Dialysis patients face a transportation challenge unlike any other in healthcare. Three times every week, without fail, they must reach a treatment center for sessions lasting 3-5 hours, and missing even one appointment can trigger hospitalization or worse.
For NEMT providers, this creates an extraordinary opportunity. Dialysis transportation generates over $3 billion annually in the United States, with a single patient requiring 156 one-way trips per year. Yet billing for these trips correctly—navigating Medicaid requirements, Medicare limitations, broker systems, and compliance rules—remains one of the most complex challenges in medical transportation.
This guide breaks down everything patients and providers need to know about dialysis NEMT billing in 2026, from insurance coverage and HCPCS codes to standing orders and denial prevention.
Why Dialysis Transportation Stands Apart from Other Medical Transport
Dialysis creates transportation demands that dwarf every other chronic condition. Understanding why helps explain the specialized billing and operational requirements.
The numbers tell the story. Over 800,000 Americans currently live with End-Stage Renal Disease (ESRD), and approximately 87% receive in-center hemodialysis. That translates to more than 70 million round-trips to dialysis centers annually—a staggering figure that explains why dialysis dominates the NEMT industry.
Consider the comparison:
| Service | Frequency | Annual Trips | Post-Treatment State |
| Dialysis | 3x weekly, indefinitely | 156 one-way | Fatigued, hypotensive, fall risk |
| Chemotherapy | Cyclical (weeks to months) | 24-48 | Nauseous, weak |
| Physical Therapy | 1-2x weekly for months | 50-100 total | Generally stable |

The financial implications are equally dramatic. Research from the Medical Transportation Access Coalition found that providing reliable NEMT for dialysis patients saves the healthcare system approximately $3,423 per patient per monthby preventing hospitalizations caused by missed treatments. When patients miss dialysis due to transportation failures, hospitalization rates climb from 0.58 per year to 2.1 per year—and mortality risk increases sharply.
For NEMT providers evaluating whetherdialysis transportation represents a profitable business opportunity, these statistics make a compelling case. A single wheelchair patient generates $11,700 or more in annual revenue, with relationships typically lasting 5-10 years.
But dialysis transportation also carries unique operational challenges. Between 30% and 80% of patients experience post-treatment symptoms, including fatigue, dizziness, and hypotension. This means the patient who walks steadily to the vehicle for their morning pickup may need wheelchair assistance and careful monitoring on the return trip. Drivers must understand this variability and accommodate variable treatment end times—sessions can run 30-60 minutes longer than scheduled.
Understanding ESRD Patients and Their Transportation Needs
Successful dialysis NEMT requires understanding who these patients are and what they need.
The dialysis population skews older and sicker than most assume. More than half (51%) are aged 65 or older, with 25% over age 75. The average patient manages 3.2 comorbid conditions alongside kidney failure, with 45% also dealing with diabetes and 40-50% having cardiovascular disease.
These comorbidities directly impact transportation needs:
Mobility Requirements
- Approximately 60% of dialysis patients can walk independently (ambulatory)
- Over 33% use wheelchairs or walkers, requiring wheelchair-accessible vehicles (WAVs)
- Less than 5% require stretcher transport
- 10-20% need an attendant or escort due to cognitive impairment or severe frailty
Insurance Profile
- More than 75% have Medicare coverage (often through ESRD entitlement)
- Approximately 50% are dual-eligible (Medicare and Medicaid)
- Around 35% are enrolled in Medicare Advantage plans
- Only about 10% have employer-sponsored insurance
This insurance mix creates the central billing complexity. Medicare pays for dialysis treatment but generally does not cover transportation. Medicaid covers transportation but only for eligible beneficiaries. Medicare Advantage plans may offer transportation benefits, but with strict limits. Navigating these overlapping systems—correctly—determines whether providers get paid.
Insurance Coverage Explained: Medicare vs. Medicaid vs. Medicare Advantage
The single most common point of confusion in dialysis NEMT billing involves understanding which insurance covers what. Getting this wrong causes denied claims, frustrated patients, and lost revenue.
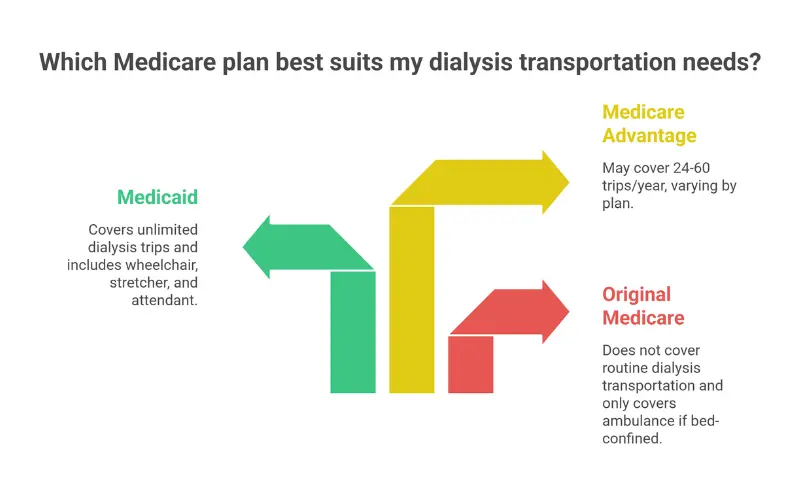
Original Medicare: The Coverage Gap
Original Medicare (Parts A and B) does not cover routine non-emergency transportation to dialysis.
