NEMT Broker Billing Guide 2026: ModivCare, MTM, Veyo & Access2Care
Table of Contents
Why Brokers Control Your NEMT Revenue—And What You Can Do About It
Here’s a number that should concern every NEMT business owner: brokers manage roughly 70% of all Medicaid transportation trips in the United States. That percentage keeps climbing. For most providers, this means one uncomfortable truth—your business depends almost entirely on companies like ModivCare, MTM, Veyo, and Access2Care deciding whether to pay you.
This guide cuts through the confusion surrounding broker billing. We’ll cover exactly how these four major brokers operate, what they demand from providers, and how to get paid faster while avoiding the denials that eat into your profits.
The question providers ask most often is straightforward: How do NEMT brokers handle billing processes efficiently? The short answer is automation combined with strict verification. Brokers use GPS tracking, electronic signatures, and algorithmic claim scrubbing to validate every trip before releasing payment. Understanding this system—and working within it—separates profitable operations from struggling ones.
Whether you’re credentialing with your first broker or managing relationships with all four, this guide gives you the specific steps, timelines, and documentation standards you need to succeed.
What Are NEMT Brokers and How Do They Work?
The Broker Model Explained
An NEMT broker sits between state Medicaid programs and transportation providers. States contract with brokers to manage their entire transportation benefit—everything from member phone calls to trip authorization to claims payment.
Here’s the arrangement in practical terms: The state pays the broker a fixed monthly amount for each Medicaid member. This capitated payment model means the broker keeps whatever money remains after paying providers for completed trips. Their profit depends on efficiency, which explains why their systems are so strict about documentation.
When a Medicaid member needs a ride to a medical appointment, they contact the broker (not you). The broker verifies eligibility, authorizes the trip, and assigns it to a provider in their network. You complete the trip, submit documentation through the broker’s portal, and wait for payment.

Why States Chose This Model:
Before brokers dominated the market, state Medicaid programs managed transportation themselves. The administrative burden proved overwhelming. States dealt with thousands of providers, endless phone calls from members, and fraud that was difficult to detect without technology.
Brokers solved these problems by:
- Centralizing member scheduling through call centers and apps
- Building technology platforms to verify trip completion
- Using GPS and electronic signatures to prevent fraud
- Managing provider networks with standardized credentialing
- Absorbing financial risk through capitated payments
From the state’s perspective, this transfers complexity and risk to private companies. From your perspective, it means working within systems designed primarily to protect the broker’s margins.
Brokers vs Direct Medicaid Contracts
Some providers ask about billing Medicaid directly. In most states, that option disappeared years ago. The broker model now dominates because states found it easier to transfer administrative complexity—and financial risk—to private companies.
The practical difference matters for your billing department:
| Aspect | Direct Medicaid | Broker Billing |
|---|---|---|
| Claims Submission | State Medicaid portal | Broker-specific portal (WellRyde, MTM Link, etc.) |
| Rules and Standards | CMS guidelines | Broker’s internal policies |
| Payment Timeline | State payment schedule | Broker payment cycle |
| Appeals | Medicaid fair hearing | Broker appeals process |
| Your Contract | With the state | With the broker |
Understanding this distinction prevents confusion. Your contract relationship is with the broker. If the broker denies your claim, Medicaid won’t intervene on your behalf.

How Brokers Get Paid (And How You Get Paid)
Money flows in a specific sequence that affects your cash flow planning:
- Federal matching: CMS provides federal matching funds to state Medicaid programs
- State payment to broker: States pay brokers monthly based on enrolled membership
- Trip authorization: Broker authorizes specific trips for eligible members
- Service delivery: You provide transportation
- Claim submission: You submit documentation through broker portals
- Verification: Broker validates GPS, signatures, and coding
- Payment: Broker releases funds for approved claims
The gap between steps 4 and 7 typically ranges from 7 to 45 days depending on which broker you’re working with and whether your claim is clean.
For a deeper understanding of reimbursement rates across different states, see our Medicaid NEMT rates by state breakdown.
The Big Four Brokers: Market Share and Coverage
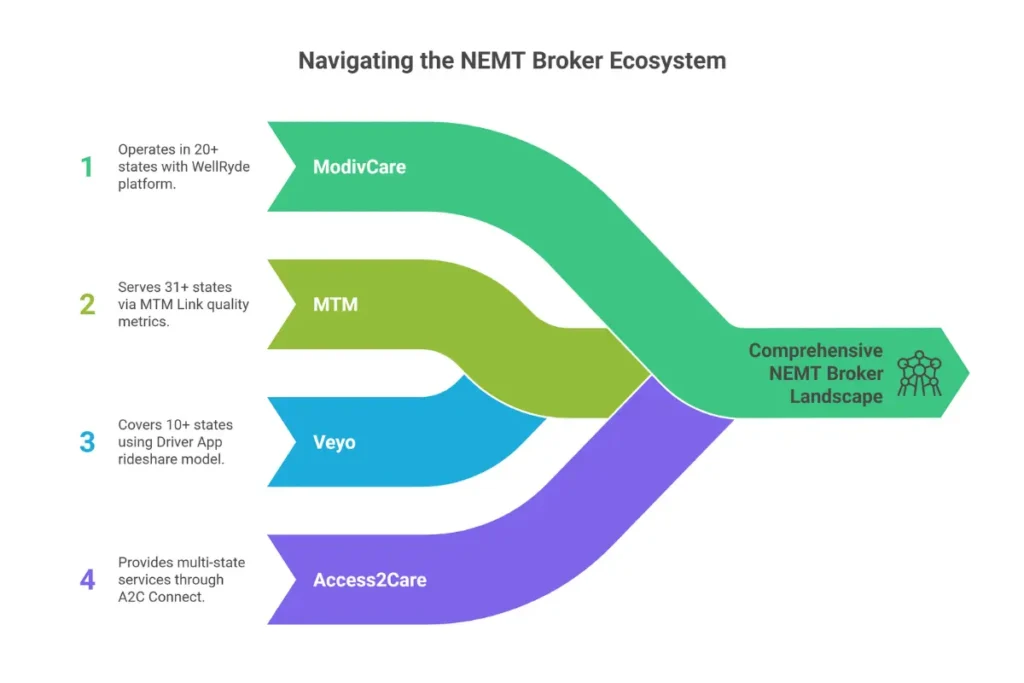
Four companies control most of the NEMT brokerage market. Each operates differently, and understanding their approaches helps you adapt your billing practices.
| Broker | Parent Company | States Covered | Primary Platform | Focus Area |
|---|---|---|---|---|
| ModivCare | ModivCare Inc. | 20+ states | WellRyde | Tech-driven verification, national scale |
| MTM | Medical Transportation Management | 31+ states | MTM Link | Quality metrics, integrated health networks |
| Veyo | MTM (subsidiary) | 10+ states | Veyo Driver App | Rideshare model, fastest payments |
| Access2Care | MTM (subsidiary) | Multi-state | A2C Connect | Hospital discharges, high-acuity transport |
Note that MTM acquired both Veyo and Access2Care, creating an integrated network that shares some compliance data. This matters because termination from one could affect your standing with the others.
ModivCare Billing Guide
ModivCare Company Overview
ModivCare emerged from the combination of LogistiCare and other acquisitions, creating the largest NEMT broker in the country. They operate in over 20 states and process millions of trips annually. Their technology platform, WellRyde, handles everything from trip dispatch to claims adjudication.
What sets ModivCare apart is their emphasis on electronic verification. Every trip generates data points—GPS coordinates, timestamps, signatures—that their system checks before approving payment. This automation speeds up clean claims but creates headaches when data capture fails.
ModivCare Credentialing Requirements
Getting credentialed with ModivCare takes 4 to 8 weeks when you submit complete documentation. Missing documents reset the clock, so prepare everything before starting.
