$600), insurance ($833-$1,250), maintenance ($200-$400), and overhead. Owner-operators who drive their own vehicles can achieve 50-70% profit margins by converting driver wages into owner income. Fleet operations with 5 vehicles generate $6,000 to $10,000 monthly owner profit, though percentage margins compress to 20-30% due to externalized labor and administrative overhead.
Is NEMT profitable in 2026?
Yes, NEMT remains profitable in 2026 despite rising operational costs. The industry is projected to grow from $9.8-$11.8 billion to $15-$19.9 billion by 2030 at 7-9% CAGR, driven by irreversible aging demographics. However, operators must adapt to current realities: driver wages increased 30%, insurance premiums rose 40-70%, and vehicle costs jumped 30%+ since 2020, while Medicaid rates often stayed flat. Success in 2026 requires technology adoption (AI dispatch software boosting revenue 26-51% per vehicle), revenue diversification toward private-pay clients commanding $75-$150 per trip, and rigorous cost control maintaining 20-30% net margins.
How much does Medicaid pay for NEMT?
Medicaid reimbursement varies dramatically by state, ranging from $16-$45 per trip in low-paying Southern states (Tennessee, Georgia, Alabama, Mississippi, Kentucky) to $45-$120 per trip in high-rate Northeastern and West Coast states (New York, California, New Jersey, Maryland, Massachusetts). The national average falls between $25-$50 for ambulatory transport and $60-$100 for wheelchair-accessible services. Research shows state rates can differ by 454% between the highest and lowest payers—this geographic disparity fundamentally determines business viability before you complete a single trip. Check your specific state Medicaid agency website for current published rate schedules.
Can you start an NEMT business with one vehicle?
Absolutely—starting with one vehicle is the recommended approach for most entrepreneurs. This allows you to prove the business model, learn operational complexities, build facility relationships, and achieve profitability before scaling capital requirements. Minimum investment for a single ambulatory vehicle launch is $30,000-$50,000, or $75,000-$120,000 for a wheelchair-accessible van operation. The single-vehicle model works best as an owner-operator where you serve as the primary driver, maximizing profit margins by internalizing labor costs. Once you consistently complete 6-8 trips daily with 25%+ margins, you’ve validated the model and can expand strategically to a second vehicle.
Is NEMT still a good business after broker cuts?
Yes, but margins are tighter, making efficiency and diversification essential. Brokers typically control rate-setting within state-approved ranges, effectively embedding their 10-30% management fee into provider reimbursement before payment. The $40-$60 you receive already reflects broker margin—the state may pay the broker $50-$75 for that trip. Successful operators mitigate broker dependence by diversifying 30-40% of revenue toward private-pay clients (dialysis transport, senior facility contracts, hospital discharge agreements) that eliminate broker fees and pay $75-$150 per trip. This hybrid model uses broker volume for baseline stability while capturing premium margins from direct contracts.
What is the hardest part of running an NEMT business?
According to operator discussions across Reddit and industry forums, the top three challenges are: (1) Driver recruitment and retention with 50-100% annual turnover forcing continuous hiring cycles costing $1,000+ per driver in screening, training, and onboarding; (2) Managing cash flow during 30-90 day Medicaid payment delays while funding payroll, fuel, and operations from reserves, with 10-20% of claims initially denied extending timelines further; and (3) Surprise insurance renewal increases of 30-50% that can eliminate an entire quarter’s profit with just 30 days notice. These operational realities—not competition or demand—cause 70% of new operators to exit within three years.
What is the best state to start an NEMT business?
High-reimbursement states with growing senior populations offer the best opportunity: New York ($45-$120 per trip), California ($40-$110), New Jersey ($40-$100), Maryland ($38-$95), and Massachusetts ($40-$105) create favorable economic environments. However, these states also feature higher operating costs (insurance, wages, compliance) and more competition. Emerging opportunities exist in moderate-rate states (Pennsylvania, Ohio, Texas) with strong suburban markets showing provider shortages—reimbursement of $35-$60 per trip combined with lower insurance costs ($4,500 vs. $7,500+ in major metros) and less saturation can yield superior net margins despite lower gross revenue per trip.