This surprises many patients and even some providers. Medicare’s ESRD program covers the dialysis treatment itself, but getting to that treatment falls outside the benefit. Medicare Part B only covers ambulance transport under strict “medical necessity” criteria—essentially, the patient must be bed-confined and unable to travel safely by any other means.
For the vast majority of dialysis patients who can sit in a wheelchair or vehicle seat, Original Medicare offers no transportation coverage. This creates what policy experts call the “transportation gap”—a significant barrier to care that patients must bridge through other means.
Medicaid: The Primary NEMT Payer
Medicaid is legally required to cover non-emergency medical transportation for all eligible beneficiaries, including dialysis trips.
Under federal regulation 42 CFR § 431.53, state Medicaid programs must “assure necessary transportation” to covered services. Because dialysis is life-sustaining and medically necessary, transportation to dialysis appointments qualifies automatically.
Medicaid NEMT coverage typically includes:
- Unlimited trips for medically necessary appointments
- Wheelchair-accessible vehicles, when documented as needed
- Stretcher transport with proper medical certification
- Attendant/escort services when medically justified
- Standing orders for recurring trip authorization
Each state administers its Medicaid NEMT program differently. Most use transportation brokers (like Modivcare or MTM) to manage scheduling and provider networks. For detailed information on how these broker systems work, see ourcomprehensive NEMT broker billing guide.
Medicare Advantage: Supplemental Benefits with Limits
Many Medicare Advantage (Part C) plans include transportation as a supplemental benefit, but coverage varies significantly by plan.
Approximately 85% of Medicare Advantage plans in 2026 offer some transportation benefit. However, these benefits typically come with annual trip limits—commonly 24 to 60 one-way trips per year. For a dialysis patient needing 156 trips annually, even 60 trips covers less than five months of treatment.
Major Medicare Advantage insurers offering transportation benefits include:
| Insurer | Typical Trip Limit | Notes |
| UnitedHealthcare | ~40 trips/year | Uses Modivcare/rideshare |
| Humana | ~36 rides/year | Varies by plan |
| Aetna/CVS | Unlimited (some D-SNPs) | Broker-based |
| Cigna | ~50 trips/year | Select plans only |
For a deeper exploration of Medicare Advantage transportation benefits and how they work for dialysis patients, see our dedicatedMedicare Advantage NEMT benefits guide.
Dual-Eligible Patients: Best of Both Worlds
Patients who qualify for both Medicare and Medicaid—approximately half of all dialysis patients—have the strongest transportation coverage. For these “dual-eligible” beneficiaries, Medicaid serves as the primary payer for NEMT. They should schedule rides through their state’s Medicaid broker using their Medicaid ID.
Dual-Eligible Special Needs Plans (D-SNPs) often coordinate these benefits automatically, making access simpler for patients who might otherwise struggle to navigate two insurance systems.
The Medicaid NEMT System: Brokers, States, and How to Navigate Them
Understanding how Medicaid NEMT operates in your state is essential for both patients seeking rides and providers seeking payment.
Broker vs. Fee-For-Service Models
States use different models to deliver NEMT services:
Broker Model (Most Common)The state contracts with a transportation broker to manage the entire NEMT benefit. The broker handles scheduling, maintains provider networks, processes authorizations, and often pays claims. Major national brokers include Modivcare (25+ states) and MTM (31+ states).
Fee-For-Service (FFS) Model:Some states or regions pay providers directly through the Medicaid claims system without an intermediary broker. New York’s eMedNY system is an example.
Managed Care ModelIn states with Medicaid managed care, the patient’s managed care organization (MCO) may administer NEMT separately from the state’s general broker system.
State-by-State Reference
Rates and procedures vary significantly by state. For complete reimbursement details, consult ourMedicaid NEMT rates by state guide. Key state contacts include:
| State | Model | Broker | Provider/Member Phone |
| Texas | Broker | Modivcare | 866-424-0147 |
| Florida | Broker (FFS regions) | MTM | 1-844-239-5974 |
| California | Broker via MCPs | Modivcare (regional) | Varies by plan |
| New York | FFS (eMedNY) | State-administered | 1-855-360-3549 |
| Ohio | Broker | MTM | 866-601-7109 |
| Georgia | Broker | Modivcare | 866-601-7106 |
| North Carolina | Broker via MCOs | Modivcare | 833-498-2262 |
Patient Booking Process
For patients learninghow to book NEMT transportation, the process typically works like this:
- Verify Medicaid eligibility using your member ID card
- Contact your state’s broker by phone, app, or online portal
- Provide appointment details, including date, time, clinic address, and mobility needs
- Request a standing order for recurring trips (see next section)
- Receive confirmation with a trip ID number
Most brokers require 24-72 hours’ advance notice for new trip requests, though standing orders eliminate this requirement for recurring appointments.
HCPCS Billing Codes and Modifiers for Dialysis Transportation
Correct coding determines whether claims get paid or denied. Dialysis NEMT uses specific HCPCS codes and requires precise modifier usage.