Business Documentation:
- NPI with correct taxonomy code (343900000X for Ambulette services)
- Employer Identification Number (EIN)
- W-9 form
- SAM.gov registration with Unique Entity ID (UEI)
- State business license
- Certificate of Good Standing
Insurance Requirements:
- Commercial auto liability: $1 million CSL minimum
- General liability: $1 million per occurrence, $2 million aggregate
- Workers’ compensation: Statutory limits
- Submit ACORD 25 and ACORD 126 forms with ModivCare listed as certificate holder
Driver Documentation:
- Valid driver’s license (minimum 3 years)
- Multi-state background check (7-year lookback)
- Motor Vehicle Record (MVR) showing clean driving history
- 10-panel drug screening
- CPR/First Aid certification
- Defensive driving certificate where required
Vehicle Requirements:
- Current registration
- Annual state safety inspection
- ADA compliance documentation for wheelchair vehicles
- Lift certification where applicable
- Vehicle age limits vary by state (typically 7-10 years)
- Photos of interior and exterior
For complete compliance documentation requirements, reference our NEMT compliance guide.
ModivCare Provider Portal Navigation
The WellRyde platform serves as your central hub for all ModivCare operations. Bookmark it and check it daily.
Key sections to master:
Trip Board — Shows all assigned trips with status indicators. Filter by date, completion status, or service type. This is where you’ll spot problems before they become denials.
Billing/Claims — Submit manual adjustments, view claim status, and download Explanation of Benefits (EOB) documents. The status column tells you whether claims are pending, paid, or denied.
Reporting — Access your performance dashboards showing On-Time Performance (OTP), complaint rates, and documentation accuracy. ModivCare reviews these metrics quarterly.
Documents — Upload updated credentials here. When insurance renews or driver certifications expire, this is where you submit new documentation.
ModivCare Billing Process Step-by-Step
ModivCare designed their billing process to be automatic—when everything works correctly. Problems emerge when drivers skip steps or technology fails.
Step 1: Trip Assignment Trip appears in driver’s WellRyde app. Driver must accept within the required timeframe.
Step 2: Pre-Trip Verification Before moving, verify member information matches the trip details. Wrong member ID guarantees denial. Call ModivCare support if something doesn’t match.
Step 3: Trip Execution Driver taps “Arrive” in the app within 300 feet of the pickup location. This starts GPS tracking. Collect electronic signature from member or facility staff. Navigate to destination. Tap “Drop Off” on arrival.
Step 4: Automatic Claim Generation WellRyde creates a claim using captured data: GPS breadcrumbs, timestamps, mileage, and signature. This happens automatically if all data points captured correctly.
Step 5: Provider Review Log into the portal within 24 hours. Verify trip details match your records. Attach any external documentation like signed PCS forms that weren’t captured electronically.
Step 6: Submission and Adjudication Submit the claim. ModivCare’s system scrubs it against their rules engine. Clean claims move to payment queue. Problem claims deny with specific reason codes.
ModivCare HCPCS Codes and Rates
ModivCare uses standard HCPCS codes for NEMT billing. Your reimbursement rate is set by your state contract, not the broker.
| Code | Description | Common Use |
|---|---|---|
| T2002 | Non-emergency transport, per trip | Wheelchair van, ambulatory |
| T2003 | Non-emergency transport, stretcher | Stretcher van |
| S0215 | Mileage, per mile | Added to base trip code |
| A0130 | Non-emergency transport, wheelchair van | Alternative to T2002 |
Modifier usage: ModivCare requires specific modifiers based on trip characteristics. Common modifiers include RH (residential to healthcare) and HE (heavy equipment). Using wrong modifiers triggers denials.
For detailed code guidance across all payers, see our complete NEMT billing guide.
ModivCare Payment Timelines
| Claim Type | Expected Payment |
|---|---|
| Clean claim, first submission | 15-30 days |
| Claim with minor corrections | 30-45 days |
| Denied claim after appeal | 45-60 days |
ModivCare pays via EFT (electronic funds transfer). Paper checks are rare and slower. Keep 30-45 days of operating expenses in reserve to bridge payment cycles.
ModivCare Performance Standards and SLAs
ModivCare monitors provider performance through their scorecard system. Falling below thresholds triggers corrective action plans, probation, or termination.
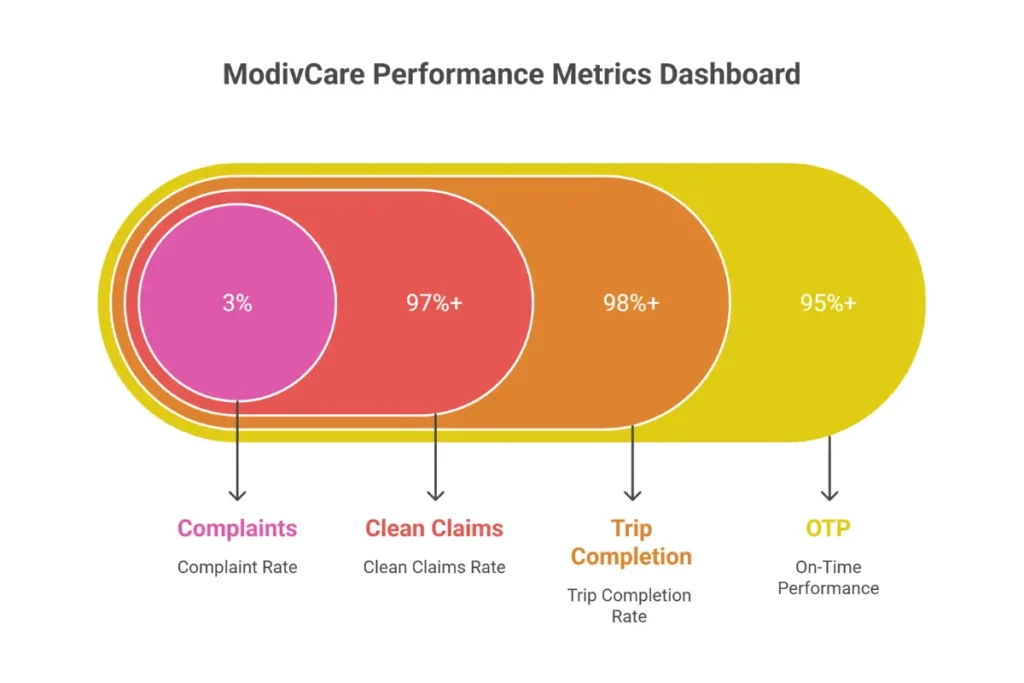
| Metric | Standard |
|---|---|
| On-Time Performance (OTP) | 95% or higher |
| Trip Completion Rate | 98% or higher |
| Clean Claims Rate | 97% or higher |
| Complaint Rate | Below 3% |
Your scorecard appears in the portal reporting section. Review it monthly to catch problems before they escalate.
Common ModivCare Billing Issues and Solutions
| Problem | Root Cause | Fix |
|---|---|---|
| “Unauthorized Arrival” denial | Driver didn’t tap Arrive in app, or GPS showed wrong location | Train drivers on exact app sequence; use app GPS, not separate navigation |
| Missing signature | Member refused or couldn’t sign; facility staff unavailable | Get facility attestation form; take photo as backup evidence |
| Mileage dispute | Odometer reading doesn’t match app GPS route | Sync odometer with app start/end; document detours in trip notes immediately |
| “Invalid Member ID” denial | Wrong ID entered at pickup or trip assigned in error | Verify member name and ID against authorization before starting trip |
| GPS gaps | Signal loss in parking structures or rural areas | Use backup photos showing location signs; document in trip notes |
Managing ModivCare billing while running daily operations stretches most providers thin. Our NEMT billing specialists handle claims submission, denial management, and payment tracking so you can focus on transportation.
MTM Billing Guide
MTM Company Overview
MTM (Medical Transportation Management) operates in over 31 states and emphasizes quality metrics more heavily than most brokers. They acquired Veyo and Access2Care, creating an integrated network that shares compliance data across subsidiaries.
