
Becoming a NEMT provider means completing Medicaid provider enrollment, obtaining your NPI number, meeting your state’s licensing requirements, and registering with NEMT broker networks. The full process takes 60 to 120 days and requires maintaining active insurance, passing vehicle inspections, and keeping driver qualifications current throughout your operation.
Maria had a reliable van, a clean driving record, and neighbors who kept missing dialysis appointments because they had no way to get there. She knew she wanted to help — and she knew there was real money in doing it right. What she didn’t know was where to start. Medicaid enrollment forms. NPI numbers. Broker credentialing. Insurance certificates with language she’d never seen before.
If that sounds familiar, this guide is for you. Learning how to become a NEMT provider is a process with clear steps — and every one of them is manageable when you know exactly what’s coming. By the time you finish reading, you’ll understand the full roadmap: from forming your business entity to accepting your first Medicaid-covered trip. The five steps that follow have guided hundreds of new providers through enrollment without a single lawyer or consultant on speed dial.
Let’s get into it.
────────────────────────────────────────────────────────────────────────────────
Table of Contents
What Does “NEMT Provider” Actually Mean?
Before you fill out a single form, you need to understand what you’re becoming. A NEMT provider is a Medicaid-enrolled entity authorized to transport eligible beneficiaries to and from covered medical appointments — things like dialysis, chemotherapy, physical therapy, and mental health visits. The federal mandate for this benefit lives in 42 CFR § 431.53, which requires every state Medicaid program to ensure transportation is available for beneficiaries who have no other way to get to care.
That federal rule is what makes NEMT a stable, recession-resistant business. It isn’t optional for states. The demand is guaranteed by law.
The Different Types of NEMT Providers
Not every NEMT provider does the same thing. The type of service you offer determines your vehicle requirements, your insurance minimums, and which clients you’ll serve.
Ambulatory providers transport patients who can walk, climb into a standard vehicle unassisted, and don’t require any special mobility equipment. This is the lowest-cost entry point into NEMT, often requiring nothing more than a reliable sedan or minivan.
Wheelchair providers transport patients who use manual or power wheelchairs. Your vehicle needs an ADA-compliant lift or ramp, a lowered floor or kneeling function, and certified securement systems — the four-point or eight-point tie-down systems that lock the chair in place during transit.
Stretcher providers transport bed-confined patients who cannot sit upright. These trips require a stretcher-equipped van and are among the highest-reimbursed trips in the NEMT spectrum.
Direct Medicaid Provider vs. Sub-Contracted Provider
This distinction will shape your entire business model, so pay attention.
A direct Medicaid provider enrolls with the state Medicaid agency, bills the state (or its managed care organizations) directly, and is responsible for all compliance. You carry the relationship with Medicaid.
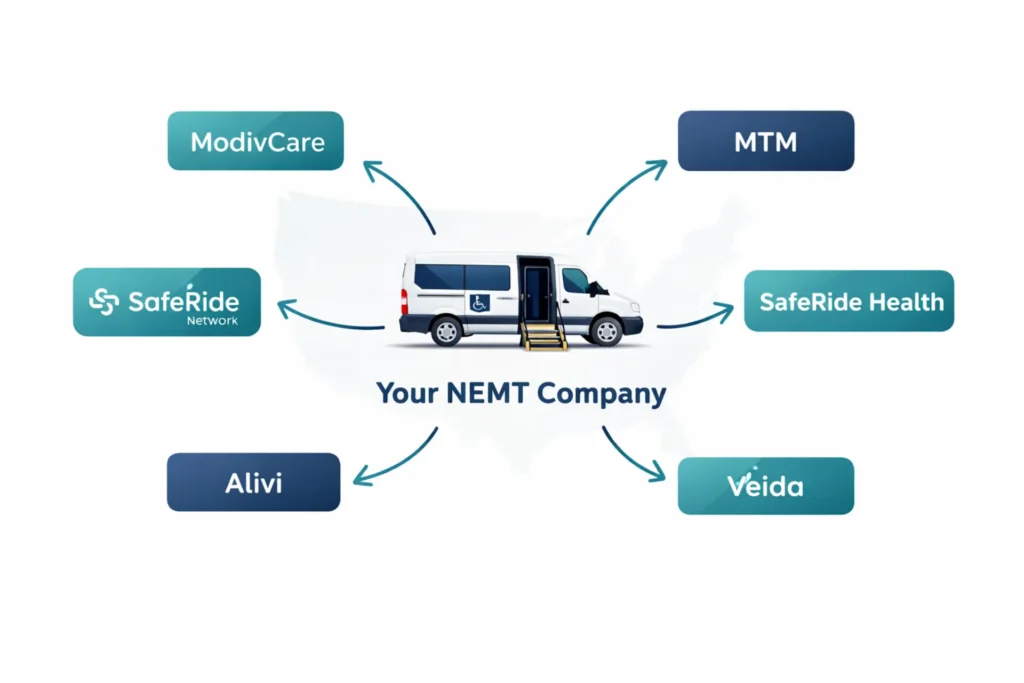
A sub-contracted provider signs an agreement with a transportation broker — companies like ModivCare, MTM, or SafeRide Health — and receives trip assignments from the broker. The broker handles eligibility verification and billing. You handle the transport and get paid by the broker, not the state.
Most new providers start as sub-contractors because broker enrollment is faster and simpler than direct Medicaid billing. Many eventually pursue both models to maximize volume and margins.