Is NEMT better than rideshare?
NEMT offers more stable income and higher per-trip earnings ($40-$60 vs. rideshare’s $15-$30) but requires significantly more upfront investment, licensing complexity, and business management. NEMT provides contracted, recurring revenue from facility relationships and Medicaid brokers rather than competing for variable consumer demand. However, rideshare allows an immediate start with minimal capital ($15K-$25K), simple onboarding, and flexible scheduling. NEMT suits entrepreneurs building a scalable business asset; rideshare works for those seeking supplemental income with minimal commitment. The decision hinges on your available capital, business-building goals, and tolerance for regulatory complexity.
Do you need a special license for NEMT?
Requirements vary significantly by state. Most states require standard business licensing, commercial vehicle registration, Medicaid provider enrollment (if accepting Medicaid patients), and comprehensive driver background checks. Drivers typically need regular driver’s licenses (not CDL) plus training certifications in HIPAA compliance, CPR/First Aid, wheelchair securement, and patient assistance techniques. Strict states like New York, California, and New Jersey impose additional health department certifications and vehicle age restrictions. Some states, like New York and Virginia, require a Certificate of Need (CON) for stretcher transport services. There is no federal NEMT license, but USDOT numbers apply to vehicles over 10,001 pounds or interstate operations. Consult your state Medicaid agency website for specific requirements.
How many trips per day is good for NEMT?
For single-van operations, 6-8 ambulatory trips or 3-5 wheelchair trips per day represent strong productivity, enabling profitability. This balances driver capacity constraints with realistic scheduling gaps, travel time, and potential cancellations. Top-performing operations using AI dispatch software can achieve 8-10 ambulatory trips daily through optimized routing that chains pickups geographically. At $35-$60 average rates, 6-8 daily trips generate $210-$480 in daily revenue per vehicle, translating to $4,620-$10,560 monthly gross across 22 working days—sufficient for sustainable profitability after expenses. Lower trip counts indicate scheduling inefficiency, market saturation, or insufficient broker/facility relationships requiring operational correction.
Should I start an NEMT business in my state?
Conduct these four assessments: (1) Check your state Medicaid agency website for published reimbursement rates—you need $30+ per ambulatory trip and $60+ for wheelchair transport minimum; (2) Research provider density using state Medicaid directories—markets with fewer than 1 provider per 7,500 residents suggest opportunity; (3) Identify broker market concentration—if brokers control 70%+ of trips with 95%+ assignment rates, limited volume remains for new entrants; (4) Analyze senior population—areas with 15%+ of residents aged 65+ ensure sustained demand. If your state meets 3 of 4 criteria, market entry is viable with proper capitalization and operational execution.