Their approach focuses on care coordination—connecting transportation with healthcare outcomes. This means higher documentation standards and more scrutiny on trip necessity.
MTM Credentialing Requirements
MTM credentialing typically takes 6 to 10 weeks. Their process follows NCQA standards for provider networks, making it more rigorous than some competitors.
Business Documentation:
- NPI and EIN
- W-9 form
- State business license
- SAM.gov registration with UEI
- Signed Provider Service Agreement
Insurance Requirements:
- Auto liability: $1 million CSL
- General liability: $1 million/$2 million
- Workers’ compensation: Statutory limits
- MTM, Inc. must be listed as certificate holder
Driver Requirements:
- Nationwide criminal background check (7-year lookback)
- 10-panel drug screening
- CPR certification
- State-specific training requirements
- Annual re-screening in some states
Vehicle Requirements:
- State inspection
- ADA compliance documentation
- Age limits enforced (typically 10 years maximum)
- Interior/exterior photos
MTM Provider Portal (MTM Link) Navigation
MTM Link centralizes all provider operations. The interface differs from WellRyde but serves similar functions.
Dashboard — Shows alerts, performance scores, and pending actions. Start here each day to catch urgent items.
Trip Management — Schedule, confirm, and cancel trips. The Authorizations tab is critical—never dispatch without checking member authorization status.
Claims Section — Submit claims, search by status, and manage denials. The Claim Batches feature allows submitting multiple trips at once.
Resources — Training guides, state-specific billing rules, and contact information for your Provider Relations representative.
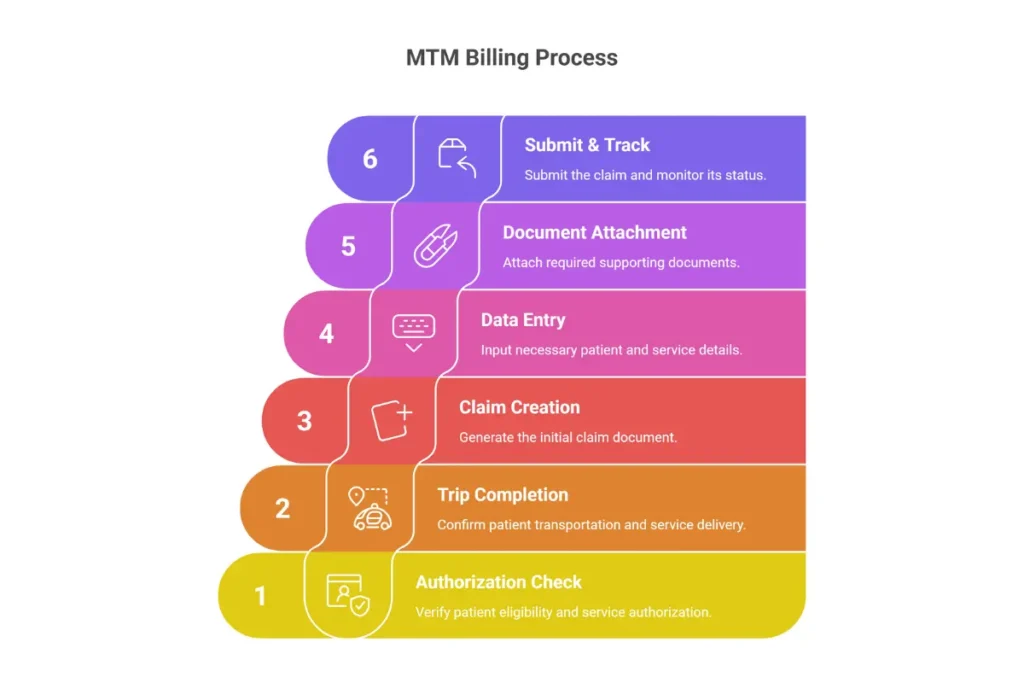
MTM Billing Process Step-by-Step
Step 1: Authorization Check Before dispatch, verify member authorization in MTM Link. Note special instructions or required modifiers.
Step 2: Trip Completion Use MTM Link mobile app or approved telematics device to capture GPS and time data.
Step 3: Claim Creation In the portal, go to Claims → Create New. The system often pre-populates trip data from GPS logs.
Step 4: Data Entry Add HCPCS codes (T2002, T2003, S0215), modifiers matching the authorization, and member date of birth.
Step 5: Document Attachment Attach signed run sheet (manifest) and any required forms. Never submit without the manifest—it’s the primary denial cause.
Step 6: Submit and Track Submit and note the claim ID. Use Claim Search to track status through Pending, Paid, or Denied.
MTM HCPCS Codes and Rates
MTM follows standard HCPCS codes but adds state-specific variations. Wisconsin BadgerCare, for example, has unique modifiers for rural trips. Always reference the billing guide for your specific state contract.
MTM Payment Timelines
| Claim Type | Expected Payment |
|---|---|
| Clean claim | 30-45 days |
| Claim requiring correction | 45-60 days |
| Denied claim after appeal | 60-90 days |
MTM offers EFT or their MTM Currency Card for payment. Regular reconciliation of 835 Remittance files catches underpayments early.
MTM Performance Standards and SLAs
| Metric | Standard |
|---|---|
| On-Time Performance | 95% or higher (within 15-minute window) |
| No-Show/Cancellation Rate | Below 5% |
| Customer Satisfaction | Monitored via post-trip surveys |
| Documentation Compliance | Claims submitted within 72 hours |
Common MTM Billing Issues and Solutions
| Problem | Root Cause | Fix |
|---|---|---|
| “Missing Documentation” denial | Signed run sheet not attached | Make manifest attachment mandatory in billing checklist |
| “Service Not Authorized” denial | Trip dispatched without active prior authorization | Implement rule: no driver moves until dispatch verifies auth |
| “Invalid Provider” denial | Credentials lapsed | Use credential tracker with 60-day renewal alerts |
| GPS variance error | Claimed mileage doesn’t match MTM mapped route | Use MTM-approved GPS; note detour reasons before submitting |
Veyo Billing Guide
Veyo Company Overview (Tech-First Model)
Veyo operates like a healthcare rideshare network. They built their entire system around independent driver providers (IDPs) managed through a smartphone app. This tech-first approach means faster payments but stricter performance requirements.
The model works well for providers who can adapt to app-based operations. Everything happens through the Veyo Driver App—trip acceptance, navigation, signature capture, and automatic claim generation.
Veyo Credentialing Requirements
Veyo onboarding moves faster than traditional brokers—typically 1 to 4 weeks. Their streamlined process suits independent drivers and smaller fleets.
Driver Requirements:
- Age 21 or older
- Valid driver’s license held for 3+ consecutive years
- Clean driving record (maximum 2 violations in 3 years)
- No DUIs in past 7 years
- No major criminal violations in past 5 years
- 10-panel drug screening
- CPR/First Aid certification
- HIPAA training completion
- Compatible smartphone (iOS or Android)
Vehicle Requirements:
- 4 doors (no pickups or 2-door vehicles)
- Seating for at least 5 people including driver
- Pass Veyo 19-point inspection
- Valid registration and insurance
- Model year 2006 or newer (varies by region)
- Space for wheelchair in trunk/back for wheelchair trips
Veyo Driver App and Provider Portal
The Veyo Driver App handles 95% of operations. Fleet owners also access the Veyo Provider Portal for driver management and payment tracking.
App Functions:
- Trip notifications and acceptance
- Turn-by-turn navigation
- Electronic signature capture
- GPS tracking (automatic)
- Will-call return requests
- Earnings and performance tracking
Portal Functions:
- Driver performance monitoring
- Payment reconciliation
- Exception management
- Fleet credential tracking
- Volume and acceptance rate analytics
Veyo Billing Process Step-by-Step
Veyo’s billing is almost entirely passive for providers—which is both its strength and risk.
Step 1: Trip Offer Trip appears in driver’s Veyo app. Seconds to accept.