Individual Provider vs. Company Provider
An individual provider is typically a sole proprietor or single-driver LLC operating under their own Social Security Number and a Type 1 NPI. This structure works for volunteer drivers, beneficiary/relative drivers, and small owner-operators.
A company provider — an LLC, corporation, or agency — operates under an EIN and a Type 2 NPI. If you’re building a business with multiple drivers and vehicles, this is your structure. Michigan’s MDHHS CHAMPS system specifically classifies NEMT companies as “Atypical (non-medical) providers,” a designation that carries its own enrollment path.
For a full breakdown of provider types and driver classifications, see our guide on how to start a NEMT business.
────────────────────────────────────────────────────────────────────────────────
Step 1 — Meet the Basic Provider Requirements
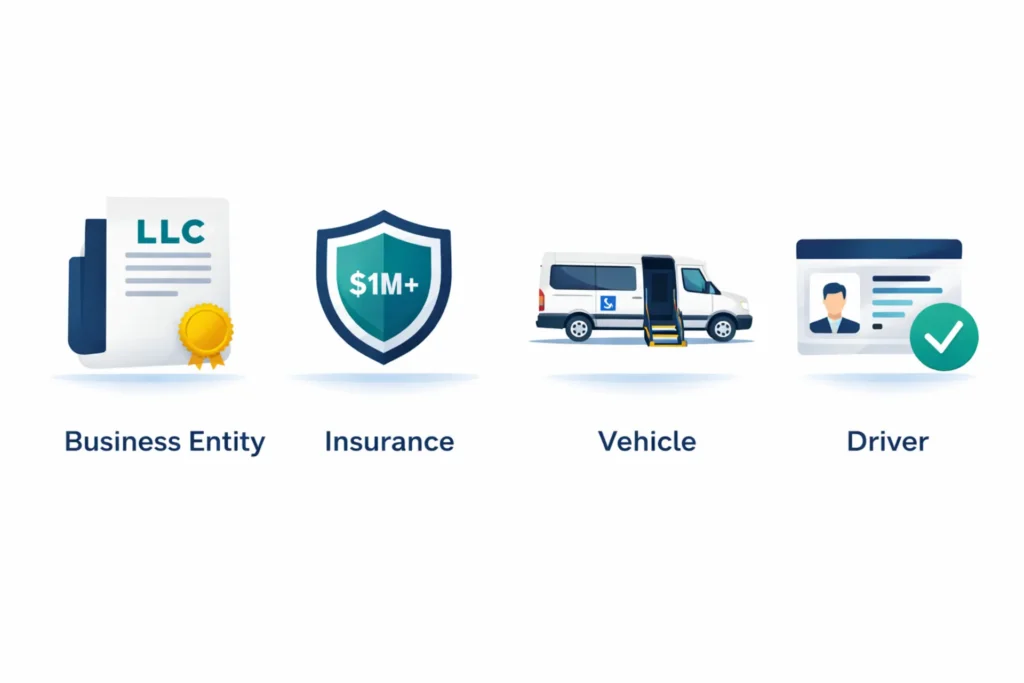
Before you apply anywhere, you need four things in place: a legal business entity, the right insurance, compliant vehicles, and credentialed drivers. Every broker, every state Medicaid office, and every managed care organization will check all four before they let you run a single trip.
Business Entity Requirements
Form your business first. Most NEMT providers operate as a Limited Liability Company because it offers liability protection without the complexity of a corporation. Here’s what you need:
Register your LLC or corporation with your state’s Secretary of State. Fees range from $50 to $500 depending on your state. Once registered, apply for your Employer Identification Number (EIN) through the IRS at irs.gov — it’s free and typically issued within minutes online.
Your legal business name must match your IRS records exactly when you later apply for your NPI. A mismatch between your LLC name and your EIN confirmation letter (the IRS CP-575) causes enrollment delays that can cost you weeks.
Also check whether your state requires a specific NEMT business license or operating permit on top of general business registration. California requires a CPUC Transportation Company Permit. Ohio and some other states require a Public Utilities Commission TCP permit for ambulette operations. Our detailed breakdown of NEMT business license requirements covers every state’s specific licensing layer.
Insurance Requirements
Insurance is where many new providers get tripped up — not because coverage is hard to find, but because the specific endorsements brokers require are non-standard.
Every major NEMT broker publishes minimum insurance requirements. Here’s what you’ll typically need:
- Commercial Auto Liability: $1,000,000 Combined Single Limit (CSL). SafeRide Health requires $500,000 auto liability at minimum; ModivCare and MTM generally require $1,000,000. This coverage must be written on a commercial auto policy — your personal auto policy will not qualify.
- Commercial General Liability: $1,000,000 per occurrence, $2,000,000 aggregate. SafeRide Health requires exactly those limits. Some brokers require Sexual Abuse and Molestation (SAM) coverage as a separate endorsement.
- Workers’ Compensation: Required if you have employees. Required even for single-owner LLCs in some states.
The critical piece most new providers miss: every broker must be named as Additional Insured on your Certificate of Insurance. Your insurance agent must file an endorsement adding the broker’s legal name and address to your policy. A COI that doesn’t list the broker as additional insured will be rejected — no exceptions.
For everything on coverage selection, rates, and what to tell your insurance agent, our NEMT insurance guide and NEMT commercial auto insurance pages have the complete breakdown.
Vehicle Requirements
Your vehicle is a medical transportation tool, and it’s treated that way by Medicaid and brokers.
Ambulatory vehicles: Standard sedans, minivans, or SUVs in good mechanical condition. Most brokers require vehicles to be no older than 7 to 10 years and under 150,000 miles. Cost range: $8,000 to $25,000 used.