Essential HCPCS Codes for Dialysis Transport
| Code | Description | When to Use | Typical Rate |
| T2001 | Taxi/sedan transport | Ambulatory patient, standard vehicle | $10-$25/trip |
| T2007 | Wheelchair van | Patient requires WAV | $30-$60/trip |
| A0130 | Wheelchair van w/ ramp/lift | Alternative WAV code (some payers) | $25-$55/trip |
| T2004 | Stretcher transport | Bed-confined patient | $50-$100/trip |
| T2005 | Stretcher with attendant | Stretcher + aide required | $75-$150/trip |
| A0170 | ADL assistance | Escort/attendant only | $40-$70/trip |
| S0215 | NEMT mileage | Per-mile add-on | $2-$5/mile |
| T2049 | Wheelchair van mileage | WAV mileage add-on | $2-$5/mile |

Critical Modifier Rules
Every base transport code requires origin/destination modifiers. These two-character codes indicate where the trip started and ended:
Common Dialysis Modifiers:
- R = Residence (patient’s home)
- D = Diagnostic/therapeutic site (dialysis center)
- J = Freestanding ESRD facility
- G = Hospital-based ESRD facility
- N = Skilled Nursing Facility
Format:First character = Origin, Second character = Destination
Examples:
- Home to dialysis center: RD or RJ
- Dialysis center to home: DR or JR
The most common coding error—and a leading cause of denials—is using invalid modifier combinations like “RR” (home to home) or forgetting modifiers entirely. For a complete breakdown ofNEMT denial codes and how to prevent them, review our denial management guide.
Billing Scenarios
Scenario 1: Ambulatory Patient, Round Trip
- Outbound: T2001-RD (1 unit) + S0215 (12 miles)
- Return: T2001-DR (1 unit) + S0215 (12 miles)
- Note: Bill each leg separately with reversed modifiers
Scenario 2: Wheelchair Patient, Round Trip
- Outbound: T2007-RJ (1 unit) + T2049 (15 miles)
- Return: T2007-JR (1 unit) + T2049 (15 miles)
Scenario 3: Stretcher Patient with Attendant
- Use T2005 (stretcher + attendant) with appropriate modifiers
- Requires Physician Certification Statement documenting “bed-confined” status
For providers just beginning dialysis NEMT billing, ourhow to Start NEMT billing guideprovides foundational instruction on claims submission and documentation.
Standing Orders: The Key to Recurring Trip Authorization
Dialysis patients need transportation three times weekly, every week, indefinitely. Calling to schedule each trip individually would overwhelm patients, brokers, and providers. Standing orders solve this problem.
What Is a Standing Order?
A standing order is a pre-approved, recurring authorization that automatically schedules trips for patients with regular appointments. Once established, the broker’s system generates trips according to the specified schedule without requiring individual booking calls.
Setting Up Standing Orders
The process involves coordination between the dialysis clinic and the NEMT broker:
- Clinic initiates request – The dialysis social worker or administrative staff completes the broker’s standing order form
- Physician certification – A doctor signs a Physician Certification Statement (PCS) documenting medical necessity and transport level
- Schedule documentation – Form includes treatment days (e.g., Mon/Wed/Fri), pickup times, addresses, and special needs
- Submission to broker – Clinic faxes or uploads the completed packet
- Broker approval – Authorization is entered into the system (typically 3-7 business days)
- Automatic scheduling begins – Trips generate according to the approved schedule

Standing Order Duration and Renewal
Standing orders don’t last forever. Duration varies by broker and state:
| Broker | Typical Duration | Renewal Lead Time |
| Modivcare | 90 days | 14 days before expiration |
| MTM | 60 days | 10 days before expiration |
| NY State (eMedNY) | Up to 365 days | 30 days before expiration |
Critical:Letting a standing order expire without renewal causes immediate service interruption. Providers and clinics should track expiration dates and initiate renewals proactively.
For comprehensive guidance onNEMT prior authorization requirements, including standing order procedures for different brokers, see our authorization guide.
Maximizing Revenue from Dialysis Transportation
Dialysis NEMT profitability depends not on high rates—which are fixed by payers—but on operational efficiency. Understanding the math helps providers optimize their service.
Revenue Calculations
Per-Patient Annual Revenue (156 one-way trips):
- Ambulatory: 156 trips × $35/trip = $5,460/year
- Wheelchair: 156 trips × $75/trip = $11,700/year
- Stretcher: 156 trips × $175/trip = $27,300/year
A typical provider serving a mix of patients can expect $8,000-$15,000 in annual revenue per dialysis patient—significantly higher than other chronic conditions and remarkably predictable.

Key Performance Indicators
Successful dialysis NEMT operations track these metrics:
| KPI | Target | Why It Matters |
| Revenue per patient/month | $700-$1,200 | Core profitability measure |
| Trips per vehicle/day | 8-12 | Fleet utilization efficiency |
| On-time performance | >95% | Clinic relationship retention |
| Clean claim rate | >95% | Cash flow and admin costs |
| Vehicle deadhead rate | <20% | Fuel and efficiency loss |
| Denial rate | <10% | Revenue protection |
Route Optimization Strategies
The difference between profitable and marginal dialysis NEMT often comes down to routing efficiency:
Geographic Clustering Group patients by dialysis center and home zip code. Patients within a 3-mile radius of each other and the same clinic create dense, efficient routes.
Shift-Based Scheduling Dialysis centers operate in shifts (morning, afternoon, evening). Align vehicle and driver schedules with clinic shifts—drop morning patients, return for morning pickups, then shift to afternoon routes.
Strategic Vehicle Positioning. After completing trips, position vehicles near the next scheduled pickup rather than returning to a central depot. This reduces deadhead miles significantly.