Step 2: Execution Driver follows app protocol: navigate to pickup, tap Arrive, verify member, collect signature, transport, tap Complete.
Step 3: Automatic Claim App instantly creates claim using captured GPS, mileage, timestamps, and signature. No manual submission.
Step 4: Payment Queue Claim enters weekly payment queue. Clean trips pay automatically.
Step 5: Exception Handling Trips missing signatures or GPS data pend in the portal. Submit corrective documentation through the Exceptions tab.
Veyo Payment Structure
Veyo’s major advantage is payment speed:
| Payment Type | Timeline |
|---|---|
| Clean trips | Weekly EFT (Tuesday/Wednesday for prior week) |
| Exception trips | Next weekly cycle after correction |
| Disputes | 30-60 days |
This weekly payment cycle helps cash flow significantly compared to 30-45 day cycles from other brokers.
Veyo Performance Standards (Strictest in Industry)
Veyo uses algorithmic scoring that directly affects trip offers. Poor scores mean fewer trips.
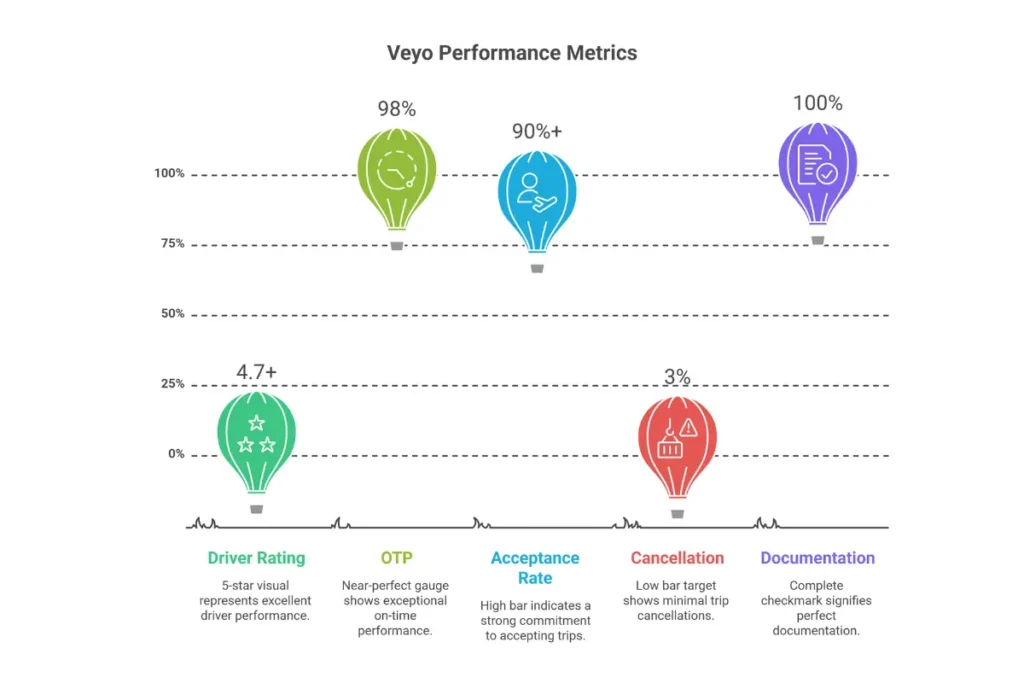
| Metric | Requirement |
|---|---|
| Driver Rating | 4.7+ stars (out of 5) |
| On-Time Performance | 98% |
| Acceptance Rate | 90%+ |
| Cancellation Rate | Below 3% |
| Documentation Completeness | 100% GPS and signature capture |
Common Veyo Billing Issues and Solutions
| Problem | Root Cause | Fix |
|---|---|---|
| “No Signature” hold | Member didn’t sign phone | Train drivers to explicitly request signature |
| “GPS Not Detected” | Location services off or phone in airplane mode | Pre-trip checklist: location ON, WiFi OFF, app refreshed |
| Low trip offers | Driver or fleet performance score dropped | Monitor scores daily; address behavior immediately |
| Missing payment | Trip in Exception status | Check Exceptions tab every Monday before payout |
Access2Care Billing Guide
Access2Care Company Overview (Hospital-Focused)
Access2Care specializes in hospital-based transportation—discharges, inter-facility transfers, and specialist appointments for high-acuity patients. This focus brings higher documentation requirements but often better rates.
Their clinical emphasis means more interaction with hospital discharge planners and nursing staff. Documentation standards reflect healthcare facility expectations.
Access2Care Credentialing Requirements
A2C credentialing takes 8 to 12 weeks—the longest among major brokers. Hospital-specific requirements add complexity.
Business Documentation:
- Standard NPI, EIN, W-9
- State licenses for all operating jurisdictions
- Proof of experience with BLS transport (often requested)
Insurance Requirements:
- Auto liability: $1 million CSL
- General liability: $2 million or higher (hospitals require higher limits)
- Workers’ compensation: Statutory
Driver Requirements:
- Advanced training (BLS, patient handling)
- Health screenings (TB test, immunization records)
- Hospital badge requirements
- Annual competency assessments
Vehicle Requirements:
- Stretcher capability for stretcher contracts
- O2 and suction equipment where specified
- Hospital facility engineering inspection in some cases
A2C Connect Portal Navigation
A2C Connect resembles MTM Link but adds clinical coordination features.
Trip Details — Contains medical information like “NPO after midnight” or “RN to accompany.” Review carefully before dispatch.
Facility Contacts — Direct lines to hospital transport desks. Use these for coordination.
Billing Module — Fields for clinical codes and nurse attestation forms.
For understanding prior authorization requirements specific to hospital transports, see our NEMT prior authorization guide.
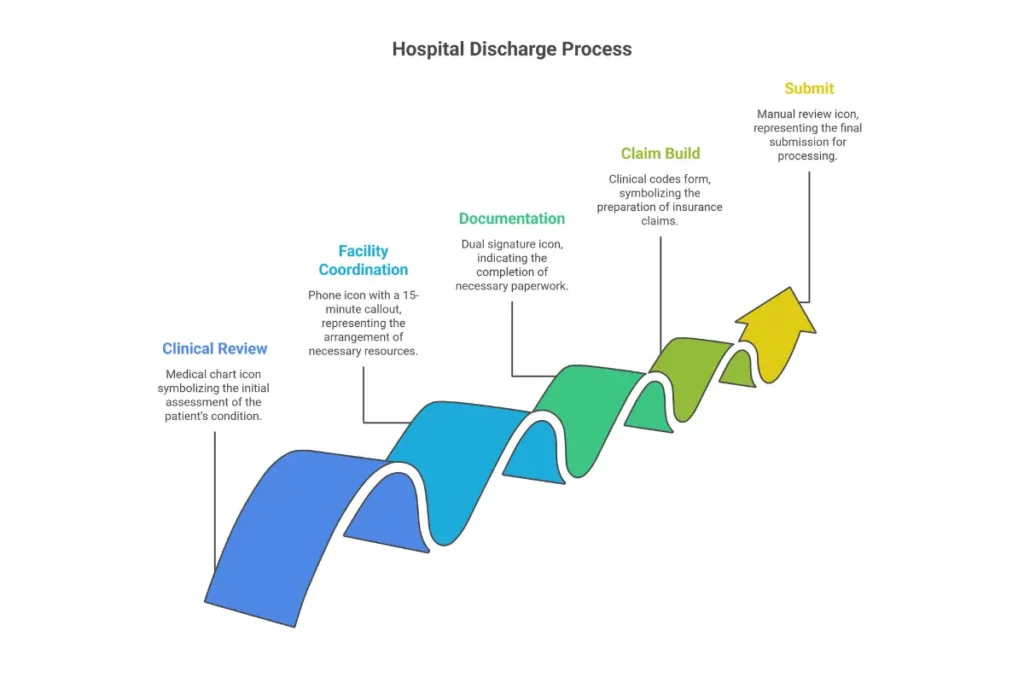
Access2Care Billing Process Step-by-Step
Step 1: Clinical Review Dispatch reviews trip details for medical requirements (oxygen, bariatric, stretcher) and assigns appropriate vehicle and staff.