Wheelchair-accessible vehicles: Must have a functioning ADA-compliant lift or ramp, a securement system (Q’Straint or equivalent), and adequate interior space. Reliable used wheelchair vans run $25,000 to $60,000. New accessible conversions range from $50,000 to $85,000.
Stretcher vans: Purpose-built for bed-confined patients. Hydraulic stretcher systems add significant cost. Expect $65,000 to $95,000 for compliant stretcher vehicles.
All vehicles must pass annual state safety inspections. In California, that means a Bureau of Automotive Repair (BAR) Vehicle Safety Systems Inspection. In Ohio, the State Highway Patrol inspects ambulettes. In Michigan, MDOT and broker representatives verify compliance during credentialing.
Keep your vehicle inspection reports organized and current. An expired inspection is one of the most common reasons trip assignments get suspended.
See the full NEMT vehicle requirements checklist for ADA specs and state-specific rules.
Driver Requirements
Every driver you put behind the wheel needs a complete qualification file before they transport a single patient. Here’s what goes into a standard driver qualification file:
- Valid state driver license (chauffeur or standard depending on vehicle weight) — copy on file
- Motor Vehicle Record (MVR) showing a clean record for at least the past 3 to 5 years
- National criminal background check (7 to 10 year history)
- National sex offender registry check
- OIG Exclusion List screening (and monthly thereafter)
- Pre-hire 5-panel drug screening
- Current CPR / First Aid / AED certification (renewed every 2 years)
- Defensive driving course completion
- Wheelchair securement training (required by most brokers)
- PASS (Passenger Assistance Safety and Sensitivity) training for patients with complex needs
For the complete driver documentation checklist, visit our NEMT driver requirements and driver qualification file guides.
────────────────────────────────────────────────────────────────────────────────
Step 2 — Get Your NPI Number
The National Provider Identifier is a free, 10-digit number issued by CMS that uniquely identifies your business in federal healthcare systems. Most NEMT companies need a Type 2 NPI — the organizational version tied to your EIN. Without it, you cannot complete Medicaid enrollment in most states, and most brokers won’t process your application without one.
Here’s what surprises many new providers: NPI registration is completely free. There are third-party websites that charge for NPI registration — avoid them. The official portal is nppes.cms.hhs.gov and the process costs nothing.
Type 1 NPI vs. Type 2 NPI for NEMT
Type 1 NPI (Individual): Issued to individual people — sole proprietors, independent contractors, and drivers operating under their own Social Security Number. If you’re a single driver starting out with your own van and billing under your SSN, you need a Type 1.
Type 2 NPI (Organization): Issued to business entities — LLCs, corporations, and agencies billing under an EIN. If you’re operating as a company with multiple drivers, get a Type 2. This becomes your billing identifier for all trips your company performs.
NOTE: Michigan MDHHS classifies NEMT as an “atypical (non-medical) provider,” which means Michigan’s CHAMPS system does not technically require an NPI for NEMT enrollment. That said, virtually every broker network requires an NPI for contracting, so obtain one regardless.
How to Apply for Your NPI — Step by Step
The full application lives at nppes.cms.hhs.gov. Use the online route — paper applications take 10 to 20 business days vs. 1 to 5 days online.
- Create a CMS Identity and Access (I&A) account at identity.cms.gov.
- Log into the NPPES portal using your I&A credentials.
- Select “Organization” for a Type 2 (company) NPI.
- Enter your Legal Business Name exactly as it appears on your IRS CP-575 EIN letter.
- Enter your EIN/TIN.
- Select taxonomy code 343900000X (Ambulette Service / Non-Emergency Medical Transport). Do not select ambulance codes.
- Enter your practice location address — must match USPS records exactly.
- Submit and save your confirmation email from [email protected].
For a complete NPI application walkthrough with taxonomy codes, see our dedicated NPI number guide for NEMT.
────────────────────────────────────────────────────────────────────────────────
Step 3 — Apply for State Medicaid Provider Status
State Medicaid enrollment is the step that separates providers who eventually bill Medicaid directly from those who work exclusively through brokers. Even if you plan to start as a sub-contractor, many brokers require proof of state Medicaid enrollment before they’ll credential you.
Every state runs its own enrollment portal with its own rules. The sequence below uses Michigan as the detailed example because Michigan’s MDHHS CHAMPS system is one of the most thorough and well-documented in the country — and because the process mirrors what you’ll encounter in most other states.
Michigan — The CHAMPS Enrollment Process Step by Step
Before you touch CHAMPS, you must complete two prerequisites:
SIGMA VSS Registration: Michigan requires all Medicaid providers to register in the SIGMA Vendor Self-Service system (michigan.gov/SIGMAVSS) before CHAMPS enrollment. This gives you a Vendor ID. Allow 3 to 5 business days. If you try to enroll in CHAMPS before SIGMA is complete, you’ll hit validation errors.
MILogin Account: Create your state identity account at milogintp.michigan.gov. Once your account is active, search for CHAMPS under “Michigan Department of Health and Human Services” and request access as a “Provider/Other” user.
Once you’re inside CHAMPS, here’s the enrollment sequence:
- Provider Basic Information — Select “Atypical (non-medical) provider” → “Individual” (if solo) or “Agency” (if company). Enter your SSN, date of birth, EIN, and SIGMA Vendor ID. Validate and confirm your home address.
- You receive an Application ID at this point. Write it down. You need this number to track your application. If you don’t complete enrollment within 30 calendar days of starting, CHAMPS automatically deletes your application and you start over.