Multi-Patient Trips. When permitted by the payer and practical given locations, transporting multiple patients in one vehicle increases revenue per route. Use the modifier GM for multi-patient billing.
Preventing Costly Billing Errors and Denials
Dialysis NEMT claims face denial rates of 15-25%—higher than many other healthcare services. Given the volume of dialysis trips, even a small improvement in denial prevention significantly impacts revenue.
Top Denial Reasons and Prevention
| Denial Code | Reason | % of Denials | Prevention |
| CO-197 | Missing/expired authorization | 20-25% | Verify standing order status before every trip |
| CO-15 | Patient eligibility lapse | 12-15% | Check eligibility day-of-service |
| CO-16 | Incomplete documentation | 10-15% | Use EVV with GPS, signatures, timestamps |
| CO-11 | Incorrect coding | 8-12% | Implement coding checklists |
| CO-29 | Timely filing exceeded | 8-12% | Automate deadline tracking |

The EVV Mandate
Electronic Visit Verification (EVV) is now required for Medicaid NEMT in over 45 states. EVV systems must capture:
- Who provided the service (driver ID)
- What service was provided (HCPCS code)
- When the service occurred (timestamps)
- Where the service happened (GPS coordinates)
Claims submitted without compliant EVV data face automatic denial. For providers still developing their compliance frameworks, ourNEMT compliance guidecovers EVV requirements in detail.
Appeal Process
When denials occur, appeals succeed approximately 50-60% of the time—but only if handled correctly:
- Analyze the denial code to understand exactly what went wrong
- Gather supporting documentation: EVV report, signed trip log, PCS form, and eligibility verification
- Submit within the deadline (typically 60 days) through the broker’s appeal portal
- Track and escalate if unresolved after 30-45 days
For complex denial management situations, professionalNEMT billing servicescan significantly improve recovery rates and reduce administrative burden.
Compliance, Credentialing, and Regulatory Requirements
NEMT providers operate in a heavily regulated environment. Compliance failures can result in claim recoupment, exclusion from programs, and even criminal penalties. Understanding these requirements isn’t optional—it’s the foundation of a sustainable business.
Federal Regulations Every Provider Must Know
Anti-Kickback Statute (42 U.S.C. § 1320a-7b)Prohibits offering or receiving anything of value to induce referrals for services payable by federal healthcare programs. This includes giving gifts to dialysis social workers for patient referrals, offering volume discounts that exceed fair market value, or providing free services in exchange for referrals.
Penalty: Up to $100,000 per violation, 10-year exclusion from federal healthcare programs, and potential criminal prosecution
False Claims Act (31 U.S.C. § 3729)Prohibits knowingly submitting false claims for payment—including billing for services not rendered (“ghost trips”), upcoding service levels (billing wheelchair when ambulatory), or falsifying EVV documentation.
Penalty: Triple damages plus $13,000+ per claim in civil penalties
Civil Monetary Penalties Law (42 U.S.C. § 1320a-7a)Limits gifts to Medicaid beneficiaries. Small, nominal gifts under $15 may be permissible if not tied to selecting a specific provider, but the safest approach is to avoid any inducements.
Penalty: $10,000+ per violation
HIPAA (45 CFR Parts 160, 162, 164)protects patient health information. NEMT providers must:
- Execute Business Associate Agreements with brokers and software vendors
- Train all staff and drivers annually on PHI protection
- Secure trip logs, patient information, and electronic systems
- Report breaches within 60 days
Penalty: $100 to $50,000 per violation, up to $1.5 million annually
21st Century Cures Act – EVV MandateRequires Electronic Visit Verification for Medicaid personal care services, extended to NEMT in most states. EVV systems must capture the “who, what, when, where” of every trip using GPS and timestamps.
Penalty: State payment withholding, individual claim denials
Driver Requirements Checklist
Before Hiring:
- FBI/Level 2 fingerprint-based criminal background check
- OIG List of Excluded Individuals/Entities (LEIE) screening
- SAM.gov exclusion database screening
- Motor Vehicle Record (MVR) check—3-year history, fewer than 3 points
- Pre-employment drug test (5-panel minimum, DOT standards if applicable)
- Age 21+ verification
- Valid driver’s license (Class B for larger WAVs if required by state)
- DOT Medical Examiner’s Certificate (for vehicles over 10,001 lbs GVWR)
Ongoing Requirements:
- Monthly OIG/LEIE/SAM exclusion screening (your system should block claims for excluded individuals)
- Quarterly MVR review
- Random and post-accident drug testing
- Annual criminal background check re-verification
- Annual training: HIPAA, Fraud/Waste/Abuse, defensive driving, CPR/First Aid
- DOT medical recertification as required (every 2 years or more often)
- Dialysis-specific training on post-treatment patient care

Vehicle Requirements Checklist
All Vehicles:
- Typically under 7-10 years old (varies by broker—Modivcare allows 10 years, MTM requires under 7)
- Clean, safe, free of odors and damage
- Annual DOT inspection (49 CFR §396.17)
- Daily Driver Vehicle Inspection Report (DVIR) completed before first trip
- $1M combined single limit / $3M aggregate commercial auto liability insurance
- Current registration and appropriate state livery/ambulette plates
- Safety equipment: first aid kit, fire extinguisher, emergency triangles
Wheelchair-Accessible Vehicles (WAVs):
- ADA-compliant (49 CFR Part 38) ramps or lifts with a minimum 800 lb. capacity
- 4-point wheelchair securement systems
- Interior height sufficient for seated wheelchair passengers
- Non-slip flooring
Broker Credentialing Process
Getting credentialed with major brokers takes 30-60 days and involves several steps:
Step 1: Application SubmissionApply through the broker’s provider portal (e.g., provider.modivcare.com, mtm-inc.net/providers). Complete all company information, including Tax ID, NPI, business license details, and service area.