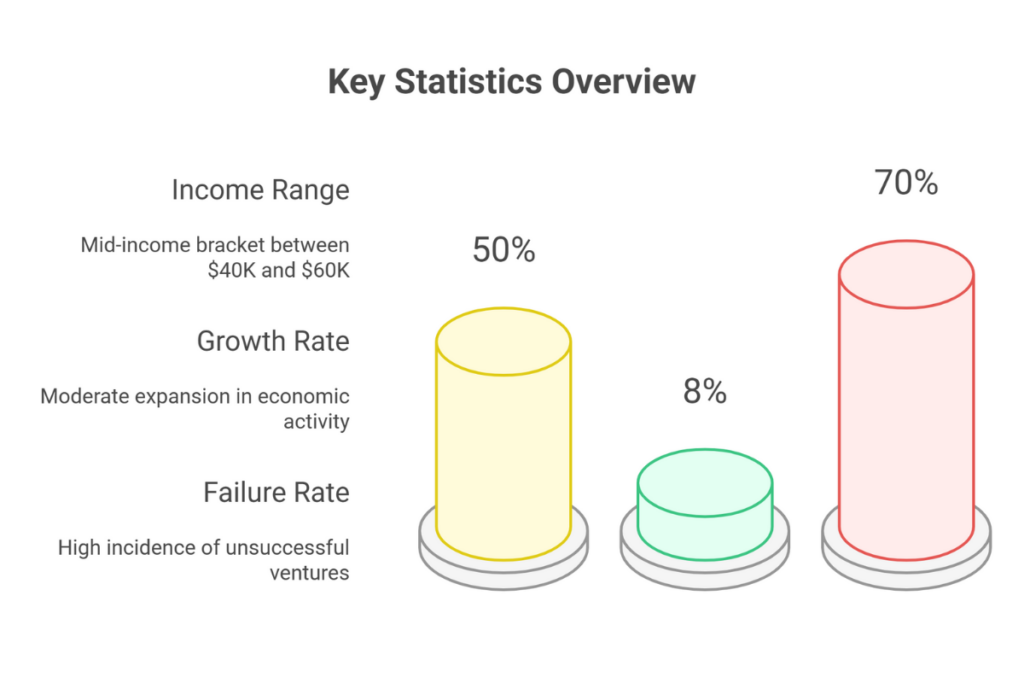
Final Verdict: NEMT Business Viability in 2026
So, is non-emergency medical transportation a good business? The answer is a qualified yes—NEMT offers genuine profitability potential backed by irreversible demographic trends and government-mandated reimbursement, but success requires strategic market selection, operational discipline, and realistic financial expectations.
What the Numbers Show: Single-vehicle owner-operators realistically earn $40,000 to $60,000 annually in favorable markets with efficient operations. Fleet owners managing 5-10 vehicles can achieve $72,000 to $120,000+ in annual income, though this requires 3-5 years of strategic growth and exceptional cost control. These earnings prove sustainable because demand is tied to non-discretionary healthcare needs rather than consumer spending patterns—making NEMT relatively recession-proof compared to most transportation services.
The Critical Success Factors: Your profitability fundamentally depends on state Medicaid reimbursement rates (the 454% difference between highest and lowest-paying states creates completely different economic realities), operational efficiency through technology adoption (AI dispatch software boosting revenue 26-51% per vehicle by eliminating dead miles and optimizing utilization), and revenue diversification beyond pure Medicaid dependence (targeting 30-40% private-pay volume at $75-$150 per trip transforms overall margins from 15% to 25%+).
The Honest Reality: This isn’t passive income or a get-rich-quick opportunity. NEMT requires 40-60-hour workweeks during startup, active daily management of dispatch, drivers, and facility relationships, and patience to reach sustainable profitability. The 70% failure rate within three years reflects inadequate capitalization (the 30-90 day Medicaid payment delay crushes underfunded operators), poor market selection (low-rate states and saturated markets make profitability nearly impossible), and operational inefficiency (manual scheduling at 35% utilization can’t compete against technology-enabled operations at 70%+ utilization).
The Long-Term Outlook: The NEMT industry is positioned for 10-20 years of steady growth as 11,400 Baby Boomers turn 65 daily through 2030 and Medicaid enrollment reaches 90 million+ by 2028. This demographic certainty provides rare business stability—you’re building in an industry with guaranteed, growing demand rather than betting on consumer trends or economic cycles.
Your Action Plan: If NEMT aligns with your circumstances, begin with thorough market research validating your state’s rates and competitive density, secure adequate capitalization including 6-month operating reserves to survive payment delays, start with a single vehicle to prove the model before scaling, invest in technology infrastructure from day one to compete effectively, and build facility relationships aggressively to diversify beyond broker dependence. For those willing to approach NEMT as a legitimate business requiring operational excellence rather than a simple transportation service, the opportunity to build a sustainable, growing income stream serving an essential healthcare need is genuinely available in 2026 and beyond.
Ready to take the next step? Explore our NEMT website development services to give your medical transportation business the professional digital presence that attracts private-pay clients and facility partnerships—or use the research framework in this guide to validate whether your local market offers the conditions for NEMT success.