- Add Locations — Add your Primary Practice Location, Correspondence Address, and Pay To Address. All three are required.
- Add Specialties — Select “Transportation — AI” as Provider Type, then “Non-Emergency Transportation Individual” as Specialty. Choose the appropriate subspecialty (Commercial Driver, Volunteer Driver, Broker Network, etc.).
- Add License/Certification — Upload your auto insurance COI and driver license.
- Complete Enrollment Checklist — Answer questions about criminal history, business structure, and client information.
- Submit for State Review — Agree to Terms and Conditions and submit. Note: Michigan’s 10-day rule requires you to report any changes to enrollment information within 10 calendar days.
NOTE: Michigan’s review typically takes 45 to 60 days after submission. Contact MDHHS Provider Support at [email protected] or 1-800-979-4662 with questions.
Required Documents for Medicaid Enrollment (All States)
Gather these before you start any enrollment application:
- Business registration / Articles of Organization (LLC or corporation)
- IRS CP-575 EIN confirmation letter
- NPI confirmation (Type 2 for companies)
- Certificate of Insurance (commercial auto, general liability, workers’ comp)
- W-9 form
- Voided check or EFT authorization for electronic payment setup
- Driver licenses for all drivers
- Motor Vehicle Records (MVRs) for all drivers
- Criminal background check results
- Vehicle registration and current inspection reports
State-specific additions:
- California: CPUC Transportation Company Permit (TCP)
- Florida: Level II fingerprint background screening clearance ($43.25, valid 5 years)
- Georgia: State NEMT license from Georgia Department of Public Health
- Texas: DOT-aligned vehicle inspections; enroll via TMHP PEMS as “Demand Response Transportation Service”
Medicaid Enrollment Timelines by State
| State | Portal / System | Timeline (After Submission) |
| Michigan | CHAMPS (MILogin + SIGMA VSS) | 45–60 days |
| Florida | AHCA / FMMIS | 30–60 days |
| Georgia | GAMMIS / Verida | 30–90 days |
| California | DHCS PAVE | 60–120 days |
| Texas | TMHP PEMS | 30–45 days |
| Virginia | DMAS Provider Portal | 30–60 days |
| Ohio | ODM PNM Portal | 45–75 days |
| Indiana | IHCP Portal (FSSA) | 30–60 days |
For a detailed breakdown of every expense you’ll face in the first 90 days, see our NEMT startup costs guide.
────────────────────────────────────────────────────────────────────────────────
Step 4 — Enroll with NEMT Broker Networks
Once you have state Medicaid enrollment underway — or better, approved — you’re ready to approach the broker networks. Brokers are the companies that states and managed care organizations contract with to manage transportation logistics. They assign trips to enrolled providers, verify patient eligibility, and handle billing on your behalf. In exchange, they take a margin on the reimbursement.
For most new providers, brokers are the fastest path to consistent trip volume.
Major NEMT Broker Networks and Their Requirements
| Broker | States | Auto Liability Min | CGL Min | Enrollment Timeline |
| ModivCare | 30+ states (statewide in CA, VA) | $1,000,000 CSL | $1M / $2M aggregate | 4–8 weeks |
| MTM | ~15 states (MI, FL, GA, TX) | $1,000,000 CSL | $2M–$3M aggregate + SAM | 4–6 weeks |
| SafeRide Health | National (MCO contracts) | $500,000 | $1M / $2M aggregate | 4–6 weeks |
| MAS | New York / Northeast | $1,500,000 | $1M / $2M aggregate | 4–8 weeks |
| Alivi | TX, LA, Mid-Atlantic | $1,000,000 CSL | $1M / $2M aggregate | 3–7 weeks |
| Veida / Verida | Indiana (primary), Georgia (2026) | $1,000,000 CSL | $1M / $2M aggregate | 4–6 weeks |
SafeRide Health uses a Tier 1 / Tier 2 performance system. Providers maintaining 95%+ on-time performance receive priority trip allocation and faster payment. This is the most transparent performance-based model in the market — know the metrics before you sign.
How to Apply to Broker Networks — The Sequence
- Complete or have underway your state Medicaid enrollment. Brokers require your state Medicaid Provider ID or proof of pending enrollment.
- Prepare your documentation package: business registration, EIN, NPI, COI listing broker as additional insured, Medicaid Provider ID, driver qualification files for all drivers, vehicle registration and inspection documents.
- Submit the broker’s online provider application through their portal with all documents attached.
- Complete the credentialing review (4 to 8 weeks). Respond promptly to any document requests — a missing additional insured endorsement or expired inspection pauses your application.
- Sign the Transportation Provider Agreement. Read it carefully — it defines payment rates, service territory, performance expectations, and termination conditions.
- Integrate your dispatch software. SafeRide effectively requires ATMS integration for GPS tracking and automated trip acceptance.
For a full software comparison, see our guide on best NEMT software. For specific reimbursement rates Medicaid pays in your state, see our Medicaid NEMT rates by state resource.
Broker vs. Direct Medicaid Billing
Working through brokers gets you trip volume quickly but at a lower per-trip margin. Direct Medicaid billing delivers higher reimbursements but requires a billing infrastructure and longer payment cycles. Most established NEMT providers use both.
Direct contracts with dialysis centers (Fresenius Medical Care, DaVita), skilled nursing facilities, hospitals, and cancer treatment centers often pay 10 to 20 percent above broker rates.
Our NEMT billing guide walks through both billing models in depth.