Step 2: Document UploadSubmit required documentation:
- W9 form
- Proof of insurance (COI with required limits)
- Workers’ compensation certificate
- Vehicle registrations and inspection reports
- DOT authority number (if applicable)
- Business license and operating authority
Step 3: Driver Credentialing.For each driver, provide:
- Valid driver’s license copy
- Clean MVR (3-year history)
- Background check results (or authorization to conduct)
- Drug test results
- Training certificates (HIPAA, CPR, NEMT)
Step 4: Review and Possible Site Inspection.The broker reviews your application. Some require an on-site inspection of your facility and vehicles before approval.
Step 5: Contract Execution and Portal AccessUpon approval, sign the provider agreement, set up EFT for payments, and gain access to the scheduling/billing portal.
Credentialing Timeline Comparison:
| Broker | Typical Timeline | Notes |
| Modivcare | 30-45 days | May extend to 90+ days with incomplete documents |
| MTM | 20-40 days | Generally faster approval process |
| Veyo | ~14 days | Streamlined app-based credentialing |
| SafeRide | 14-30 days | Regional focus |
Building a Compliance Program
The OIG recommends seven elements for an effective compliance program:
- Written Policies and Procedures – Document standards for billing, driver conduct, HIPAA, and gift/referral policies
- Compliance Officer and Committee – Designate someone responsible for oversight
- Effective Training – Annual training for all staff on FWA, HIPAA, and company policies
- Lines of Communication – Confidential hotline for reporting concerns
- Internal Monitoring and Auditing – Monthly claim audits, quarterly driver file reviews
- Consistent Discipline – Documented, fair consequences for violations
- Prompt Response – Investigate issues and implement corrective actions
For providers serious about building their dialysis NEMT operations, investing in propermedical billing servicesensures compliance from day one.
Partnering with Dialysis Centers for Sustainable Growth
The most successful dialysis NEMT providers build strong relationships with dialysis centers. These partnerships create reliable patient volume and operational efficiency that transforms business outcomes.
The Dialysis Center Landscape
Two companies dominate the U.S. dialysis market:
- DaVita: 2,657 U.S. centers, ~37% market share
- Fresenius Medical Care: 2,600-2,800 U.S. centers, ~38% market share
The remaining market includes regional chains (US Renal Care with 550+ centers, Dialysis Clinic Inc. with 300+ centers), hospital-based units (~500 locations), and approximately 1,200 independent centers. Independent centers often offer the fastest path to partnership—decisions happen locally rather than through corporate vendor processes.
Key Contacts at Dialysis Centers
| Role | Responsibilities | How to Engage |
| Social Worker | Coordinates NEMT, documents missed rides, and manages standing orders | Primary contact—provide reliability data and a dedicated phone line |
| Facility Administrator | Approves vendors, manages contracts | Formal business approach with insurance documentation |
| Charge Nurse | Manages patient flow, knows treatment end times | Coordinate for “patient ready” notifications |
| Patient Care Technicians | Direct patient care, know real-time status | Brief, clear communication for smooth handoffs |
Research indicates that dialysis social workers spend 25-40% of their workday managing transportation issues. When you solve this problem, you earn not just their business but their loyalty and referrals.

Building Partnerships Step-by-Step
Phase 1: Research and Approach
- Identify target centers in your service area using ESRD Network lists
- Research whether they use a primary broker or work with direct vendors
- Prepare a “reliability one-pager” showing your on-time performance, fleet capabilities, and dialysis experience
- Contact the social worker or facility administrator by phone or in-person visit
Phase 2: Demonstrate Value5. Offer to handle their most challenging routes (early morning, rural, bariatric) 6. Propose a free trial period for a subset of patients 7. Provide a dedicated contact number for the clinic 8. Establish clear communication protocols for delays, no-shows, and emergencies
Phase 3: Formalize and Scale9. Document the relationship in a written agreement (preferred vendor, exclusive for certain routes, or volume-tiered contract) 10. Implement monthly performance reporting (on-time rate, complaints, patient satisfaction) 11. Expand services based on demonstrated reliability
Service Level Expectations
Clinics hold NEMT providers to high standards. Meeting these benchmarks is essential for partnership retention:
| Metric | Expected Standard | Consequence of Failure |
| On-time arrival | 95-98% within 15-minute window | Partnership at risk below 90% |
| Post-treatment wait | <10 minutes from “patient ready.” | Clinic frustration, complaints |
| Missed trip rate | <5% | Immediate patient health risk |
| Driver professionalism | Name badges assist with boarding | Reflects poorly on the clinic |
| Issue resolution | Acknowledge within 24 hours | Loss of trust |
Communication Best Practices
When a patient is ready for pickup,the driver checks in with the charge nurse or patient care technician. Dispatcher confirms pickup via your dedicated clinic contact.
When there’s a schedule change:Clinic social worker notifies your dedicated dispatcher 48-72 hours in advance. Confirm receipt and update standing order.
When there’s a problem:Acknowledge within 24 hours. Take ownership, compensate with a priority service if appropriate, and report back with a prevention plan.