Step 2: Facility Coordination Driver calls facility transport desk 15 minutes out and again on arrival. This communication is required.
Step 3: Documentation Collect signatures from releasing AND receiving facility staff. A2C often requires a Patient Care Handoff form.
Step 4: Claim Build In A2C Connect, build claim with specific service codes. Attach handoff form and nursing notes.
Step 5: Submit Submit and expect manual review. A2C staff may call for clarification.
Access2Care Payment Timelines
| Claim Type | Expected Payment |
|---|---|
| Clean claim | 45-60 days |
| Claim requiring clarification | 60-90 days |
| Appealed denial | 90-120 days |
The longer timeline reflects manual review processes for clinical trips.
Access2Care Performance Standards
| Metric | Standard |
|---|---|
| Communication Compliance | 100% facility call-in adherence |
| Clinical Documentation | All required forms complete |
| On-Time Performance | 98% |
| Complaint Rate | Below 1% |
Common Access2Care Billing Issues and Solutions
| Problem | Root Cause | Fix |
|---|---|---|
| “Missing Handoff Form” denial | Driver didn’t get both RN signatures | Laminated checklist for drivers: signatures at BOTH facilities |
| “Level of Service” dispute | Documentation doesn’t support stretcher medical necessity | PCS form must state “stretcher” or “non-ambulatory” |
| Long payment hold | Manual review by hospital billing | Designate contact person for quick response to inquiries |
| Credential lapse at hospital | Hospital badge or training expired | Track hospital credentials separately from broker credentials |
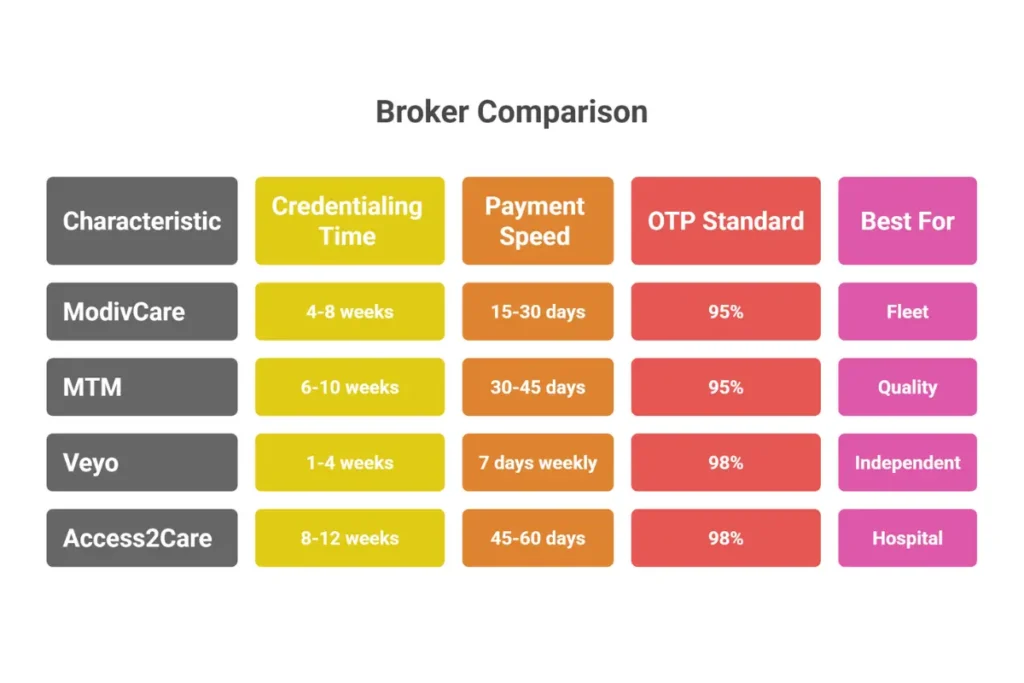
Complete Broker Comparison
Side-by-Side Broker Requirements Comparison
| Requirement | ModivCare | MTM | Veyo | Access2Care |
|---|---|---|---|---|
| Credentialing Time | 4-8 weeks | 6-10 weeks | 1-4 weeks | 8-12 weeks |
| Insurance (GL) Minimum | $1M | $1M | Varies by state | $2M+ |
| Primary Technology | WellRyde | MTM Link | Veyo Driver App | A2C Connect |
| Key Performance Metric | OTP 95%+ | OTP & Complaints | Driver Rating 4.7+ | Clinical Compliance |
| Best For | High-volume fleets | Quality-focused providers | Independent drivers | Hospital-based transport |
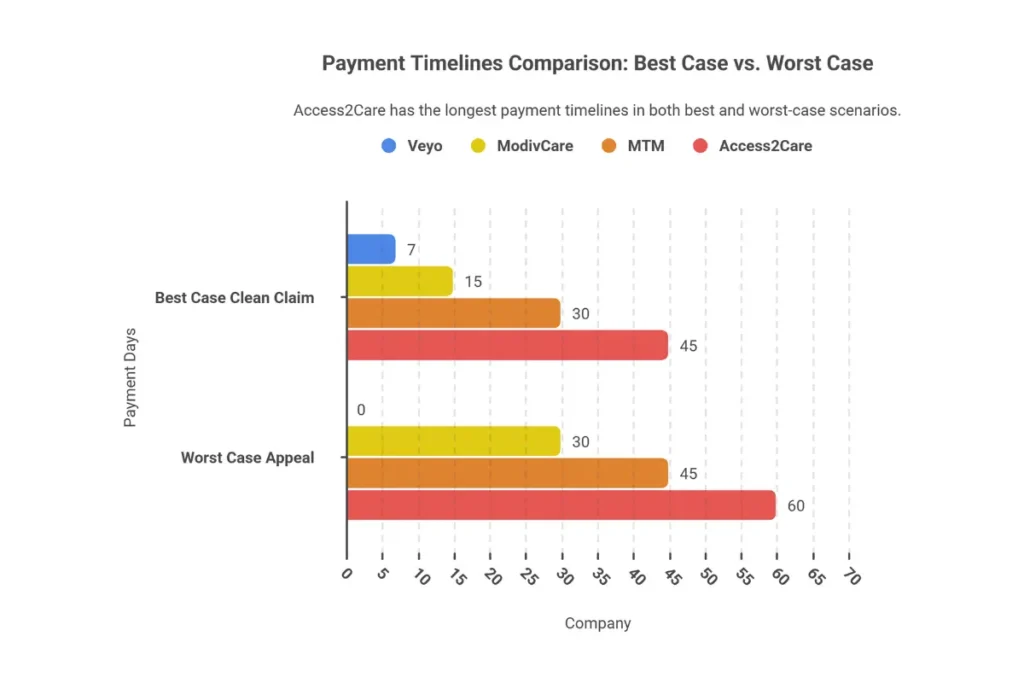
Payment Timeline Comparison
| Broker | Best Case (Clean Claim) | Worst Case (Appeal) | Payment Method |
|---|---|---|---|
| ModivCare | 15-30 days | 60-90 days | EFT |
| MTM | 30-45 days | 75-120 days | EFT/Payment Card |
| Veyo | 7 days | 14-21 days | Weekly EFT |
| Access2Care | 45-60 days | 90-180 days | EFT/Check |
Performance Standards Comparison
| Standard | ModivCare | MTM | Veyo | Access2Care |
|---|---|---|---|---|
| On-Time Performance | 95%+ | 95%+ | 98%+ | 98%+ |
| Clean Claim Rate | 97%+ | 95%+ | N/A (auto) | 98%+ |
| Complaint Rate Limit | <3% | <3% | <2% | <1% |
| Cancellation Limit | <2% | <5% | <2% | <1% |
NEMT Broker Billing Software and Automation
What Software Solutions Are Best for NEMT Broker Billing?