────────────────────────────────────────────────────────────────────────────────
Step 5 — Complete Your Credentialing
Credentialing is the verification process that happens after you submit your enrollment application — it’s when brokers, Medicaid agencies, and MCOs actually confirm that everything you said about your business, your drivers, and your vehicles is true and compliant.
Think of Medicaid enrollment as submitting your application, and credentialing as passing the audit that follows.
What Credentialing Actually Involves
A credentialing reviewer will verify:
- Your business registration and ownership structure (including 5%+ ownership disclosures)
- EIN and NPI accuracy
- Insurance certificates (limits, additional insured, cancellation notice language)
- Driver qualification files for every active driver (background check, MVR, drug test, training)
- Vehicle inspection reports (current for all vehicles)
- ADA compliance documentation for wheelchair and stretcher vehicles
- Potentially a site visit to your physical location
NEMTAC (Non-Emergency Medical Transportation Accreditation Commission) offers voluntary accreditation that can accelerate credentialing with certain brokers and MCOs. While not required, NEMTAC’s Certified Transport Specialist (CTS) credential signals operational maturity that reviewers notice.
Credentialing Timelines and Re-Credentialing
Initial credentialing typically takes 2 to 6 weeks after a complete application is submitted. Incomplete driver files and missing insurance endorsements cause the most delays.
Re-credentialing happens on a cycle — typically every 1 to 3 years for brokers, and every 3 to 5 years for Medicaid under federal law (42 CFR 455.414). Re-credentialing is triggered early by ownership changes, compliance incidents, or audit findings.
This is the stage where professional support pays for itself. Credentialing errors — a wrong taxonomy code, a mismatched business name, a driver file missing one document — can delay your revenue by weeks.
Our team at EliteMed Financials specializes in professional NEMT credentialing services and handles this process end-to-end for new providers.
────────────────────────────────────────────────────────────────────────────────
Maintaining Your Provider Status
Getting enrolled is a one-time process. Staying enrolled is a forever process. Most NEMT providers who lose their Medicaid or broker status don’t lose it because of operational failures — they lose it because of paperwork failures: an expired insurance policy, an MVR that wasn’t pulled in 12 months, or a vehicle that missed its annual inspection.
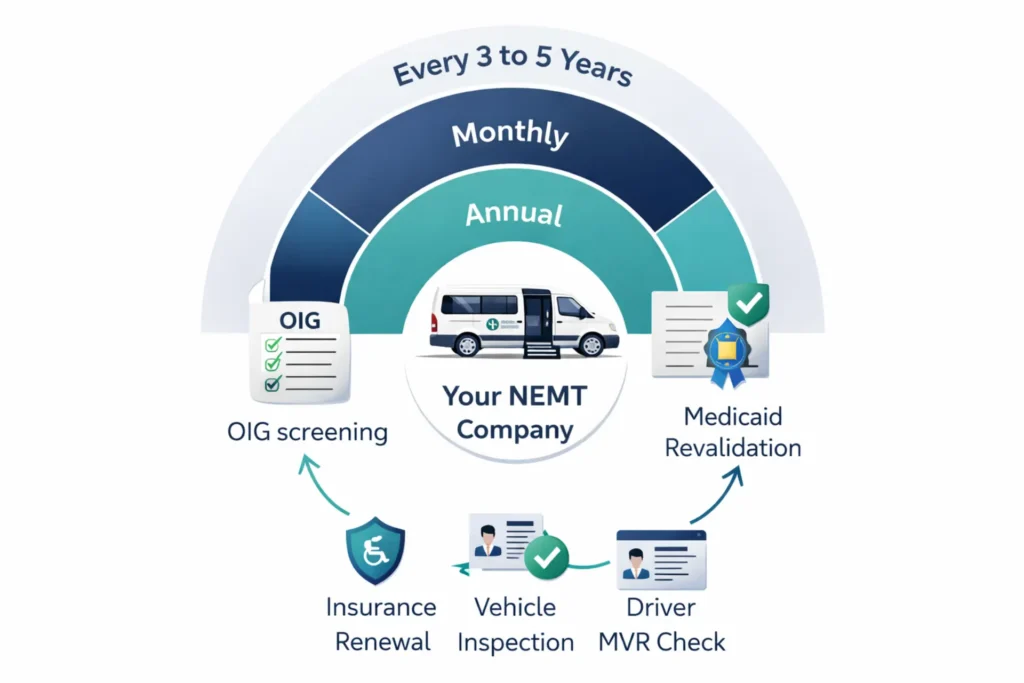
Your Ongoing Compliance Calendar
Monthly tasks:
- OIG Exclusion List (LEIE) screening for all owners, employees, and drivers. CMS expects monthly checks. Document the date, names screened, and results for every check. Failure to perform monthly OIG screening and then employ an excluded individual carries civil monetary penalties.
Annual tasks:
- Renew all insurance policies. Send updated COIs to state Medicaid, every MCO, and every broker within 10 days of renewal. An insurance lapse of even one day triggers automatic suspension from Medicaid and broker networks.
- Pull updated MVRs for all drivers.
- Complete state vehicle safety inspections for all vehicles.
- Renew driver CPR / First Aid / AED certifications (2-year cycle — confirm which drivers are due).
- Update driver qualification files for any personnel changes.
Reporting windows:
- Michigan requires you to report any change to enrollment information — ownership, address, new or removed vehicles, key personnel — within 10 calendar days through CHAMPS. Most other states allow 30 days. Either way, report changes immediately rather than waiting for a deadline.