When there’s a major incident (late/missed trip):Call the social worker immediately while troubleshooting. Dispatch a backup vehicle. Follow up with a formal incident report
Technology and Software for Dialysis NEMT
Modern NEMT operations require technology that handles recurring scheduling, EVV compliance, broker integration, and billing automation.
Essential Software Features for Dialysis
- Recurring trip templates for Mon/Wed/Fri schedules
- Standing order management with expiration tracking
- Integrated EVV (GPS, timestamps, e-signatures)
- Broker API connectivity (Modivcare, MTM)
- Automated HCPCS coding with modifier logic
- Route optimization for geographic clustering
- Real-time driver tracking with ETA sharing
Software Comparison
| Platform | Key Strengths | Broker Integration | Price Range |
| TripMaster | Enterprise-grade, comprehensive | EDI-based | $500-$2,000/mo |
| RouteGenie | AI routing, cost-effective | Partial | $99-$499/mo |
| NEMT Cloud Dispatch | Strong Modivcare/MTM APIs | Excellent | $150-$800/mo |
| Tobi Cloud | User-friendly, recurring trips | Good | $200-$1,000/mo |
For detailed platform comparisons and selection guidance, see ourbest NEMT software guide.
Providers needing custom technology solutions—including patient portals, booking systems, and dispatch interfaces—may benefit from specializedNEMT website development services.
Alternative Transportation Resources for Patients
When insurance coverage falls short, patients need to know where else to turn. These resources fill critical gaps.
Charitable and Community Programs
| Resource | Contact | Who Qualifies |
| American Kidney Fund (AKF) | 1-800-638-8299 | Low-income dialysis patients |
| National Kidney Foundation | 1-800-622-9010 | ESRD patients (local chapters) |
| Area Agency on Aging | 1-800-677-1116 | Age 60+ |
| VA Beneficiary Travel | 1-877-222-8387 | Enrolled veterans |
| 2-1-1 Information Line | Dial 2-1-1 | General public |
Rideshare Options
Uber Health and Lyft Healthcare allow clinics to schedule medical rides for patients. These work best for:
- Ambulatory patients only (limited wheelchair access)
- Short distances
- Patients who are stable post-treatment
However, rideshare is not appropriate for patients experiencing post-dialysis hypotension or those who need physical assistance.
Family Mileage Reimbursement
In approximately 15 states, Medicaid offers mileage reimbursement programs for family members who drive patients to appointments. Rates range from $0.20-$0.67 per mile. The driver must apply to become an approved Individual Transport Provider (ITP).

Frequently Asked Questions
Does Medicare cover transportation to dialysis?
Yes. Under federal law (42 CFR § 431.53), Medicaid must provide non-emergency medical transportation for all eligible beneficiaries. Dialysis trips are covered without annual limits when arranged through your state’s designated broker.
Does Medicare Advantage cover dialysis transportation?
Many Medicare Advantage plans include transportation as a supplemental benefit—approximately 85% offer some coverage. However, these benefits typically come with annual trip limits of 24-60 one-way trips, which cover only 2-5 months of thrice-weekly dialysis appointments.
How many trips does Medicaid cover for dialysis?
Medicaid coverage for dialysis transportation is effectively unlimited because dialysis is medically necessary. Standing orders authorize all recurring trips (typically 156+ one-way trips per year). There are no annual caps like those found in Medicare Advantage plans.
Is wheelchair transportation covered for dialysis patients?
Yes, when medically necessary. A Physician Certification Statement (PCS) documenting the patient’s mobility limitation is required. Brokers then dispatch wheelchair-accessible vehicles with ramps/lifts and securement systems.
Can a family member ride with me to dialysis?
Yes, if medically necessary. When a patient has cognitive impairment, severe frailty, or medical instability requiring assistance, an escort/attendant is typically covered. The need must be documented by a physician.
What if I have both Medicare and Medicaid (dual-eligible)?
You have the best coverage available. For transportation, use your Medicaid benefit by calling your state’s NEMT broker. Medicaid is the primary payer for transportation, while Medicare pays for your dialysis treatment.
Can my family member get reimbursed for driving me to dialysis?
In approximately 15 states, Medicaid offers mileage reimbursement programs for family members who drive patients to appointments. The driver must apply to become an approved Individual Transport Provider (ITP) and submit mileage logs. Rates range from $0.20-$0.67 per mile.
What if I don’t have Medicaid, and Medicare won’t cover my rides?
Explore alternative resources: Medicare Advantage plans may offer supplemental transportation, the American Kidney Fund (1-800-638-8299) provides transportation grants, Area Agency on Aging (1-800-677-1116) offers rides for those 60+, and your dialysis social worker can connect you with local programs.
How do I schedule Medicaid transportation for dialysis?
Call your state’s designated Medicaid NEMT broker (such as Modivcare or MTM) using your Medicaid member ID. Provide your appointment details, pickup address, and any special mobility needs. For recurring dialysis trips, ask about setting up a standing order through your clinic.
How far in advance do I need to book my dialysis ride?
Most brokers require 24-72 hours’ advance notice for new trip requests. However, setting up a standing order through your dialysis clinic eliminates this requirement—rides are automatically scheduled according to your treatment schedule.
What if my Medicaid ride doesn’t show up?
Call the broker’s support line immediately to report the no-show. They can track the assigned vehicle and dispatch a backup. Also, inform your dialysis clinic social worker, who can advocate on your behalf and document the incident for grievance filing if needed.