Managing multiple broker portals manually wastes hours and creates errors. The right software consolidates everything into one dashboard.
The best platforms pull trip data from broker systems automatically, scrub claims before submission, and track payments across all your broker relationships. This automation cuts billing staff hours and improves clean claim rates.
For a detailed comparison of available platforms, see our guide on best NEMT software.
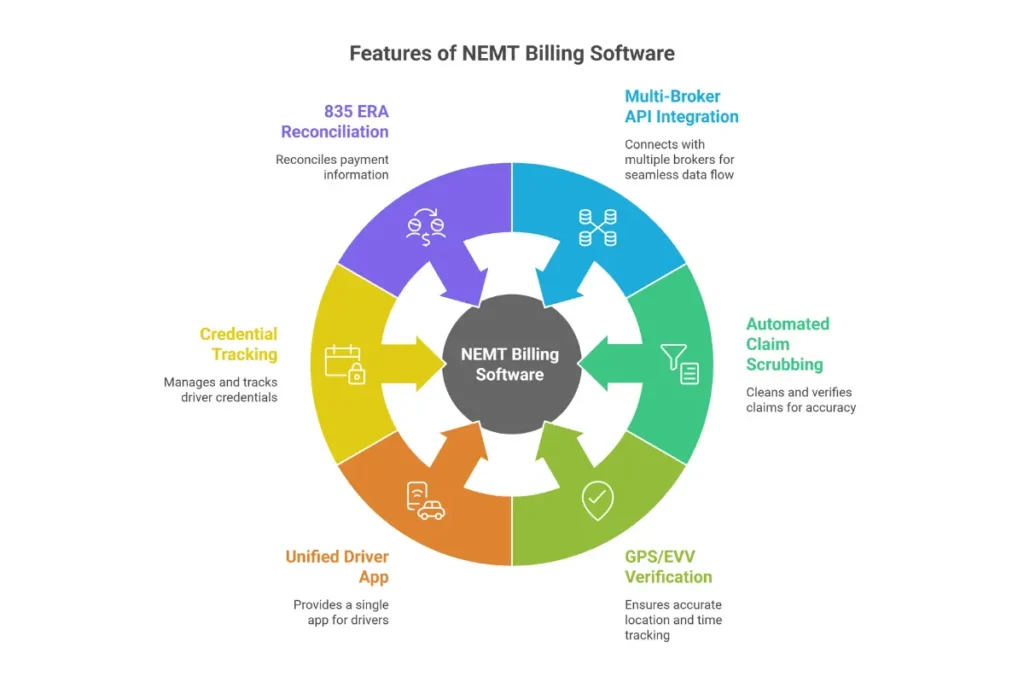
Key Features to Look for in NEMT Broker Billing Platforms
| Feature | Why It Matters |
|---|---|
| Multi-broker API integration | Pulls trips from WellRyde, MTM Link, Veyo automatically |
| Automated claim scrubbing | Catches errors before submission |
| GPS/EVV verification | Imports trip data to support claims |
| Unified driver app | One app for all brokers reduces driver errors |
| Credential tracking | Alerts before licenses and insurance expire |
| 835 ERA reconciliation | Matches payments to claims automatically |
Can You Integrate Billing Software with Broker Scheduling Tools?
Yes. Modern NEMT platforms offer two-way integration:
- Scheduled trips from broker portals flow into your dispatch dashboard
- Trip completion data syncs back automatically
- Claims generate without manual data entry
- Payments reconcile against submitted claims
This closed-loop approach reduces billing errors by 50% or more.
Technology as Competitive Advantage:
Providers who invest in technology outperform those who don’t. The gap shows up in clean claim rates, driver productivity, and customer satisfaction scores.
Beyond billing software, consider your overall digital presence. A professional online presence helps with broker credentialing (some brokers check your website during vetting) and attracts direct-pay customers. For providers building their digital footprint, our NEMT website development services create professional sites that support your growth.
Companies Providing Automated Billing for NEMT Brokers
| Software | Key Strength | Best For |
|---|---|---|
| TobiCloud | Deep billing automation | Maximizing clean claim rates |
| RouteGenie | All-in-one dispatch and billing | Mid-sized fleets wanting one system |
| Bambi | User-friendly interface | Newer companies or high driver turnover |
| MediRoutes | Strong reporting capabilities | Data-driven operations |
| Momentm | Credential management excellence | Companies struggling with compliance lapses |
Not sure which software fits your operation? Our team can assess your billing needs and recommend the right solution—or handle your broker billing entirely.
Managing Multiple Broker Relationships
Multi-Broker Operations Strategy
Running contracts with multiple brokers requires systems, not chaos. Create one unified operation that meets the strictest requirements.
Dispatch: Use software that pulls trips from all brokers into one queue. Drivers shouldn’t need to check multiple apps.
Training: Train everyone on the highest standard (Access2Care’s clinical requirements). Simpler broker trips become automatic.
Billing Team: Organize by function, not broker. One person submits all claims, another handles all denials. This prevents knowledge silos.
Why Multi-Broker Makes Sense:
Relying on a single broker puts your business at risk. When that broker loses a state contract, implements new rules that hurt your profitability, or decides to reduce your trip volume, you have no backup.
Providers with three or more broker relationships report:
- More stable monthly revenue
- Better negotiating position on rates
- Protection against single-broker termination
- Access to different trip types (Veyo for routine, A2C for hospital)
The overhead of managing multiple relationships pays off through stability.
Building Your Multi-Broker Strategy:
Start with one broker and master their system completely before adding another. Each broker takes 3-6 months to truly understand—their quirks, their denial patterns, their payment cycles. Rushing into multiple relationships simultaneously leads to problems everywhere.
When you’re ready to expand, choose brokers that complement your existing relationships. If you have ModivCare’s high-volume routine trips, adding Access2Care gives you hospital business at higher rates. If you’re running Veyo’s rideshare model, MTM offers more traditional scheduling.
Credential Tracking Across Portals
Missing a single credential renewal can halt payments across your entire operation. Use a dedicated compliance platform that tracks:
- Driver license expiration dates
- MVR renewal schedules
- Insurance policy terms
- Vehicle inspection due dates
- Certification renewals
Set alerts for 90, 60, and 30 days before expiration. The cost of tracking beats the cost of suspended payments.
Cash Flow Management with Different Payment Cycles
Veyo pays weekly. Access2Care pays in 60+ days. This spread requires careful planning.
Steps:
- Project next month’s trip volume by broker
- Multiply by average reimbursement rate per broker
- Apply each broker’s payment lag
- Calculate cash needed to cover operating expenses until payments arrive
Maintain a line of credit or cash reserve equal to your longest payment cycle.
Understanding Where Trips Originate:
Your relationship with brokers starts when members book trips. Understanding this process helps you anticipate volume and prepare for busy periods. Members typically book through broker call centers or mobile apps, though some states allow facility-based booking.
For details on how members schedule transportation, see our guide on how to book NEMT.
The booking process affects your operations because:
- Trip lead times vary (24-hour notice vs same-day)
- Standing orders create predictable recurring revenue
- Member no-shows hurt your performance metrics
- Will-call returns require flexible driver availability
Compliance Reciprocity (How Termination Affects All Brokers)
Since MTM owns both Veyo and Access2Care, information flows between them. Termination for fraud or major compliance violations at one broker can trigger investigation by the others.
Even performance-based termination creates risk. Other brokers see your history during re-credentialing. Protect your reputation by meeting standards consistently across all relationships.
Juggling credentials, claims, and payments across four different broker portals? Professional NEMT billing services consolidate your revenue cycle into one streamlined operation.
Broker Billing Best Practices
How to Streamline Billing for NEMT Brokerage Operations
Daily Reconciliation: Close out every completed trip by end of business. Identify missing signatures or GPS issues while driver memory is fresh.
Batch Processing: Submit claims daily, not weekly. This smooths workflow and accelerates payment.