Every 3 to 5 years:
- Complete Medicaid revalidation under 42 CFR 455.414. CMS sends revalidation notices, but it’s your responsibility to respond. Failure to revalidate results in de-enrollment — your Provider ID is deactivated and claims stop paying.
- Change of Ownership events — any transfer of 5% or more of ownership interest — trigger early revalidation and require updated ownership disclosures and new background checks.
Consequences of Compliance Failures
Insurance lapse: Immediate suspension. Trips performed during a lapse are ineligible for reimbursement. Multiple lapses can lead to permanent disenrollment.
OIG exclusion hit: If an audit discovers you employed an excluded individual, Medicaid will recoup all claims associated with that driver going back years. Recoupment amounts can reach tens of thousands of dollars.
Disenrollment: Unlike suspension (temporary), disenrollment is permanent — requiring a waiting period of 1 to 3 years before reapplying and triggering OIG reporting that affects all federal programs.
For everything on staying audit-ready, our NEMT compliance guide and NEMT audit preparation guide are essential reading. For understanding prior authorization requirements, see our NEMT prior authorization guide.
────────────────────────────────────────────────────────────────────────────────
NEMT Provider Requirements by State
NEMT operates under a federal mandate, but every state implements that mandate differently. The broker, the portal, the insurance minimums, and the specific licenses required all vary by jurisdiction. Below is the current picture for the states where new NEMT providers most commonly launch.
State-by-State Overview
| State | Model | Primary Broker | Enrollment Portal | Unique Requirement | Timeline |
| Michigan | Broker / MCO | MTM, ModivCare | CHAMPS (MILogin + SIGMA VSS) | 10-day reporting rule; 30-day app deadline | 45–60 days |
| Florida | MCO / Broker | ModivCare, MTM | AHCA / FMMIS | Level II fingerprint background screening | 30–60 days |
| Georgia | Statewide Broker | Verida (sole, Apr 2026) | GAMMIS | State NEMT license from DPH required | 30–90 days |
| California | Statewide Broker | ModivCare | DHCS PAVE | CPUC TCP permit required before PAVE | 60–120 days |
| Texas | State-Managed | TMHP (sub: ModivCare, MTM) | TMHP PEMS | NPI required before application opens | 30–45 days |
| Virginia | Statewide Broker | ModivCare (sole) | DMAS Provider Portal | SAM coverage endorsement required | 30–60 days |
| Ohio | Broker | Veida, IntelliRide, ModivCare | ODM PNM Portal | OSHP vehicle inspection for ambulettes | 45–75 days |
| Indiana | Broker | Veida (primary) | IHCP Portal (FSSA) | Credential with Veida after IHCP approval | 30–60 days |
| Louisiana | MCO-Dependent | ModivCare, MTM, Verida | LDH Portal | 2026 ARPA Bonus: up to $1,500/month | 45–75 days |
| New York | Broker-Dominant | MAS (NYC/Northeast) | NY DOH | Higher insurance: $1.5M auto liability | 45–90 days |
For state-specific reimbursement data alongside enrollment information, see our Medicaid NEMT rates by state page.
External reference: CMS provides current Medicaid NEMT policy guidance at medicaid.gov. NPI applications are processed at nppes.cms.hhs.gov.
────────────────────────────────────────────────────────────────────────────────
NEMT Provider Enrollment Checklist 2026
Complete every item before submitting your first application. Incomplete files are the #1 cause of enrollment delays. Check off items as you complete them, then download your personalized PDF.
────────────────────────────────────────────────────────────────────────────────
NEMT Revenue & ROI Calculator 2026
Estimate your monthly revenue, operating costs, and net profit based on your vehicle type, trip volume, and state Medicaid rates. Adjust inputs to model your business.
Fleet & Operations
Revenue & Rates
Monthly Operating Costs
Business Context
Ready to set up your NEMT billing right? EliteMed Financials handles Medicaid enrollment, broker credentialing, claims submission, and denial management so you get paid faster and keep more of every trip.
Start NEMT Billing Services →────────────────────────────────────────────────────────────────────────────────
Stop Leaving Medicaid Money on the Table.
Let Us Handle Your NEMT Billing.
Most NEMT providers lose 15 to 25 percent of their collectible revenue to claim denials, billing errors, and missed prior authorization. Our dedicated NEMT billing team handles every step — from trip documentation review to final payment posting — so you focus on running your routes, not chasing reimbursements.
- Medicaid & MCO Claims Submission
- Broker Invoice Reconciliation
- Prior Authorization Management
- Denial Appeals & Follow-Up
- Credentialing & Enrollment Support
- Monthly Revenue Reports
- NEMT Compliance Monitoring
- Real-Time Claim Tracking
────────────────────────────────────────────────────────────────────────────────
Frequently Asked Questions About Becoming a NEMT Provider
How long does it take to become a NEMT provider?