How do I set up recurring rides for dialysis?
Your dialysis clinic social worker completes a standing order form, which your doctor signs. The clinic then submits this to the NEMT broker. Once approved (typically 3-7 business days), rides are automatically scheduled for your treatment schedule without requiring individual booking calls.
What information do I need to book a Medicaid ride?
Have ready: your Medicaid member ID, full name and date of birth, pickup address, dialysis center name and address, appointment time, your mobility needs (ambulatory, wheelchair, or stretcher), and whether you need an escort or companion.
Can I cancel or change my scheduled ride?
Yes, but most brokers require at least a 2-hour notice for cancellations. Late cancellations or no-shows may count against you—after multiple violations, services could be suspended. For schedule changes, notify the broker 48-72 hours in advance.
What if my ride is late and I might miss dialysis?
Call the broker immediately—they can track your driver and provide an updated ETA or dispatch a backup. Call your dialysis clinic to inform them. Most clinics can accommodate late arrivals, but they need advance notice.
Can someone ride with me to my dialysis appointment?
Yes, if medically necessary. When you have cognitive impairment, severe frailty, or need physical assistance, an escort/attendant is typically covered. Your doctor must document this need. Family members can often accompany you with prior broker approval.
What HCPCS code do I use for wheelchair transport to dialysis?
The standard codes are T2007 or A0130 for wheelchair van transport. Always append the appropriate origin/destination modifier (e.g., RD for residence-to-dialysis, JR for dialysis-to-residence). Include the ESRD diagnosis code N18.6.
How much does Medicaid pay for dialysis NEMT?
Rates vary significantly by state: $25-$90 for ambulatory trips, $50-$150 for wheelchair van trips, plus mileage add-ons ($2-$10/mile). Payment typically arrives 30-45 days after a clean claim submission.
What are the most common NEMT claim denials?
The top denial reasons are: missing/expired prior authorization (CO-197), patient eligibility lapse (CO-15), incomplete documentation (CO-16), and incorrect coding/modifiers (CO-11). Prevention requires pre-trip verification, same-day eligibility checks, and compliant EVV documentation.
How do I become a Medicaid dialysis transportation provider?
First, enroll with your state Medicaid agency. Then complete credentialing with the state’s NEMT broker(s)—typically Modivcare or MTM. Submit proof of insurance ($1M/$3M liability), vehicle registrations/inspections, and driver credentials. The process takes 30-60 days.
How do I bill for recurring dialysis trips?
Each trip is billed individually using the same per-trip codes (T2007, A0130, etc.) with appropriate modifiers. The standing order provides authorization, but you must submit separate claims for each completed trip. Billing software can generate claims automatically from completed trip data.
What documentation do I need to support each claim?
Essential documentation includes: EVV data (GPS coordinates, timestamps, driver ID), patient or clinic staff signature, trip log with addresses and mileage, reference to the valid standing order or prior authorization, and a current PCS form on file for the patient’s documented service level.
How do I appeal a denied NEMT claim?
Analyze the denial code, gather supporting documentation (EVV report, signed trip log, PCS form, eligibility verification), and submit an appeal through the broker’s portal within 60 days. Include a cover letter referencing the claim ID and denial code, explaining why the denial was incorrect.
Can I bill Medicaid and Medicare Advantage for the same patient?
No—patients have one primary payer for transportation. Dual-eligible patients use Medicaid for NEMT. For Medicare Advantage patients (without Medicaid), the MA plan is the payer. Never bill both for the same trip.
What vehicle requirements exist for dialysis NEMT?
Vehicles must typically be under 7-10 years old, pass annual DOT inspections, and carry required commercial auto insurance ($1M/$3M). Wheelchair-accessible vehicles need ADA-compliant ramps/lifts (800+ lb capacity), 4-point securement systems, and sufficient interior height for seated passengers.
How do I partner with dialysis centers?
Contact the clinic’s social worker or facility administrator. Demonstrate reliability (target 98%+ on-time performance), offer to handle their most challenging routes, provide a dedicated contact number, and share monthly performance reports. Start with independent centers for faster decisions.
What KPIs should I track for dialysis NEMT operations?
Focus on: revenue per patient per month ($700-$1,200 target), trips per vehicle per day (8-12 target), on-time performance (>95%), clean claim rate (>95%), denial rate (<10%), vehicle deadhead rate (<20%), and no-show rate (<10%).
How do I reduce no-shows and cancellations?
Implement automated SMS reminders 48 hours and 24 hours before pickup. Partner with clinics for day-of verification. Enforce a clear cancellation policy. Maintain a waitlist to backfill canceled slots. Track and address chronic no-show patients through their social workers.
What happens if a patient becomes ill during transport?
NEMT drivers are not paramedics. In emergencies, drivers should stop safely, call 911 immediately, provide first aid as trained, stay with the patient until EMS arrives, and notify dispatch to inform the clinic.
How long does broker credentialing take?
Typically 30-60 days: Veyo is fastest at approximately 14 days, MTM takes 20-40 days, and Modivcare takes 30-45 days. Incomplete documents or missing information can extend timelines to 90 days or more.
Does Medicare pay for rides to dialysis?
No. Original Medicare doesn’t cover routine rides to dialysis. It only pays for ambulance transport in rare cases when a doctor certifies it’s medically necessary. However, some Medicare Advantage plans offer transportation as an extra benefit.
How do I get free transportation to dialysis?