Accountability: Assign one person ultimate responsibility for clean claim rates. They own the number.
Clean Claims Submission
A clean claim gets paid on first submission. Every field matters:
- Accurate patient demographics (DOB, member ID)
- Correct HCPCS codes and modifiers
- Valid prior authorization number
- Complete supporting documentation (PCS forms)
- Accurate provider information (NPI, Tax ID)
- Proper electronic format (no 837P formatting errors)
Documentation Standards
Your documentation must survive an audit three years from now.
Digital-Only: Eliminate paper. Use electronic signatures and cloud storage.
Redundant Verification: Get member signature AND facility staff signature when possible.
Photo Backup: When electronic signature fails, photograph signed manifest with vehicle and location visible.
Denial Prevention Strategies
Prevention costs less than appeals.
Eligibility Verification: Check member status and authorization before dispatch. This stops “Not Authorized” denials.
Driver Accountability: Connect driver incentives to documentation completeness.
Pre-Submission Scrub: Mimic broker adjudication rules before submitting.
For detailed denial code explanations and appeal strategies, see our NEMT denial codes guide.
Appeal Processes by Broker
Each broker has formal appeals processes:
ModivCare/MTM/A2C: Submit written appeal through their portal with claim ID, explanation, and supporting documentation. Follow up after 10 business days without response.
Veyo: Use Trip Exceptions function in provider portal. Faster but less formal.
Universal Rule: Be professional, factual, and persistent. Document every communication.
When to Outsource Broker Billing
Consider outsourcing when:
- Denial rate exceeds 8%
- Billing staff spends 20+ hours weekly on corrections
- Expanding to new brokers without internal expertise
- You’d rather invest capital in fleet expansion than billing staff
Signs Your Internal Billing Isn’t Working:
Your accounts receivable aging report tells the truth. If you’re seeing more than 20% of receivables over 60 days, something is broken. Either claims aren’t submitting correctly, denials aren’t getting worked, or payments aren’t posting properly.
Track these metrics monthly:
- Days in accounts receivable (target: under 35 days)
- First-pass clean claim rate (target: above 95%)
- Denial write-off percentage (target: below 2%)
- Staff hours per claim (target: under 15 minutes)
When these numbers slip, the cost of fixing them internally often exceeds what you’d pay a specialist.
For providers just starting their billing operations, our guide on how to start NEMT billing covers the foundational steps
Common NEMT Broker Billing Challenges and Solutions
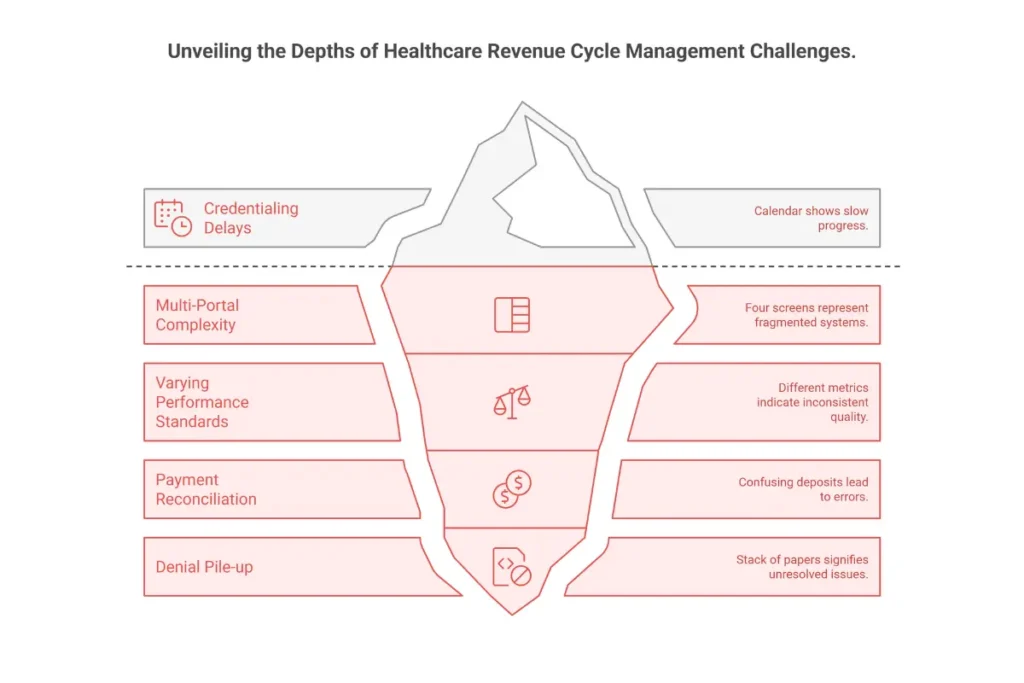
Credentialing Delays and Documentation Gaps
Challenge: Missing driver CPR card halts your entire application for two months.
Solution: Cloud-based compliance management. Give each driver a login to upload their own documents with automated reminders 90, 60, and 30 days before expiration.
Multi-Portal Management Complexity
Challenge: Logging into four portals daily to check trips and payments.
Solution: Integrated software with unified dashboard. If that’s not feasible, create a daily checklist for staff to record key data from each portal in a shared spreadsheet.
Varying Performance Standards Across Brokers
Challenge: ModivCare wants 95% OTP but Veyo’s algorithm punishes you for being late once.
Solution: Set internal standards 5% higher than the toughest broker. Aim for 99% OTP universally.
Payment Reconciliation Across Different Cycles
Challenge: EFT deposits hit your account without clarity on which broker or trips.
Solution: Require Electronic Remittance Advice (ERA 835) from every broker. Use accounting software that imports and posts these files automatically.
Denial Management and Appeals
Challenge: Denials pile up because no one has time to fight them.
Solution: Denial triage system:
- Categorize by reason code
- Prioritize highest-dollar, easiest-to-win denials
- Submit appeals in batches for same denial reason
- Analyze monthly to fix root causes
Frequently Asked Questions
What is an NEMT broker?
An NEMT broker is a company contracted by state Medicaid agencies to manage non-emergency medical transportation benefits. They build provider networks, authorize trips, handle scheduling, and pay providers for completed services. Major brokers include ModivCare, MTM, Veyo, and Access2Care.
How do NEMT brokers handle billing processes efficiently?
Brokers use automated, technology-driven systems. Trips logged through proprietary apps capture GPS, timestamps, and signature data. This auto-generates claims which are scrubbed against rules before payment. Their efficiency depends on providers submitting perfect digital data.
How do I become a ModivCare provider?
Visit the ModivCare provider page, click “Join Network,” and complete the online application. Have all business, insurance, driver, and vehicle documents ready. The process takes 4-8 weeks.
How long does MTM credentialing take?
MTM credentialing typically takes 6-10 weeks from complete application submission. Incomplete applications are the primary delay cause. Contact your assigned Provider Relations representative for status updates.
What are Veyo’s driver requirements?
Veyo requires drivers to be 21+, hold a valid license for 3+ consecutive years, have a clean driving record, pass background and drug screening, complete CPR/First Aid certification, and use a compatible smartphone.
What software solutions are best for NEMT broker billing management?
Integrated platforms like RouteGenie and TobiCloud combine dispatch, billing, and compliance tracking. Bambi offers an easier starting point for smaller operations. Your choice depends on volume, broker mix, and budget.
Which companies provide automated billing for NEMT brokers?
Specialized medical billing companies focus on NEMT. They manage the entire revenue cycle from claim submission to denial management. EliteMed Financials offers comprehensive NEMT billing services.
What features should I look for in an NEMT broker billing platform?
Prioritize multi-broker API integration, automated claim scrubbing, GPS/EVV data import, unified driver app, credential tracking, and 835 ERA reconciliation.
Can I integrate billing software with NEMT broker scheduling tools?
Yes. Advanced software pulls scheduled trips directly from broker portals into your dispatch system. After completion, it pushes claim data back, creating an automated workflow.