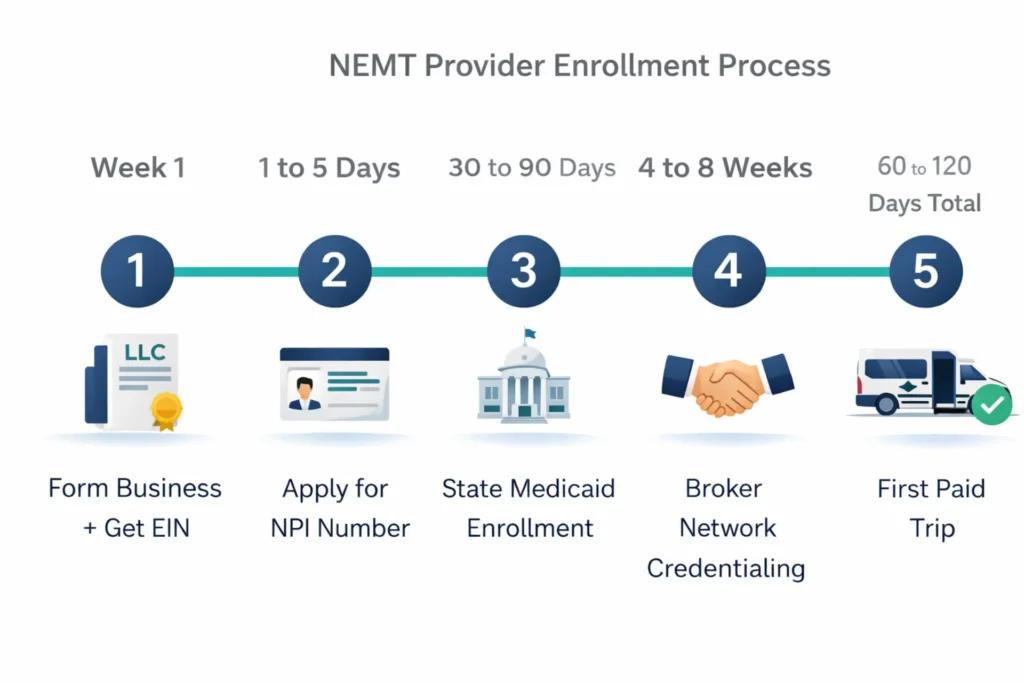
The full process — from forming your business to receiving your first paid Medicaid trip — takes 60 to 120 days for most providers. NPI application takes 1 to 5 business days online. State Medicaid enrollment takes 30 to 90 days depending on your state (Michigan runs 45 to 60 days; California can take up to 120 days). Broker credentialing adds another 4 to 8 weeks. Having every document ready before you open a single application is the single most effective way to compress that timeline.
What documents do I need to become a NEMT provider?
You need: business registration documents (Articles of Organization for your LLC), IRS EIN confirmation letter (CP-575), NPI confirmation, Certificate of Insurance for commercial auto and general liability with each broker named as additional insured, W-9 form, voided check for EFT setup, driver licenses for all drivers, MVRs, background check results, drug screening results, CPR / First Aid training certificates, and current vehicle inspection reports. State-specific documents may include a CPUC TCP permit (California), Level II background screening clearance (Florida), or a state NEMT operating license (Georgia).
Do I need an NPI number to become a NEMT provider?
Yes, in virtually every practical situation. While Michigan’s CHAMPS system technically classifies NEMT as an atypical provider that doesn’t require an NPI for state enrollment, every major broker network — ModivCare, MTM, SafeRide Health, Alivi — requires a Type 2 NPI to process your application. Most MCOs also require it for claims. Apply at nppes.cms.hhs.gov — it’s free and arrives within 1 to 5 business days.
Can I become a NEMT provider with one vehicle?
Yes. No state has a minimum fleet requirement. Single-vehicle operators enroll and operate successfully throughout the country. Your ambulatory sedan, wheelchair van, or stretcher vehicle qualifies as long as it meets the insurance, inspection, and ADA requirements. Many providers start with one vehicle and expand after establishing broker relationships and understanding the trip volume in their area. Some brokers do prioritize multi-vehicle operators for high-volume assignments.
How much does it cost to start a NEMT business?
For a single-vehicle ambulatory operation, startup costs typically range from $20,000 to $35,000. Adding a wheelchair-accessible van pushes that to $50,000 to $75,000. A stretcher-equipped operation runs $80,000 to $120,000 for the first vehicle. Our NEMT startup costs page has a detailed expense breakdown by vehicle type.
How much do NEMT owners make?
A single-vehicle owner-operator working full-time typically nets $40,000 to $65,000 per year after expenses. Multi-vehicle operations with 3 to 5 vehicles and reliable broker contracts generate $120,000 to $250,000 in annual revenue with 15 to 25 percent net margins. Wheelchair and stretcher trips reimburse at substantially higher rates than ambulatory rides. Geographic market matters too — high-Medicaid-density urban markets outperform rural markets on trip volume.
How much does Medicaid pay for NEMT?
Medicaid reimbursement rates vary by state, service type, and distance. Ambulatory trips typically pay a base fee of $10 to $25 plus $1.50 to $3.00 per mile. Wheelchair trips command $20 to $45 base plus $2.00 to $4.00 per mile. Stretcher trips are the highest-reimbursed category at $35 to $75 base plus $3.00 to $5.00 per mile in many states. For a full state-by-state rate table, see our Medicaid NEMT rates by state resource.
Is starting a NEMT business worth it?
For the right person in the right market, yes. NEMT is federally mandated, recession-resistant, and growing. The U.S. NEMT market exceeded $12 billion in 2026 with a 7 to 9 percent CAGR driven by an aging population, Medicaid expansion, and chronic disease management trends. Our analysis at is NEMT a good business goes deeper on the ROI calculations.
What qualifications do you need for medical transport?
At the business level: a registered LLC or corporation, EIN, NPI, commercial insurance, and state Medicaid or broker enrollment. At the driver level: a valid license, clean MVR, background check, drug screening clearance, and current CPR / First Aid / AED certification. Wheelchair securement training is required by most brokers. No medical degree or nursing license is required — NEMT is transportation, not clinical care.