If you have Medicaid, you qualify for free rides through your state’s program. Call your state’s Medicaid transportation broker with your member ID. If you don’t have Medicaid, contact the American Kidney Fund at 1-800-638-8299 or ask your dialysis social worker about local programs.
Who pays for dialysis transportation?
Medicaid is the primary payer for most dialysis transportation through state brokers. Medicare only covers ambulances in rare circumstances. For patients with Medicare Advantage, some plans offer limited transportation benefits. About half of dialysis patients have both Medicare and Medicaid.
How often do dialysis patients need rides?
Patients on in-center hemodialysis typically need rides three times a week, every week. That adds up to about 156 one-way trips each year. This is why dialysis creates the highest transportation volume of any chronic condition.
What’s the phone number for Medicaid transportation?
It varies by state. For Texas, call Modivcare at 866-424-0147. For Florida, call MTM at 844-239-5974. Your dialysis center’s social worker will have the correct number for your state.
Can I use Uber to get to dialysis?
You can, but it has limitations. Uber works for ambulatory patients but has very limited wheelchair access. For three weekly trips, the cost adds up quickly. A better option is Uber Health, which clinics can book for medical appointments at potentially lower rates.
What if I miss dialysis because of transportation?
Missing a treatment is serious—it can cause fluid overload and lead to hospitalization. If you think you might miss your appointment due to transportation issues, call your dialysis clinic immediately. The social worker can often arrange emergency transportation.
How much do NEMT companies get paid for dialysis trips?
Payments range from $25-$90 for standard rides and $50-$150 for wheelchair vans, plus mileage. A single wheelchair patient can generate $11,700 or more in annual revenue. Dialysis patients typically remain on service for 5-10 years.
What’s the billing code for dialysis wheelchair transport?
The standard HCPCS code for a wheelchair van trip is T2007 or A0130. You must add a modifier like RD to show the trip was from a residence to a dialysis center, and use diagnosis code N18.6 for ESRD.
How do I become a dialysis transportation provider?
First, enroll with your state’s Medicaid program. Then get credentialed with the NEMT broker in your state—usually Modivcare or MTM. You’ll need to submit insurance certificates, vehicle inspections, and driver background checks. The process takes 30 to 60 days.
What if my dialysis ride is late?
Call the broker’s support line right away—they can track the driver’s location and send a backup if needed. Also, inform your dialysis clinic so they know you’re coming. Most clinics can accommodate late arrivals if you let them know.
How do I set up recurring rides to dialysis?
Ask your dialysis social worker to submit a standing order to the transportation broker. This form, signed by your doctor, authorizes automatic scheduling for your regular treatment days. Once approved, you won’t need to call for each appointment.
Where can I get help with dialysis transportation?
Start with your dialysis social worker—they know local resources. You can also call the American Kidney Fund at 1-800-638-8299, the Eldercare Locator at 1-800-677-1116 if you’re 60 or older, or dial 211 for community resources in your area.
How long does a dialysis appointment take?
A typical dialysis session lasts 3 to 5 hours. Your return ride should be scheduled about 30 to 60 minutes after your appointment time to allow for treatment completion and recovery time.
Can I use a wheelchair van for dialysis?
Yes, if you need one. Your doctor must certify that you require wheelchair transportation due to mobility limitations. Once documented, the broker will dispatch a wheelchair-accessible vehicle with a ramp or lift.
What does EVV mean for NEMT?
EVV stands for Electronic Visit Verification. It’s a system that tracks when and where transportation services happen using GPS and timestamps. It’s required by law for Medicaid trips in most states to prove services were provided.
How much can I make transporting dialysis patients?
A single wheelchair dialysis patient can generate $11,700 or more per year in revenue. Ambulatory patients bring in about $5,400 annually. With patients staying on service for 5-10 years, the lifetime value is significant.
Why do dialysis NEMT claims get denied?
The most common reasons are expired authorizations, patient eligibility problems, missing documentation, and wrong billing codes. Checking authorization status and eligibility before every trip prevents most denials.
Key Takeaways
Dialysis transportation represents both the highest-volume opportunity and one of the most complex billing challenges in NEMT. Success requires understanding several interconnected systems:
For Patients:
- Medicaid covers dialysis transportation as a mandatory benefit—you have this right
- Medicare does NOT cover routine rides; only Medicaid or Medicare Advantage supplemental benefits do
- Your dialysis social worker is your most important advocate and resource navigator
- Standing orders eliminate the need to call for every trip—ask your clinic to set one up
For Providers:
- Dialysis generates predictable, recurring revenue ($8,000-$15,000/patient/year)
- Operational efficiency—not higher rates—determines profitability
- Compliance with EVV mandates and credentialing requirements is non-negotiable
- Building clinic partnerships creates sustainable volume and referral networks
- Professional billing support significantly impacts clean claim rates and cash flow
Whether you’re a patient navigating coverage options or a provider building dialysis transportation services, the complexity of this space rewards expertise. Organizations like EliteMed Financials specialize in helping NEMT providers master billing, compliance, and operational efficiency—turning the complexity of dialysis transportation into sustainable business success.
This guide is provided for informational purposes and reflects regulations and industry practices as of January 2026. State Medicaid programs, broker requirements, and Medicare Advantage benefits change periodically. Always verify current rules with your state Medicaid agency, broker, or insurance plan. For personalized guidance on NEMT billing challenges, consult with qualified healthcare billing professionals.