What are common billing challenges faced by NEMT providers?
Common challenges include credentialing delays, multi-portal management complexity, varying performance standards, payment cycle differences, and denial management workload.
What payment processing options are available for NEMT broker billing?
EFT (electronic funds transfer) is standard and preferred. Some brokers offer prepaid debit cards. Paper checks are rare and slow. You must provide a voided check and W-9 to set up EFT.
How do I set up electronic billing for an NEMT brokerage?
Obtain your NPI and Tax ID. Enroll with a clearinghouse or get EDI-certified software for 837P generation. Complete EFT/ERA enrollment forms for each broker.
Which NEMT broker pays the fastest?
Veyo pays weekly for auto-verified trips. Among traditional brokers, ModivCare often pays faster (15-30 days) than MTM or Access2Care.
Can I work with multiple NEMT brokers?
Absolutely. Diversification reduces risk and increases volume. The key is using management systems to handle different rules and portals efficiently.
What happens if I’m terminated by one broker?
Termination for cause (fraud, major violations) typically leads to termination by others and state reporting. Performance-based termination may allow re-application after 6-12 months, but you must prove you’ve fixed the issues.
What are the requirements to become an NEMT broker provider?
Core requirements include a valid business license, NPI with appropriate taxonomy code, commercial auto insurance ($1M+ CSL), general liability insurance ($1M-$2M), workers’ compensation, credentialed drivers with background checks and drug tests, ADA-compliant vehicles with current inspections, and technology capability to interface with broker platforms.
How does ModivCare credentialing work?
ModivCare uses a centralized online credentialing system. You submit digital copies of all required documents through their provider portal. Their team verifies each document, often checking with primary sources. Processing takes 4-8 weeks. Final approval grants access to the WellRyde platform for trip management and billing.
What is the MTM Link provider portal?
MTM Link is MTM’s secure web-based interface for providers. It handles trip management, claim submission, document upload, performance reporting, and broker communication. The portal is essential for efficient operations within the MTM network.
How long does it take to get paid by NEMT brokers?
Payment timelines vary significantly: Veyo pays weekly (7 days), ModivCare pays in 15-30 days, MTM pays in 30-45 days, and Access2Care pays in 45-60 days. These timelines assume clean claims on first submission. Any documentation errors reset the clock.
What performance standards do NEMT brokers require?
Universal standards include On-Time Performance above 95%, trip cancellation rates below 5%, high trip completion rates, minimal passenger complaints (below 3%), and clean claim submission rates above 95%. Each broker monitors these metrics through provider scorecards.
How do I submit claims to Veyo?
Veyo claims generate automatically when drivers complete trips correctly in the Veyo Driver App. There’s no manual submission required. Your responsibility is ensuring drivers follow exact app protocol and managing any trips that fall into Exception status in the provider portal.
What documents do I need for broker credentialing?
Universal requirements include business license, articles of incorporation, EIN, NPI, W-9, ACORD insurance certificates (auto/GL/WC), driver MVRs, background checks, drug test results, CPR certifications, vehicle registrations, and inspection reports. Specific requirements vary by broker.
What is compliance reciprocity between NEMT brokers?
Compliance reciprocity means brokers share information about provider terminations, especially for serious offenses. Since MTM owns Veyo and Access2Care, termination by one often triggers investigation by the others. This makes maintaining good standing across all broker relationships critical.
How do I manage billing for multiple NEMT brokers?
Use centralized management software that integrates with all broker portals. If software isn’t feasible, create manual systems including a master credential tracker, unified trip manifest template, and daily portal checklist. Assign broker-specific billing leads for high-volume operations.
What are common reasons for NEMT broker claim denials?
Top denial causes include missing or invalid prior authorization, missing member signatures, GPS data not verifying trip occurred, mileage discrepancies, incorrect HCPCS codes or modifiers, missing PCS forms, and late submission past timely filing limits.
What software is best for managing NEMT broker billing?
RouteGenie offers all-in-one dispatch and billing. TobiCloud provides deep billing automation. Bambi is user-friendly for simpler operations. Momentm excels at credential compliance tracking. The best choice depends on your operational complexity and budget.
How can I automate my NEMT broker billing process?
Automation requires three steps: integrate your software with broker APIs, equip drivers with a unified app capturing all necessary data (GPS, signatures), and implement rules within your software to auto-scrub claims and submit them without manual review for complete trips.
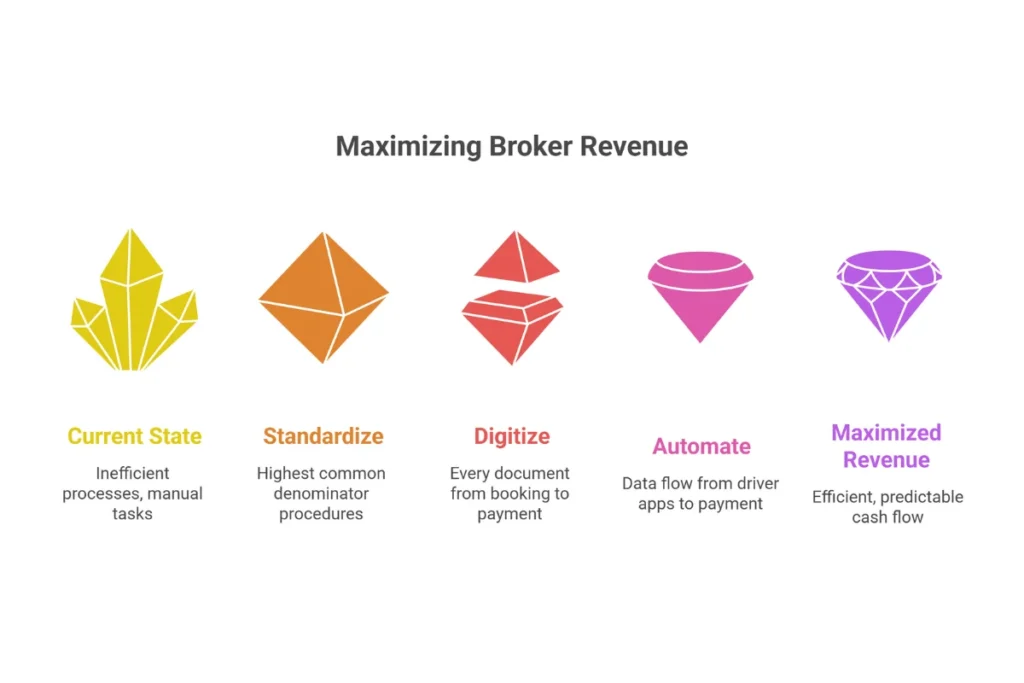
Conclusion: Maximizing Your Broker Revenue
Your revenue from NEMT brokers isn’t just about trip volume. It’s about how perfectly you execute the billing lifecycle for each one. The gap between top-tier providers and struggling operations isn’t fleet size—it’s systems.
Winning means accepting that broker rules are the rules of the game. Your job is building an operation so compliant, so documented, and so efficient that their automated systems have no choice but to pay you quickly and in full.
The path forward is clear: Standardize, Digitize, and Automate. Standardize your procedures to meet the highest common denominator. Digitize every piece of documentation from trip booking to payment posting. Automate the flow of data from driver apps to broker payment systems.
When you do this, you stop fighting denials and start predicting cash flow. You stop worrying about credentialing lapses and start building a reputation as a reliable partner. That’s when brokers start sending you their best contracts.
Whether you’re credentialing with your first broker or managing relationships with all four major brokers, EliteMed Financials’ NEMT billing team maximizes your reimbursements while minimizing administrative burden. Contact us today for a free billing assessment.
For providers wondering whether NEMT is the right business opportunity, explore our analysis of whether NEMT is a profitable business.
For official broker credentialing information, visit the ModivCare Provider Network page.
For federal Medicaid transportation guidelines, reference the CMS Non-Emergency Medical Transportation overview.