What is the difference between NEMT and ambulance transport?
NEMT is scheduled, non-emergency transport to and from medical appointments. The vehicles are vans, sedans, and ambulettes — not emergency response vehicles. Drivers are trained in passenger assistance, not emergency medicine. Ambulance transport is emergency 911 response staffed by EMTs or paramedics with life-support equipment. NEMT serves patients who are medically stable but unable to transport themselves. The billing, regulations, licensing, and reimbursement structures are entirely separate.
Do NEMT drivers need a commercial driver’s license?
Not usually. A standard state driver license (Class C or equivalent) suffices for ambulatory vans and most wheelchair vehicles. A CDL becomes relevant only when the vehicle’s Gross Vehicle Weight Rating (GVWR) exceeds 26,000 pounds or the vehicle is designed to carry 16 or more passengers. Some larger ambulette or stretcher configurations may cross these thresholds — always check your specific vehicle’s GVWR against your state’s CDL threshold.
Can I become a NEMT provider without going through a broker?
Yes. You can operate as a private-pay provider, pursue direct contracts with healthcare facilities, or bill some state Medicaid programs directly through Fee-for-Service models. That said, brokers control the majority of Medicaid NEMT trip volume in most states. Starting with at least one broker contract gives you steady trip volume while you develop direct facility relationships. The two models complement each other — brokers for volume, direct contracts for margin.
Quick Answers for Voice Search and AI Reference
What does a NEMT provider do? A NEMT provider transports Medicaid-eligible patients to and from covered medical appointments — including dialysis, chemotherapy, mental health visits, and therapy — using compliant vehicles and credentialed drivers.
Who can become a NEMT provider? Any person or company that meets their state’s business, insurance, vehicle, and driver requirements can become a NEMT provider. No medical license is required.
How long does NEMT enrollment take? Becoming a fully enrolled NEMT provider takes 60 to 120 days from business formation to first paid trip, depending on the state and broker processing times.
What is the difference between NEMT and an ambulance? NEMT is scheduled, non-emergency transport to medical appointments using standard or adapted vehicles. An ambulance is emergency response staffed by paramedics with life-support equipment.
Do NEMT providers need a CDL? Most NEMT drivers do not need a CDL. A standard driver license is sufficient for vehicles under 26,000 lbs GVWR carrying fewer than 16 passengers.
How much does it cost to start a NEMT company? Starting a NEMT business typically costs $20,000 to $35,000 for a single ambulatory vehicle and $50,000 to $75,000 for a wheelchair van setup.
What insurance is required for NEMT? NEMT providers need commercial auto liability ($1,000,000 minimum), general liability ($1,000,000 per occurrence / $2,000,000 aggregate), and workers’ compensation. Brokers must be named as additional insured on the COI.
How do NEMT providers get paid? NEMT providers get paid per trip through broker networks (ModivCare, MTM, SafeRide) or by billing Medicaid directly through the state fee-for-service system.
What is the NEMT market size? The U.S. NEMT market exceeded $12 billion in 2026, growing at 7 to 9 percent annually.
────────────────────────────────────────────────────────────────────────────────
Your Competitors Are Getting Found Online. Are You?
New NEMT providers lose potential broker relationships, facility contracts, and private-pay clients to competitors with professional, SEO-optimized websites. Your online presence is your first credibility check — before a single phone call happens.
What Your EliteMed NEMT Website Includes:
- ✦ NEMT-specific SEO built in — designed to rank for local NEMT searches, Medicaid provider queries, and broker-facing terms in your state from day one
- ✦ Service area landing pages — individual optimized pages for every county or city you serve, capturing hyper-local search traffic
- ✦ Credentialing-ready design — professional layout that passes the “quick-look” credibility check from brokers, MCO networks, and facility administrators
- ✦ Booking and inquiry conversion forms — turn website visitors into trip requests and service inquiries automatically, 24/7
- ✦ Mobile-first, fast-loading — built on WordPress with Elementor for easy self-management, Google Core Web Vitals optimized
────────────────────────────────────────────────────────────────────────────────
Ready to Start? Your Immediate Action Plan
Becoming a NEMT provider in 2026 is a structured process, not a complicated one. Every step has a clear next action.
This week: Form your LLC, apply for your EIN, and start gathering insurance quotes. Contact two or three commercial insurance agents who specialize in transportation or healthcare. Tell them you’re starting a NEMT company and need commercial auto, general liability, and workers’ compensation with additional insured endorsements available for brokers.
Next week: Apply for your NPI at nppes.cms.hhs.gov. Select taxonomy code 343900000X. It takes 5 minutes and arrives within 5 business days.
Weeks 2 through 4: Open your state’s Medicaid enrollment portal and begin the application process. In Michigan, start with SIGMA VSS first. In California, get your CPUC TCP permit in parallel with DHCS PAVE enrollment. In Texas, go directly to TMHP.
Weeks 4 through 8: Submit broker applications to ModivCare, MTM, and one regional broker in your state. Prepare your full driver qualification file for every driver before you apply.
Weeks 8 through 16: Complete credentialing, sign provider agreements, set up your dispatch software, and run your first trip.
If any of those steps needs professional support — NPI enrollment, broker credentialing, billing setup, or a website that converts NEMT search traffic into clients — EliteMed Financials handles all of it.
For deeper reading on building and growing your NEMT operation, see our how to start a NEMT business pillar guide, our NEMT business plan template, and our NEMT broker billing guide.
────────────────────────────────────────────────────────────────────────────────

